The immunology of asthma: Asthma phenotypes and their implications for personalized treatment
- PMID: 27499537
- PMCID: PMC4977430
- DOI: 10.1016/j.anai.2016.04.022
The immunology of asthma: Asthma phenotypes and their implications for personalized treatment
Abstract
Objectives: To review current thinking regarding the role of personalized phenotype-driven as opposed to broad guideline-based therapies in asthma and to speculate on the relative contributions of innate (lung) and adaptive (T and B lymphocyte) roles in asthma pathogenesis.
Data sources: PubMed literature review.
Study selections: Articles pertaining to asthma pathogenesis, with emphasis on those that included biotherapeutic interventions.
Results: Current methods allow asthma to be divided into phenotypes characterized by the presence or absence of eosinophilic inflammation. Corticosteroids are likely to be only effective in the context of eosinophilic inflammation. Similarly, interventions with biotherapeutic agents currently available or in development have efficacious only when administered to patients with asthma of relevant phenotypes.
Conclusion: The availability of biotherapeutic agents that target IgE, interleukin (IL) 5, and, in the near future, IL-13 is an exciting vindication of molecular medicine. However, these biotherapeutic agents are only effective when targeted to patients with specific asthma phenotypes. In Promising biotherapeutic targets are the airway epithelial-derived cytokines IL-25, IL-33, and thymic stromal lymphopoietin. Targeting these lung epithelial-derived mediators, instead of products of the adaptive immune system, may be more likely to improve day-to-day asthma symptoms in contrast to agents that target the adaptive immune system, approaches that primarily act to ameliorate asthma exacerbations.
Copyright © 2016 American College of Allergy, Asthma & Immunology. Published by Elsevier Inc. All rights reserved.
Figures

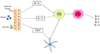



References
-
- Expert Panel Report 3 (EPR-3): Guidelines for the Diagnosis and Management of Asthma-Summary Report 2007. J Allergy Clin Immunol. 2007;120(5 Suppl):S94–S138. - PubMed
-
- Green RH, Brightling CE, Bradding P. The reclassification of asthma based on subphenotypes. Curr Opin Allergy Clin Immunol. 2007;7(1):43–50. - PubMed
-
- Cowan DC, Cowan JO, Palmay R, Williamson A, Taylor DR. Effects of steroid therapy on inflammatory cell subtypes in asthma. Thorax. 2010;65(5):384–390. - PubMed
-
- Nembrini C, Marsland BJ, Kopf M. IL-17-producing T cells in lung immunity and inflammation. J Allergy Clin Immunol. 2009;123(5):986–994. quiz 995–986. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

