Impact of Post-Hospital Syndrome on Outcomes Following Elective, Ambulatory Surgery
- PMID: 27537532
- PMCID: PMC5315678
- DOI: 10.1097/SLA.0000000000001965
Impact of Post-Hospital Syndrome on Outcomes Following Elective, Ambulatory Surgery
Abstract
Objective: The aim of this study was to investigate whether post-hospital syndrome (PHS) places patients undergoing elective hernia repair at increased risk for adverse postoperative events.
Summary of background data: PHS is a transient period of health vulnerability following inpatient hospitalization for acute illness. PHS has been well studied in nonsurgical populations, but its effect on surgical outcomes is unclear.
Methods: State-specific datasets for California in 2011 available through the Healthcare Cost and Utilization Project (HCUP) were linked. Patients older than 18 years who underwent elective hernia repair were included. The primary exposure variable was PHS, defined as any inpatient admission within 90 days of an elective hernia repair performed in an ambulatory surgery center. The primary outcome was an adverse event, defined as any unplanned emergency department visit or inpatient admission within 30 days postoperatively. Mixed-effects logistic models were used for multivariable analyses.
Results: A total of 57,988 patients met inclusion criteria. The 30-day risk-adjusted adverse event rate was significantly higher for PHS patients versus non-PHS patients (11.8% vs 5.8%, P < 0.001). PHS patients were more likely than non-PHS patients to experience postoperative complications (odds ratio 2.2, 95% confidence interval 1.6-3.0). Adverse events attributable to PHS cost an additional $63,533.46 per 100 cases in California. The risk of adverse events due to PHS remained elevated throughout the 90-day window between hospitalization and surgery.
Conclusions: Patients hospitalized within 90 days of an elective surgery are at increased risk of adverse events postoperatively. The impact of PHS on outcomes is independent of baseline patient characteristics, medical comorbidities, quality of center performing the surgery, and reason for hospitalization before elective surgery. Adverse events owing to PHS are costly and represent a quality improvement target.
Conflict of interest statement
The authors report no conflicts of interest.
Figures

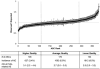


Similar articles
-
Impact of posthospital syndrome on outcomes of elective endovascular repair of abdominal aortic aneurysm.J Vasc Surg. 2020 Nov;72(5):1618-1625. doi: 10.1016/j.jvs.2020.01.063. Epub 2020 Apr 2. J Vasc Surg. 2020. PMID: 32249046
-
Dialysis is an independent risk factor for perioperative adverse events, readmission, reoperation, and mortality for patients undergoing elective spine surgery.Spine J. 2018 Nov;18(11):2033-2042. doi: 10.1016/j.spinee.2018.04.007. Epub 2018 Aug 2. Spine J. 2018. PMID: 30077772
-
Post-hospital syndrome predicts poor postoperative outcomes and increased cost following transvaginal midurethral sling placement.Int Urogynecol J. 2020 Jul;31(7):1417-1422. doi: 10.1007/s00192-019-04009-5. Epub 2019 Jun 13. Int Urogynecol J. 2020. PMID: 31197429
-
Surgeon Gender and Early Complications in Elective Surgery: A Systematic Review and Meta-analysis.Ann Surg. 2025 Mar 1;281(3):404-416. doi: 10.1097/SLA.0000000000006450. Epub 2024 Jul 24. Ann Surg. 2025. PMID: 39045696
-
Medical disease and ambulatory surgery, new insights in patient selection based on medical disease.Curr Opin Anaesthesiol. 2022 Jun 1;35(3):385-391. doi: 10.1097/ACO.0000000000001132. Curr Opin Anaesthesiol. 2022. PMID: 35671030 Review.
Cited by
-
Thirty-day hospital revisits after prostate brachytherapy: who is at risk?Prostate Int. 2019 Jun;7(2):68-72. doi: 10.1016/j.prnil.2018.03.003. Epub 2018 Mar 14. Prostate Int. 2019. PMID: 31384608 Free PMC article.
-
A Path to High-Value Gastric Cancer Surgery Care Delivery.Ann Surg Open. 2024 Mar 29;5(2):e408. doi: 10.1097/AS9.0000000000000408. eCollection 2024 Jun. Ann Surg Open. 2024. PMID: 38911627 Free PMC article.
-
Post-Discharge Services for Different Diagnoses Than Index Hospitalization Predict Decreased 30-Day Readmissions Among Medicare Beneficiaries.J Gen Intern Med. 2019 Sep;34(9):1766-1774. doi: 10.1007/s11606-019-05115-2. Epub 2019 Jun 21. J Gen Intern Med. 2019. PMID: 31228052 Free PMC article.
-
App-based telerehabilitation program for older adults on waiting list for physiotherapy after hospital discharge: a feasibility pragmatic randomized trial.Pilot Feasibility Stud. 2024 Jul 3;10(1):98. doi: 10.1186/s40814-024-01521-4. Pilot Feasibility Stud. 2024. PMID: 38961470 Free PMC article.
-
Same-Day Home Recovery for Benign Foregut Surgery.JAMA Surg. 2022 Sep 14;157(11):1000-6. doi: 10.1001/jamasurg.2022.4245. Online ahead of print. JAMA Surg. 2022. PMID: 36103170 Free PMC article.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

