Usefulness of video-laryngoscopy with the Airway Scope for intubation performance and learning: an experimental manikin controlled study
- PMID: 27566712
- PMCID: PMC5001963
- DOI: 10.1186/s13613-016-0182-0
Usefulness of video-laryngoscopy with the Airway Scope for intubation performance and learning: an experimental manikin controlled study
Abstract
Background: Different video-laryngoscopes (VDLs) for endotracheal intubation (ETI) have recently been developed. We compared the performance of the VDL Airway Scope (AWS) with the direct laryngoscopy by Macintosh (DLM) for ETI success, time and learning.
Methods: We performed an experimental manikin controlled study. Twenty experienced (experts) and 40 inexperienced operators (novices) for DLM-ETI were enrolled. None of them had experience with the use of AWS-VDL. Novices were assigned to start learning with DLM or AWS, and two sub-groups of 20 novices were formed. Experts group constituted the control group. Each participant performed 10 ETI attempts with each device on the same standard manikin. The primary endpoint was the ETI success probability. Secondary endpoints were ETI time, technical validity and qualitative evaluation for each technique. We also assessed the learning order and the successive attempts effects for these parameters.
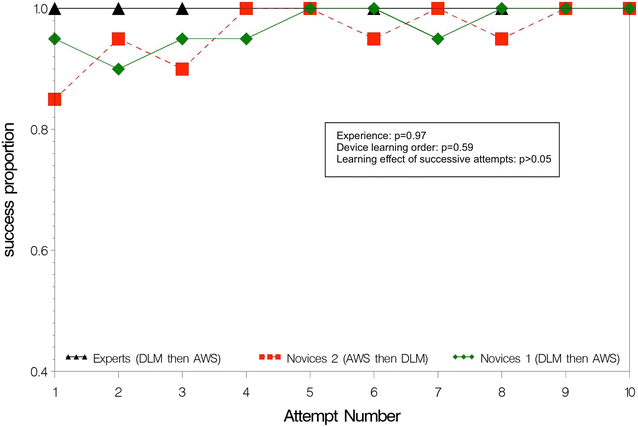
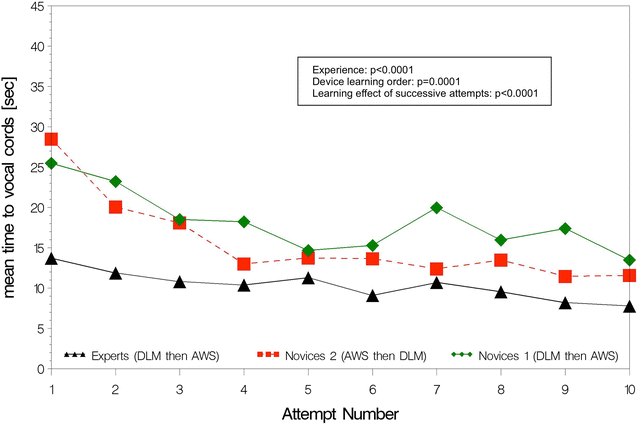
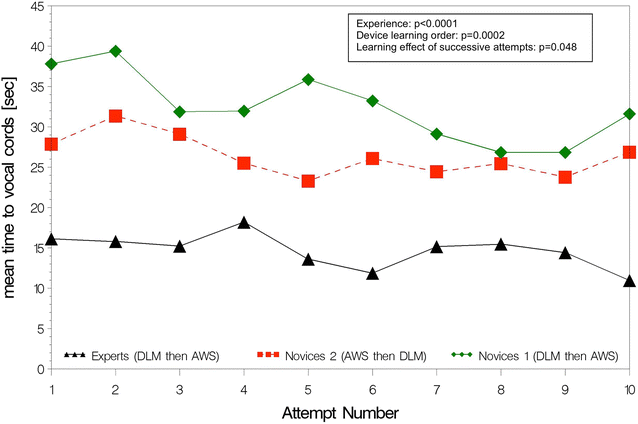
Results: Overall, 1200 ETI attempts were performed. ETI success probability was higher with the AWS than with the DLM for all operators (98 vs. 81 %; p < 0.0001) and for experts compared to novices using devices in the same order (97 vs. 83 %; p = 0.0002). Overall ETI time was shorter with the AWS than with the DLM (13 vs. 20 s; p < 0.0001) and for experts compared to novices using devices in the same order (11 vs. 21 s; p < 0.0001). Among novices, those starting learning with AWS had higher ETI success probability (89 vs. 83 %; p = 0.03) and shorter ETI time (18 vs. 21 s; p = 0.02). Technical validity was found better with the AWS than DLM for all operators. Novices expressed global satisfaction and device preference for the AWS, whereas experts were indifferent.
Conclusions: AWS-VDL permits faster, easier and more reliable ETI compared to the DLM whatever the previous airway ETI experience and could be a useful device for DLM-ETI learning.
Keywords: Airway Scope; Intubation; Learning; Macintosh; Simulation; Video-laryngoscopy.
Figures

Similar articles
-
Evaluation of the Airway Scope, a new video laryngoscope, in tracheal intubation by naive operators: a manikin study.Acta Anaesthesiol Scand. 2007 Nov;51(10):1378-81. doi: 10.1111/j.1399-6576.2007.01450.x. Acta Anaesthesiol Scand. 2007. PMID: 17944642
-
Comparison of results from novice and trained personnel using the Macintosh laryngoscope, Pentax AWS®, C-MAC™ and Bonfils intubation fibrescope: a manikin study.Singapore Med J. 2013 Feb;54(2):64-8. Singapore Med J. 2013. PMID: 23462828
-
Efficacy of Pentax airway scope versus Macintosh laryngoscope when used by novice personnel: A prospective randomized controlled study.J Int Med Res. 2018 Jan;46(1):258-271. doi: 10.1177/0300060517726229. Epub 2017 Aug 23. J Int Med Res. 2018. PMID: 28835153 Free PMC article. Clinical Trial.
-
A comparison of the Glidescope, Pentax AWS, and Macintosh laryngoscopes when used by novice personnel: a manikin study.Can J Anaesth. 2009 Nov;56(11):802-11. doi: 10.1007/s12630-009-9165-z. Epub 2009 Aug 5. Can J Anaesth. 2009. PMID: 19655213 Clinical Trial.
-
Comparison of different video laryngoscopes for emergency intubation in a standardized airway manikin with immobilized cervical spine by experienced anaesthetists. A randomized, controlled crossover trial.Resuscitation. 2012 Jun;83(6):740-5. doi: 10.1016/j.resuscitation.2011.11.024. Epub 2011 Dec 7. Resuscitation. 2012. PMID: 22155448 Clinical Trial.
Cited by
-
Video Laryngoscopy for Endotracheal Intubation: A Consideration for Manual In-Line Stabilization Without Cervical Collar Versus Full Immobilization.Ther Clin Risk Manag. 2025 Jan 25;21:103-109. doi: 10.2147/TCRM.S486978. eCollection 2025. Ther Clin Risk Manag. 2025. PMID: 39882274 Free PMC article.
References
-
- Jaber S, Amraoui J, Lefrant JY, Arich C, Cohendy R, Landreau L, et al. Clinical practice and risk factors for immediate complications of endotracheal intubation in the intensive care unit: a prospective, multiple-center study. Crit Care Med. 2006;34:2355–2361. doi: 10.1097/01.CCM.0000233879.58720.87. - DOI - PubMed
-
- Cook TM, Woodall N, Harper J, Benger J. Major complications of airway management in the UK: results of the Fourth National Audit Project of the Royal College of Anaesthetists and the Difficult Airway Society. Part 2: intensive care and emergency departments. Br J Anaesth. 2011;106:632–642. doi: 10.1093/bja/aer059. - DOI - PubMed
-
- De Jong A, Molinari N, Terzi N, Mongardon N, Arnal J-M, Guitton C, et al. Early identification of patients at risk for difficult intubation in the intensive care unit: development and validation of the MACOCHA score in a multicenter cohort study. Am J Respir Crit Care Med. 2013;187:832–839. doi: 10.1164/rccm.201210-1851OC. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

