Optimal point of insertion of the needle in neuraxial blockade using a midline approach: study in a geometrical model
- PMID: 27570462
- PMCID: PMC4986907
- DOI: 10.2147/LRA.S111569
Optimal point of insertion of the needle in neuraxial blockade using a midline approach: study in a geometrical model
Abstract
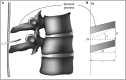
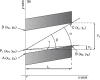
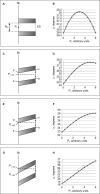
Performance of neuraxial blockade using a midline approach can be technically difficult. It is therefore important to optimize factors that are under the influence of the clinician performing the procedure. One of these factors might be the chosen point of insertion of the needle. Surprisingly few data exist on where between the tips of two adjacent spinous processes the needle should be introduced. A geometrical model was adopted to gain more insight into this issue. Spinous processes were represented by parallelograms. The length, the steepness relative to the skin, and the distance between the parallelograms were varied. The influence of the chosen point of insertion of the needle on the range of angles at which the epidural and subarachnoid space could be reached was studied. The optimal point of insertion was defined as the point where this range is the widest. The geometrical model clearly demonstrated, that the range of angles at which the epidural or subarachnoid space can be reached, is dependent on the point of insertion between the tips of the adjacent spinous processes. The steeper the spinous processes run, the more cranial the point of insertion should be. Assuming that the model is representative for patients, the performance of neuraxial blockade using a midline approach might be improved by choosing the optimal point of insertion.
Keywords: geometrical model; midline approach; neuraxial blockade; optimal point of insertion.
Figures
Similar articles
-
Optimal Point of Insertion and Needle Angle in Neuraxial Blockade Using a Midline Approach: A Study in Computed Tomography Scans of Adult Patients.Reg Anesth Pain Med. 2017 Sep/Oct;42(5):600-608. doi: 10.1097/AAP.0000000000000653. Reg Anesth Pain Med. 2017. PMID: 28796132
-
Predicting the difficult neuraxial block: a prospective study.Anesth Analg. 1999 Aug;89(2):384-9. doi: 10.1097/00000539-199908000-00025. Anesth Analg. 1999. PMID: 10439752
-
[Ultrasound imaging increases first-attempt success rate of neuraxial block in elderly patients].Zhonghua Yi Xue Za Zhi. 2016 Nov 22;96(43):3459-3463. doi: 10.3760/cma.j.issn.0376-2491.2016.43.004. Zhonghua Yi Xue Za Zhi. 2016. PMID: 27903338 Chinese.
-
Recent developments in ultrasound imaging for neuraxial blockade.Curr Opin Anaesthesiol. 2018 Oct;31(5):608-613. doi: 10.1097/ACO.0000000000000634. Curr Opin Anaesthesiol. 2018. PMID: 29994941 Review.
-
Ultrasonography of the adult thoracic and lumbar spine for central neuraxial blockade.Anesthesiology. 2011 Jun;114(6):1459-85. doi: 10.1097/ALN.0b013e318210f9f8. Anesthesiology. 2011. PMID: 21422997 Review.
References
-
- Atallah MM, Demian AD, Shorrab AA. Development of a difficulty score for spinal anaesthesia. Br J Anaesthesia. 2004;92(3):354–360. - PubMed
-
- Guglielminotti J, Mentré F, Bedairia E, Montraves P, Lamgrois D. Development and evaluation of a score to predict difficult epidural placement during labor. Reg Anesth Pain Med. 2013;38(3):233–238. - PubMed
-
- Puolakka R, Haasio J, Pitkänen MT, Kallio M, Rosenberg PH. Technical aspects and postoperative sequelae of spinal and epidural anesthesia: a prospective study of 3,230 orthopedic patients. Reg Anesth Pain Med. 2000;25(5):488–497. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

