Patients with Acute Myeloid Leukemia Admitted to Intensive Care Units: Outcome Analysis and Risk Prediction
- PMID: 27575819
- PMCID: PMC5004890
- DOI: 10.1371/journal.pone.0160871
Patients with Acute Myeloid Leukemia Admitted to Intensive Care Units: Outcome Analysis and Risk Prediction
Erratum in
-
Correction: Patients with Acute Myeloid Leukemia Admitted to Intensive Care Units: Outcome Analysis and Risk Prediction.PLoS One. 2018 Jan 2;13(1):e0190802. doi: 10.1371/journal.pone.0190802. eCollection 2018. PLoS One. 2018. PMID: 29293694 Free PMC article.
Abstract
Background: This retrospective, multicenter study aimed to reveal risk predictors for mortality in the intensive care unit (ICU) as well as survival after ICU discharge in patients with acute myeloid leukemia (AML) requiring treatment in the ICU.
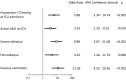
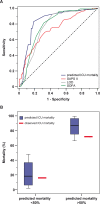
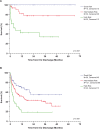
Methods and results: Multivariate analysis of data for 187 adults with AML treated in the ICU in one institution revealed the following as independent prognostic factors for death in the ICU: arterial oxygen partial pressure below 72 mmHg, active AML and systemic inflammatory response syndrome upon ICU admission, and need for hemodialysis and mechanical ventilation in the ICU. Based on these variables, we developed an ICU mortality score and validated the score in an independent cohort of 264 patients treated in the ICU in three additional tertiary hospitals. Compared with the Simplified Acute Physiology Score (SAPS) II, the Logistic Organ Dysfunction (LOD) score, and the Sequential Organ Failure Assessment (SOFA) score, our score yielded a better prediction of ICU mortality in the receiver operator characteristics (ROC) analysis (AUC = 0.913 vs. AUC = 0.710 [SAPS II], AUC = 0.708 [LOD], and 0.770 [SOFA] in the training cohort; AUC = 0.841 for the developed score vs. AUC = 0.730 [SAPSII], AUC = 0.773 [LOD], and 0.783 [SOFA] in the validation cohort). Factors predicting decreased survival after ICU discharge were as follows: relapse or refractory disease, previous allogeneic stem cell transplantation, time between hospital admission and ICU admission, time spent in ICU, impaired diuresis, Glasgow Coma Scale <8 and hematocrit of ≥25% at ICU admission. Based on these factors, an ICU survival score was created and used for risk stratification into three risk groups. This stratification discriminated distinct survival rates after ICU discharge.
Conclusions: Our data emphasize that although individual risks differ widely depending on the patient and disease status, a substantial portion of critically ill patients with AML benefit from intensive care.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures


References
-
- Walter RB, Kantarjian HM, Huang X, Pierce SA, Sun Z, Gundacker HM, et al. Effect of complete remission and responses less than complete remission on survival in acute myeloid leukemia: a combined Eastern Cooperative Oncology Group, Southwest Oncology Group, and M. D. Anderson Cancer Center Study. J Clin Oncol. 2010;28: 1766–1771. 10.1200/JCO.2009.25.1066 - DOI - PMC - PubMed
-
- Krug U, Rollig C, Koschmieder A, Heinecke A, Sauerland MC, Schaich M, et al. Complete remission and early death after intensive chemotherapy in patients aged 60 years or older with acute myeloid leukaemia: a web-based application for prediction of outcomes. Lancet. 2010;376: 2000–2008. 10.1016/S0140-6736(10)62105-8 - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

