MAIT cells: new guardians of the liver
- PMID: 27588203
- PMCID: PMC5007630
- DOI: 10.1038/cti.2016.51
MAIT cells: new guardians of the liver
Erratum in
-
Erratum: MAIT cells: new guardians of the liver.Clin Transl Immunology. 2017 Feb 24;6(2):e132. doi: 10.1038/cti.2017.5. eCollection 2017 Feb. Clin Transl Immunology. 2017. PMID: 28265374 Free PMC article.
Abstract
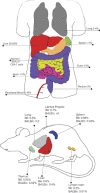
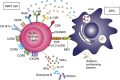
The liver is an important immunological organ that remains sterile and tolerogenic in homeostasis, despite continual exposure to non-self food and microbial-derived products from the gut. However, where intestinal mucosal defenses are breached or in the presence of a systemic infection, the liver acts as a second 'firewall', because of its enrichment with innate effector cells able to rapidly respond to infections or tissue dysregulation. One of the largest populations of T cells within the human liver are mucosal-associated invariant T (MAIT) cells, a novel innate-like T-cell population that can recognize a highly conserved antigen derived from the microbial riboflavin synthesis pathway. MAIT cells are emerging as significant players in the human immune system, associated with an increasing number of clinical diseases of bacterial, viral, autoimmune and cancerous origin. As reviewed here, we are only beginning to investigate the potential role of this dominant T-cell subset in the liver, but the reactivity of MAIT cells to both inflammatory cytokines and riboflavin derivatives suggests that MAIT cells may have an important role in first line of defense as part of the liver firewall. As such, MAIT cells are promising targets for modulating the host defense and inflammation in both acute and chronic liver diseases.
Figures

References
-
- Balmer ML, Slack E, de Gottardi A, Lawson MAE, Hapfelmeier S, Miele L et al. The liver may act as a firewall mediating mutualism between the host and its gut commensal microbiota. Sci Transl Med 2014; 6: 237ra66. - PubMed
-
- Dusseaux M, Martin E, Serriari N, Péguillet I, Premel V, Louis D et al. Human MAIT cells are xenobiotic-resistant, tissue-targeted, CD161hi IL-17-secreting T cells. Blood 2011; 117: 1250–1259. - PubMed
-
- Kenna T, Golden-Mason L, Porcelli SA, Koezuka Y, Hegarty JE, O'Farrelly C et al. NKT cells from normal and tumor-bearing human livers are phenotypically and functionally distinct from murine NKT cells. J Immunol 2003; 171: 1775–1779. - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
