Recurrent stroke risk and cerebral microbleed burden in ischemic stroke and TIA: A meta-analysis
- PMID: 27590288
- PMCID: PMC5075978
- DOI: 10.1212/WNL.0000000000003183
Recurrent stroke risk and cerebral microbleed burden in ischemic stroke and TIA: A meta-analysis
Abstract
Objective: To determine associations between cerebral microbleed (CMB) burden with recurrent ischemic stroke (IS) and intracerebral hemorrhage (ICH) risk after IS or TIA.
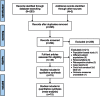
Methods: We identified prospective studies of patients with IS or TIA that investigated CMBs and stroke (ICH and IS) risk during ≥3 months follow-up. Authors provided aggregate summary-level data on stroke outcomes, with CMBs categorized according to burden (single, 2-4, and ≥5 CMBs) and distribution. We calculated absolute event rates and pooled risk ratios (RR) using random-effects meta-analysis.
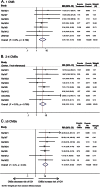
Results: We included 5,068 patients from 15 studies. There were 115/1,284 (9.6%) recurrent IS events in patients with CMBs vs 212/3,781 (5.6%) in patients without CMBs (pooled RR 1.8 for CMBs vs no CMBs; 95% confidence interval [CI] 1.4-2.5). There were 49/1,142 (4.3%) ICH events in those with CMBs vs 17/2,912 (0.58%) in those without CMBs (pooled RR 6.3 for CMBs vs no CMBs; 95% CI 3.5-11.4). Increasing CMB burden increased the risk of IS (pooled RR [95% CI] 1.8 [1.0-3.1], 2.4 [1.3-4.4], and 2.7 [1.5-4.9] for 1 CMB, 2-4 CMBs, and ≥5 CMBs, respectively) and ICH (pooled RR [95% CI] 4.6 [1.9-10.7], 5.6 [2.4-13.3], and 14.1 [6.9-29.0] for 1 CMB, 2-4 CMBs, and ≥5 CMBs, respectively).
Conclusions: CMBs are associated with increased stroke risk after IS or TIA. With increasing CMB burden (compared to no CMBs), the risk of ICH increases more steeply than that of IS. However, IS absolute event rates remain higher than ICH absolute event rates in all CMB burden categories.
© 2016 American Academy of Neurology.
Figures


References
-
- Tanaka A, Ueno Y, Nakayama Y, Takano K, Takebayashi S. Small chronic hemorrhages and ischemic lesions in association with spontaneous intracerebral hematomas. Stroke 1999;30:1637–1642. - PubMed
-
- Knudsen KA, Rosand J, Karluk D, Greenberg SM. Clinical diagnosis of cerebral amyloid angiopathy: validation of the Boston criteria. Neurology 2001;56:537–539. - PubMed
-
- Shoamanesh A, Kwok CS, Benavente O. Cerebral microbleeds: histopathological correlation of neuroimaging. Cerebrovasc Dis 2011;32:528–534. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
