Dexamethasone and supportive care with or without whole brain radiotherapy in treating patients with non-small cell lung cancer with brain metastases unsuitable for resection or stereotactic radiotherapy (QUARTZ): results from a phase 3, non-inferiority, randomised trial
- PMID: 27604504
- PMCID: PMC5082599
- DOI: 10.1016/S0140-6736(16)30825-X
Dexamethasone and supportive care with or without whole brain radiotherapy in treating patients with non-small cell lung cancer with brain metastases unsuitable for resection or stereotactic radiotherapy (QUARTZ): results from a phase 3, non-inferiority, randomised trial
Abstract
Background: Whole brain radiotherapy (WBRT) and dexamethasone are widely used to treat brain metastases from non-small cell lung cancer (NSCLC), although there have been no randomised clinical trials showing that WBRT improves either quality of life or overall survival. Even after treatment with WBRT, the prognosis of this patient group is poor. We aimed to establish whether WBRT could be omitted without a significant effect on survival or quality of life.
Methods: The Quality of Life after Treatment for Brain Metastases (QUARTZ) study is a non-inferiority, phase 3 randomised trial done at 69 UK and three Australian centres. NSCLC patients with brain metastases unsuitable for surgical resection or stereotactic radiotherapy were randomly assigned (1:1) to optimal supportive care (OSC) including dexamethasone plus WBRT (20 Gy in five daily fractions) or OSC alone (including dexamethasone). The dose of dexamethasone was determined by the patients' symptoms and titrated downwards if symptoms improved. Allocation to treatment group was done by a phone call from the hospital to the Medical Research Council Clinical Trials Unit at University College London using a minimisation programme with a random element and stratification by centre, Karnofsky Performance Status (KPS), gender, status of brain metastases, and the status of primary lung cancer. The primary outcome measure was quality-adjusted life-years (QALYs). QALYs were generated from overall survival and patients' weekly completion of the EQ-5D questionnaire. Treatment with OSC alone was considered non-inferior if it was no more than 7 QALY days worse than treatment with WBRT plus OSC, which required 534 patients (80% power, 5% [one-sided] significance level). Analysis was done by intention to treat for all randomly assigned patients. The trial is registered with ISRCTN, number ISRCTN3826061.
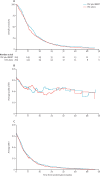
Findings: Between March 2, 2007, and Aug 29, 2014, 538 patients were recruited from 69 UK and three Australian centres, and were randomly assigned to receive either OSC plus WBRT (269) or OSC alone (269). Baseline characteristics were balanced between groups, and the median age of participants was 66 years (range 38-85). Significantly more episodes of drowsiness, hair loss, nausea, and dry or itchy scalp were reported while patients were receiving WBRT, although there was no evidence of a difference in the rate of serious adverse events between the two groups. There was no evidence of a difference in overall survival (hazard ratio 1·06, 95% CI 0·90-1·26), overall quality of life, or dexamethasone use between the two groups. The difference between the mean QALYs was 4·7 days (46·4 QALY days for the OSC plus WBRT group vs 41·7 QALY days for the OSC group), with two-sided 90% CI of -12·7 to 3·3.
Interpretation: Although the primary outcome measure result includes the prespecified non-inferiority margin, the combination of the small difference in QALYs and the absence of a difference in survival and quality of life between the two groups suggests that WBRT provides little additional clinically significant benefit for this patient group.
Funding: Cancer Research UK, Medical Research Council Clinical Trials Unit at University College London, and the National Health and Medical Research Council in Australia.
Copyright © 2016 The Author(s). Published by Elsevier Ltd. This is an Open Access article under the CC BY license. Published by Elsevier Ltd.. All rights reserved.
Figures


Comment in
-
Whole brain radiotherapy in patients with NSCLC and brain metastases.Lancet. 2016 Oct 22;388(10055):1960-1962. doi: 10.1016/S0140-6736(16)31391-5. Epub 2016 Sep 4. Lancet. 2016. PMID: 27604505 No abstract available.
-
Lung cancer: Best supportive care - a reasonable option for patients with brain metastases?Nat Rev Clin Oncol. 2016 Dec;13(12):722-724. doi: 10.1038/nrclinonc.2016.179. Epub 2016 Nov 8. Nat Rev Clin Oncol. 2016. PMID: 27824047 No abstract available.
-
Whole brain radiotherapy for brain metastases.BMJ. 2016 Dec 5;355:i6483. doi: 10.1136/bmj.i6483. BMJ. 2016. PMID: 27920008 No abstract available.
-
Whole brain radiotherapy for brain metastases from non-small cell lung cancer: the end of an era?J Thorac Dis. 2016 Nov;8(11):E1525-E1527. doi: 10.21037/jtd.2016.11.41. J Thorac Dis. 2016. PMID: 28066650 Free PMC article. No abstract available.
-
Whole brain radiotherapy for non-small cell lung cancer.Lancet. 2017 Apr 8;389(10077):1394-1395. doi: 10.1016/S0140-6736(17)30895-4. Lancet. 2017. PMID: 28402816 No abstract available.
-
Whole brain radiotherapy for non-small cell lung cancer.Lancet. 2017 Apr 8;389(10077):1395. doi: 10.1016/S0140-6736(17)30894-2. Lancet. 2017. PMID: 28402817 No abstract available.
References
-
- Ferlay J, Soerjomataram I, Dikshit R. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer. 2015;136:E359–E386. - PubMed
-
- Law A, Karp DD, Dipetrillo T, Daly BT. Emergence of increased cerebral metastasis after high-dose preoperative radiotherapy with chemotherapy in patients with locally advanced nonsmall cell lung carcinoma. Cancer. 2001;92:160–164. - PubMed
-
- Barnholtz-Sloan JS, Sloan AE, Davis FG, Vigneau FD, Lai P, Sawaya RE. Incidence proportions of brain metastases in patients diagnosed (1973 to 2001) in the Metropolitan Detroit Cancer Surveillance System. J Clin Oncol. 2004;22:2865–2872. - PubMed
-
- Chen AM, Jahan TM, Jablons DM, Garcia J, Larson DA. Risk of cerebral metastases and neurological death after pathological complete response to neoadjuvant therapy for locally advanced nonsmall-cell lung cancer: clinical implications for the subsequent management of the brain. Cancer. 2007;109:1668–1675. - PubMed
-
- Stuschke M, Eberhardt W, Pöttgen C. Prophylactic cranial irradiation in locally advanced non-small-cell lung cancer after multimodality treatment: long-term follow-up and investigations of late neuropsychologic effects. J Clin Oncol. 1999;17:2700–2709. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

