Prescribing of FDA-approved and compounded hormone therapy differs by specialty
- PMID: 27648594
- PMCID: PMC5028143
- DOI: 10.1097/GME.0000000000000683
Prescribing of FDA-approved and compounded hormone therapy differs by specialty
Abstract
Objective: To determine the prescribing patterns of general practitioners (GPs), obstetrician/gynecologists (OB/GYNs), and wellness physicians (WPs) of menopausal hormone therapy (HT) for both compounded (CHT) and Food and Drug Administration (FDA)-approved products, using a survey of US physicians.
Methods: Nine thousand one US physicians were invited to participate in a survey to report on their HT-prescribing patterns. Physicians were eligible if they prescribed HT for at least six patients per month.
Results: The survey was completed by 440 eligible physicians (893 responded of 9,001 invited) including 171 GPs, 170 OB/GYNs, and 84 WPs. Physicians prescribed HT for 15% to 30% of their female patients, with WPs numerically most likely to prescribe HT. Menopausal symptoms were the leading reason for HT prescriptions among all specialties. WPs seemed more likely to prescribe HT for general/cardiovascular health (28%), and for shorter durations, than other specialties. WPs prescribed proportionally more compounded (vs FDA-approved) estrogens/progestogens than GPs or OB/GYNs, but OB/GYNs seemed to prescribe more compounded dehydroepiandrosterone and testosterone (prescribed alone) than did others. OB/GYNs seemed least likely to consider CHT being more safe or effective than FDA-approved HT. Symptom relief was the main determinant of efficacy for all specialties; WPs also used blood (61%) or saliva testing (25%) for dose adjustment.
Conclusions: Although all physician specialties surveyed prescribed HT, differences in prescribing CHT versus FDA-approved formulations by medical specialty/practice seemed to exist. Of those surveyed, OB/GYNs and GPs prescribed proportionally more FDA-approved HT, whereas WPs, similarly, prescribed more CHT. More discussion is needed concerning physicians' decisions to prescribe CHT versus FDA-approved formulations.
Conflict of interest statement
Funding/support: TherapeuticsMD supported the survey, and Jolene Mason, PhD, (Precise Publications, LLC) assisted in medical writing. Financial disclosure/conflicts of interest: G.D.C. consulted pharmaceutical companies including but not limited to TherapeuticsMD. D.F.A. serves as consultant to Shionogi Inc, Agile Therapeutics, AbbVie, Bayer Healthcare, CHEMO, Endoceutics, HRA Pharma, and TEVA, and serves on the Speakers’ Bureau for Agile Therapeutics. S.G. and S.M. are employees of TherapeuticsMD with stock options. B.A.B. is a board member and an employee of TherapeuticsMD with stock options.
Figures



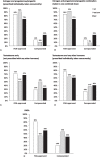
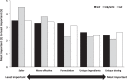

References
-
- Hunter MS, Gentry-Maharaj A, Ryan A, et al. Prevalence, frequency and problem rating of hot flushes persist in older postmenopausal women: impact of age, body mass index, hysterectomy, hormone therapy use, lifestyle and mood in a cross-sectional cohort study of 10,418 British women aged 54-65. BJOG 2012; 119:40–50. - PubMed
-
- Simon JA, Kokot-Kierepa M, Goldstein J, Nappi RE. Vaginal health in the United States: results from the Vaginal Health: Insights, Views & Attitudes survey. Menopause 2013; 20:1043–1048. - PubMed
-
- Rolnick SJ, Jackson J, Kopher R, Defor TA. Provider management of menopause after the findings of the Women's Health Initiative. Menopause 2007; 14:441–449. - PubMed
-
- Blumel JE, Castelo-Branco C, Chedraui PA, et al. Patients’ and clinicians’ attitudes after the Women's Health Initiative study. Menopause 2004; 11:57–61. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

