[Effect of cerebral hemodynamic changes on white matter damage in premature infant with patent ductus arteriosus]
- PMID: 27651194
- PMCID: PMC10396934
- DOI: 10.3785/j.issn.1008-9292.2016.05.10
[Effect of cerebral hemodynamic changes on white matter damage in premature infant with patent ductus arteriosus]
Abstract
Objective: To investigate the effect of cerebral hemodynamic changes on white matter damage in premature infant with patent ductus arteriosus(PDA).
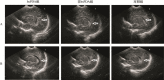
Methods: A total of 106 premature infants were enrolled in the study, including 35 PDA infants with hemodynamic changes (hsPDA group), 35 PDA infants without hemodynamic changes (non-hsPDA group) and 36 non-PDA infants (control group). Serum level of neuron-specific enolase (NES) was detected and craniocerebral ultrasound examination was performed on d3, d7 and d14 after birth. The correlation between blood flow rate of PDA and gray scale value of lateral ventricle was analyzed.
Results: Gray scale values of lateral ventricle and serum levels of NES in hsPDA group were higher than those in control group on d3, d7 and d14 (P<0.01), but no significant difference was observed between non-hsPDA group and control group (P>0.05). There was a positive correlation between the blood flow rate of PDA and gray scale value of lateral ventricle (r=0.876, P<0.01) in premature infants.
Conclusion: Patent ductus arteriosus with hemodynamic changes is closely related to white matter damage in premature infants, and early intervention is necessary.
目的: 探讨血流动力学改变对动脉导管未闭(PDA)早产儿脑白质损伤发生的影响。
方法: 具有血流动力学改变的PDA早产儿35例(hsPDA组)、没有血流动力学改变的PDA早产儿35例(非hsPDA组)、非PDA早产儿36例(对照组)分别于出生后3 d、7 d、14 d检测血清神经特异性烯醇化酶(NSE)的水平,同时进行颅脑超声显像检查,作超声心动图显像PDA血流速度与颅脑超声显像侧脑室灰度值相关性分析。
结果: 出生后3 d、7 d、14 d颅脑超声显像侧脑室灰度值hsPDA组均高于对照组(均 P < 0.01),非hsPDA组与对照组差异均无统计学意义(均 P > 0.05);出生后3 d、7 d、14 d血清NSE水平hsPDA组均高于对照组(均 P < 0.01),非hsPDA组与对照组差异均无统计学意义(均 P > 0.05)。早产儿PDA血流速度大小与超声显像侧脑室灰度值呈正相关( r=0.876, P < 0.01)。
结论: hsPDA早产儿容易发生脑白质损伤,需要及时干预。
Similar articles
-
Transcatheter closure of hemodynamic significant patent ductus arteriosus in 32 premature infants by amplatzer ductal occluder additional size-ADOIIAS.Catheter Cardiovasc Interv. 2017 Oct 1;90(4):612-617. doi: 10.1002/ccd.27091. Epub 2017 May 4. Catheter Cardiovasc Interv. 2017. PMID: 28471089
-
[Clinical characteristics and cardiac hemodynamic changes of patent ductus ateriosus in preterm infants].Zhonghua Er Ke Za Zhi. 2015 Mar;53(3):187-93. Zhonghua Er Ke Za Zhi. 2015. PMID: 26165015 Chinese.
-
Brain and renal oxygenation measured by NIRS related to patent ductus arteriosus in preterm infants: a prospective observational study.BMC Pediatr. 2021 Dec 9;21(1):559. doi: 10.1186/s12887-021-03036-w. BMC Pediatr. 2021. PMID: 34886825 Free PMC article.
-
[Transcatheter occlusion of patent ductus arteriosus in a preterm infant and review of literatures].Zhonghua Er Ke Za Zhi. 2016 Jan;54(1):43-6. doi: 10.3760/cma.j.issn.0578-1310.2016.01.010. Zhonghua Er Ke Za Zhi. 2016. PMID: 26791923 Review. Chinese.
-
Hemodynamic assessment of the patent ductus arteriosus: Beyond ultrasound.Semin Fetal Neonatal Med. 2018 Aug;23(4):239-244. doi: 10.1016/j.siny.2018.04.002. Epub 2018 Apr 27. Semin Fetal Neonatal Med. 2018. PMID: 29730050 Review.
Cited by
-
Clinical efficacy of gangliosides on premature infants suffering from white matter damage and its effect on the levels of IL-6, NSE and S100β.Exp Ther Med. 2019 Jul;18(1):63-68. doi: 10.3892/etm.2019.7539. Epub 2019 May 2. Exp Ther Med. 2019. PMID: 31258638 Free PMC article.
References
-
- HEO M J, LEE O S, LIM S C. Comparative evaluation for the use of oral ibuprofen and intravenous indomethacin in Korean infants with patent ductus. Arch Pharm Res. 2012;35(9):1673–1683. doi: 10.1007/s12272-012-0919-8. [HEO M J, LEE O S, LIM S C. Comparative evaluation for the use of oral ibuprofen and intravenous indomethacin in Korean infants with patent ductus[J]. Arch Pharm Res, 2012, 35(9):1673-1683.] - DOI - PubMed
-
- RICHARDS J, JOHNSON A, FOX G, et al. A second course of ibuprofen is effective in the closure of a clinically significant PDA in ELBW infants. Pediatrics. 2009;124(2):e287–e293. doi: 10.1542/peds.2008-2232. [RICHARDS J, JOHNSON A, FOX G, et al. A second course of ibuprofen is effective in the closure of a clinically significant PDA in ELBW infants[J/OL]. Pediatrics, 2009, 124(2): e287-e293.] - DOI - PubMed
-
- KOCH J, HENSLEY G, ROY L, et al. Prevalence of spontaneous closure of the ductus arteriosus in neonates at a birth weight of 1000 gramsor less. Pediatrics. 2006;117(4):1113–1121. doi: 10.1542/peds.2005-1528. [KOCH J, HENSLEY G, ROY L, et al. Prevalence of spontaneous closure of the ductus arteriosus in neonates at a birth weight of 1000 gramsor less[J]. Pediatrics, 2006, 117(4): 1113-1121.] - DOI - PubMed
-
- SOUL J S, ROBERTSON R L, WYPIJD C, et al. Subtle hemorrhagic brain injury is associated with neuro developmental impairment in infants with repaired congenital heart disease. J Thorac Cardiovasc Surg. 2009;138(2):374–381. doi: 10.1016/j.jtcvs.2009.02.027. [SOUL J S, ROBERTSON R L, WYPIJD C, et al. Subtle hemorrhagic brain injury is associated with neuro developmental impairment in infants with repaired congenital heart disease[J]. J Thorac Cardiovasc Surg, 2009, 138(2): 374-381.] - DOI - PMC - PubMed
-
- 冯 琪, 李 源, 王 颖, et al. 早产儿动脉导管未闭的临床研究. http://cdmd.cnki.com.cn/Article/CDMD-90023-1013123534.htm. 实用儿科临床杂志. 2005;(2):129–131. [冯琪, 李源, 王颖, 等.早产儿动脉导管未闭的临床研究[J].实用儿科临床杂志, 2005, (2): 129-131.]
MeSH terms
LinkOut - more resources
Full Text Sources