Comparison of graft-versus-host disease-free, relapse-free survival according to a variety of graft sources: antithymocyte globulin and single cord blood provide favorable outcomes in some subgroups
- PMID: 27662017
- PMCID: PMC5479609
- DOI: 10.3324/haematol.2016.149427
Comparison of graft-versus-host disease-free, relapse-free survival according to a variety of graft sources: antithymocyte globulin and single cord blood provide favorable outcomes in some subgroups
Abstract
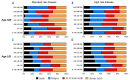
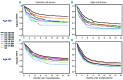
Graft-versus-host disease-free relapse-free survival, which is defined as the absence of grade III-IV acute graft-versus-host disease, systemically treated chronic graft-versus-host disease, relapse, and death, is a novel, meaningful composite end point for clinical trials. To characterize risk factors and differences in graft-versus-host disease-free relapse-free survival according to a variety of graft sources, we analyzed 23,302 patients with hematologic malignancy that had a first allogeneic transplantation from 2000 through 2013 using the Japanese national transplant registry database. The 1-year graft-versus-host disease-free relapse-free survival rate was 41% in all patients. The rate was higher after bone marrow transplantation than after peripheral blood stem cell transplantation due to the lower risks of III-IV acute and chronic graft-versus-host disease. The rate was highest after HLA-matched sibling bone marrow transplantation. The rate after single cord blood transplantation was comparable to that after HLA-matched unrelated bone marrow transplantation among patients aged 20 years or under, and was comparable or better than other alternative graft sources among patients aged 21 years or over, due to the low risk of chronic graft-versus-host disease. Other factors associated with better graft-versus-host disease-free relapse-free survival include female patients, antithymocyte globulin prophylaxis (for standard-risk disease), recent years of transplantation, sex combinations other than from a female donor to a male patient, the absence of prior autologous transplantation, myeloablative conditioning, negative cytomegalovirus serostatus, and tacrolimus-based prophylaxis. These results provide important information to guide the choice of graft sources and are benchmarks for future graft-versus-host disease prophylaxis studies.
Copyright© Ferrata Storti Foundation.
Figures

Similar articles
-
Improved graft-versus-host disease-free, relapse-free survival associated with bone marrow as the stem cell source in adults.Haematologica. 2016 Jun;101(6):764-72. doi: 10.3324/haematol.2015.138990. Epub 2016 Apr 1. Haematologica. 2016. PMID: 27036159 Free PMC article.
-
Comparable composite endpoints after HLA-matched and HLA-haploidentical transplantation with post-transplantation cyclophosphamide.Haematologica. 2017 Feb;102(2):391-400. doi: 10.3324/haematol.2016.144139. Epub 2016 Oct 20. Haematologica. 2017. PMID: 27846611 Free PMC article.
-
[Graft-versus-host disease-free, and relapse-free survival in Japanese patients with hematological malignancies].Rinsho Ketsueki. 2018;59(8):1101-1107. doi: 10.11406/rinketsu.59.1101. Rinsho Ketsueki. 2018. PMID: 30185712 Review. Japanese.
-
Reduced intensity haplo plus single cord transplant compared to double cord transplant: improved engraftment and graft-versus-host disease-free, relapse-free survival.Haematologica. 2016 May;101(5):634-43. doi: 10.3324/haematol.2015.138594. Epub 2016 Feb 11. Haematologica. 2016. PMID: 26869630 Free PMC article. Clinical Trial.
-
Results of unrelated umbilical cord blood hematopoietic stem cell transplant.Transfus Clin Biol. 2001 Jun;8(3):146-54. doi: 10.1016/s1246-7820(01)00132-x. Transfus Clin Biol. 2001. PMID: 11499955 Review.
Cited by
-
Hematopoiesis in the spleen after engraftment in unrelated cord blood transplantation evaluated by 18F-FLT PET imaging.Int J Hematol. 2023 Nov;118(5):618-626. doi: 10.1007/s12185-023-03658-z. Epub 2023 Oct 2. Int J Hematol. 2023. PMID: 37782417 Free PMC article.
-
Clinical relevance of feto-maternal microchimerism in (hematopoietic stem cell) transplantation.Semin Immunopathol. 2024 Dec 7;47(1):4. doi: 10.1007/s00281-024-01028-3. Semin Immunopathol. 2024. PMID: 39644358 Free PMC article. Review.
-
GVHD-free, relapse-free survival provides novel clues for optimizing allogeneic-HSCT for adult T-cell leukemia/lymphoma.Bone Marrow Transplant. 2021 Jan;56(1):155-166. doi: 10.1038/s41409-020-00996-y. Epub 2020 Jul 14. Bone Marrow Transplant. 2021. PMID: 32665675 Free PMC article.
-
Extracorporeal photopheresis with TC-V in Japanese patients with steroid-resistant chronic graft-versus-host disease.Int J Hematol. 2018 Sep;108(3):298-305. doi: 10.1007/s12185-018-2483-6. Epub 2018 Jun 29. Int J Hematol. 2018. PMID: 29959747 Clinical Trial.
-
National Institutes of Health Consensus Development Project on Criteria for Clinical Trials in Chronic Graft-versus-Host Disease: IV. The 2020 Highly morbid forms report.Transplant Cell Ther. 2021 Oct;27(10):817-835. doi: 10.1016/j.jtct.2021.06.001. Epub 2021 Jun 10. Transplant Cell Ther. 2021. PMID: 34217703 Free PMC article.
References
-
- Sankoh AJ, Li H, D’Agostino RB., Sr Use of composite endpoints in clinical trials. Stat Med. 2014;33(27):4709–4714. - PubMed
-
- Schacke H, Docke WD, Asadullah K. Mechanisms involved in the side effects of glucocorticoids. Pharmacol Ther. 2002; 96(1):23–43. - PubMed
-
- Oh H, Loberiza FR, Jr, Zhang MJ, et al. Comparison of graft-versus-host-disease and survival after HLA-identical sibling bone marrow transplantation in ethnic populations. Blood. 2005;105(4):1408–1416. - PubMed
-
- Takahashi S, Ooi J, Tomonari A, et al. Comparative single-institute analysis of cord blood transplantation from unrelated donors with bone marrow or peripheral blood stem-cell transplants from related donors in adult patients with hematologic malignancies after myeloablative conditioning regimen. Blood. 2007;109(3):1322–1330. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

