Long-term outcomes of children treated for Cushing's disease: a single center experience
- PMID: 27678103
- PMCID: PMC5080319
- DOI: 10.1007/s11102-016-0756-8
Long-term outcomes of children treated for Cushing's disease: a single center experience
Abstract
Purpose: Pediatric Cushing's disease (CD) is rare and there are limited data on the long-term outcomes. We assessed CD recurrence, body composition, pituitary function and psychiatric comorbidity in a cohort of pediatric CD patients.
Methods: Retrospective review of 21 CD patients, mean age at diagnosis 12.1 years (5.7-17.8), managed in our center between 1986 and 2010. Mean follow-up from definitive treatment was 10.6 years (2.9-27.2).
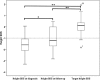
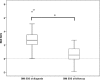
Results: Fifteen patients were in remission following transsphenoidal surgery (TSS) and 5 were in remission following TSS + external pituitary radiotherapy (RT). One patient underwent bilateral adrenalectomy (BA). CD recurrence occurred in 3 (14.3 %) patients: 2 at 2 and 6 years after TSS and 1 7.6 years post-RT. The BA patient developed Nelson's syndrome requiring pituitary RT 0.6 years post-surgery. Short-term growth hormone deficiency (GHD) was present in 14 patients (81 % patients tested) (11 following TSS and 3 after RT) and 4 (44 % of tested) had long-term GHD. Gonadotropin deficiency caused impaired pubertal development in 9 patients (43 %), 4 requiring sex steroid replacement post-puberty. Four patients (19 %) had more than one pituitary hormone deficiency, 3 after TSS and 1 post-RT. Five patients (24 %) had long-term psychiatric co-morbidities (cognitive dysfunction or mood disturbance). There were significant long-term improvements in growth, weight and bone density but not complete reversal to normal in all patients.
Conclusions: The long-term consequences of the diagnosis and treatment of CD in children is broadly similar to that seen in adults, with recurrence of CD after successful treatment uncommon but still seen. Pituitary hormone deficiencies occurred in the majority of patients after remission, and assessment and appropriate treatment of GHD is essential. However, while many parameters improve, some children may still have mild but persistent defects.
Keywords: Cushing’s disease; Outcome; Pediatric; Recurrence.
Conflict of interest statement
The authors declare no conflict of interest. Ethical approval All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors. Informed consent Informed consent was obtained from all individual participants included in the study.
Figures
Similar articles
-
Long-term outcome in patients after treatment for Cushing's disease in childhood.PLoS One. 2019 Dec 12;14(12):e0226033. doi: 10.1371/journal.pone.0226033. eCollection 2019. PLoS One. 2019. PMID: 31830115 Free PMC article.
-
A critical reappraisal of bilateral adrenalectomy for ACTH-dependent Cushing's syndrome.Eur J Endocrinol. 2015 Oct;173(4):M23-32. doi: 10.1530/EJE-15-0265. Epub 2015 May 20. Eur J Endocrinol. 2015. PMID: 25994948 Review.
-
Surgical management of adrenocorticotropic hormone-secreting macroadenomas: outcome and challenges in patients with Cushing's disease or Nelson's syndrome.J Neurosurg. 2005 Nov;103(5):825-30. doi: 10.3171/jns.2005.103.5.0825. J Neurosurg. 2005. PMID: 16304985
-
Management of Cushing's disease: outcome in patients with microadenoma detected on pituitary magnetic resonance imaging.J Neurosurg. 2008 Oct;109(4):751-9. doi: 10.3171/JNS/2008/109/10/0751. J Neurosurg. 2008. PMID: 18826366
-
Cushing's disease.Handb Clin Neurol. 2014;124:221-34. doi: 10.1016/B978-0-444-59602-4.00015-0. Handb Clin Neurol. 2014. PMID: 25248590 Review.
Cited by
-
Pediatric pituitary adenomas.Childs Nerv Syst. 2019 Nov;35(11):2107-2118. doi: 10.1007/s00381-019-04293-y. Epub 2019 Jul 13. Childs Nerv Syst. 2019. PMID: 31302729 Review.
-
Pituitary adenomas evade apoptosis via noxa deregulation in Cushing's disease.Cell Rep. 2022 Aug 23;40(8):111223. doi: 10.1016/j.celrep.2022.111223. Cell Rep. 2022. PMID: 36001971 Free PMC article.
-
Treatment challenges in pediatric Cushing's disease: Review of the literature with particular emphasis on predictive factors for the disease recurrence.Endocrine. 2019 Nov;66(2):125-136. doi: 10.1007/s12020-019-02036-2. Epub 2019 Nov 7. Endocrine. 2019. PMID: 31701434 Free PMC article. Review.
-
The Effects of Sampling Lateralization on Bilateral Inferior Petrosal Sinus Sampling for Pediatric Cushing's Disease-A Single Endocrinology Centre Experience and Review of the Literature.Front Endocrinol (Lausanne). 2021 Apr 19;12:650967. doi: 10.3389/fendo.2021.650967. eCollection 2021. Front Endocrinol (Lausanne). 2021. PMID: 33953696 Free PMC article.
-
Long-term outcome in patients after treatment for Cushing's disease in childhood.PLoS One. 2019 Dec 12;14(12):e0226033. doi: 10.1371/journal.pone.0226033. eCollection 2019. PLoS One. 2019. PMID: 31830115 Free PMC article.
References
-
- Arnaldi G, Angeli A, Atkinson AB, Bertagna X, Cavagnini F, Chrousos GP, Fava GA, Findling JW, Gaillard RC, Grossman AB, Kola B, Lacroix A, Mancini T, Mantero F, Newell-Price J, Nieman LK, Sonino N, Vance ML, Giustina A, Boscaro M. Diagnosis and complications of Cushing’s syndrome: a consensus statement. J Cli Endocrinol Metab. 2003;88(12):5593–5602. doi: 10.1210/jc.2003-030871. - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

