Comparative Effectiveness of Cancer Control and Survival after Robot-Assisted versus Open Radical Prostatectomy
- PMID: 27720782
- PMCID: PMC5568078
- DOI: 10.1016/j.juro.2016.09.115
Comparative Effectiveness of Cancer Control and Survival after Robot-Assisted versus Open Radical Prostatectomy
Abstract
Purpose: Robot-assisted surgery has been rapidly adopted in the U.S. for prostate cancer. Its adoption has been driven by market forces and patient preference, and debate continues regarding whether it offers improved outcomes to justify the higher cost relative to open surgery. We examined the comparative effectiveness of robot-assisted vs open radical prostatectomy in cancer control and survival in a nationally representative population.
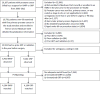
Materials and methods: This population based observational cohort study of patients with prostate cancer undergoing robot-assisted radical prostatectomy and open radical prostatectomy during 2003 to 2012 used data captured in the SEER (Surveillance, Epidemiology, and End Results)-Medicare linked database. Propensity score matching and time to event analysis were used to compare all cause mortality, prostate cancer specific mortality and use of additional treatment after surgery.
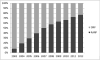
Results: A total of 6,430 robot-assisted radical prostatectomies and 9,161 open radical prostatectomies performed during 2003 to 2012 were identified. The use of robot-assisted radical prostatectomy increased from 13.6% in 2003 to 2004 to 72.6% in 2011 to 2012. After a median followup of 6.5 years (IQR 5.2-7.9) robot-assisted radical prostatectomy was associated with an equivalent risk of all cause mortality (HR 0.85, 0.72-1.01) and similar cancer specific mortality (HR 0.85, 0.50-1.43) vs open radical prostatectomy. Robot-assisted radical prostatectomy was also associated with less use of additional treatment (HR 0.78, 0.70-0.86).
Conclusions: Robot-assisted radical prostatectomy has comparable intermediate cancer control as evidenced by less use of additional postoperative cancer therapies and equivalent cancer specific and overall survival. Longer term followup is needed to assess for differences in prostate cancer specific survival, which was similar during intermediate followup. Our findings have significant quality and cost implications, and provide reassurance regarding the adoption of more expensive technology in the absence of randomized controlled trials.
Keywords: comparative effectiveness research; propensity score; prostatectomy; robotic surgical procedures.
Copyright © 2017 American Urological Association Education and Research, Inc. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
All authors declare they have no potential conflicts of interest.
Figures

References
-
- Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A. Global cancer statistics, 2012. CA: a cancer journal for clinicians. 2015;65(2):87–108. - PubMed
-
- UK PC. About prostate cancer. 2015 http://prostatecanceruk.org/prostate-information/about-prostate-cancer. Accessed Oct 19, 2015.
-
- Hu JC, Gu X, Lipsitz SR, et al. Comparative effectiveness of minimally invasive vs open radical prostatectomy. Jama. 2009;302(14):1557–1564. - PubMed
-
- Audit NPC. First Year Annual Report — Organisation of Services and Analysis of Existing Clinical Data. 2014
-
- Bolenz C, Freedland SJ, Hollenbeck BK, et al. Costs of radical prostatectomy for prostate cancer: a systematic review. European urology. 2014;65(2):316–324. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

