Prenatal Major Depressive Disorder, Placenta Glucocorticoid and Serotonergic Signaling, and Infant Cortisol Response
- PMID: 27763986
- PMCID: PMC6541396
- DOI: 10.1097/PSY.0000000000000410
Prenatal Major Depressive Disorder, Placenta Glucocorticoid and Serotonergic Signaling, and Infant Cortisol Response
Abstract
Objectives: Extending prior studies of prenatal adversity and depressive symptoms, we tested associations between maternal prenatal major depressive disorder (MDD) and infant cortisol regulation. Based on prior findings by our group, we also tested placenta glucocorticoid (HSD11B2 methylation) and serotonin (SLC6A4 gene expression) signaling as moderators of links between prenatal MDD and infant cortisol.
Methods: Participants were 153 mother-infant pairs from a low-income, diverse sample (M [SD] age = 26 [6] years). Repeated structured diagnostic interviews were used to identify mothers with (a) prenatal MDD, (b) preconception-only MDD, and (c) controls. Placenta samples were assayed for HSD11B2 methylation and SLC6A4 gene expression. Infant salivary cortisol response to a neurobehavioral examination was assessed at 1 month.
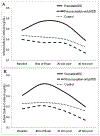
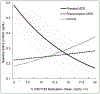
Results: Daughters of prenatal MDD mothers had 51% higher baseline (ratio = 1.51; 95% confidence interval [CI] = 1.01-2.27; p = .045) and 64% higher stress responsive cortisol (ratio = 1.64; 95% CI = 1.05-2.56; p = .03) than daughters of controls and 75% higher stress-responsive cortisol (ratio = 1.75; 95% CI = 1.04-2.94; p = .04) than daughters of preconception-only MDD mothers. HSD11B2 methylation moderated links between prenatal MDD and baseline cortisol (p = .02), with 1% methylation decreases associated with 9% increased baseline cortisol in infants of prenatal MDD mothers (ratio = 1.09; 95% CI = 1.01-1.16). SLC6A4 expression moderated links between prenatal MDD and cortisol response among boys alone (p = .007), with 10-fold increases in expression associated with threefold increases in stress-responsive cortisol (ratio = 2.87; 95% CI = 1.39-5.93) in sons of control mothers.
Conclusions: Results highlight specificity of associations between prenatal versus preconception MDD and cortisol regulation and the importance and complexity of placenta glucocorticoid and serotonergic pathways underlying the intergenerational transmission of risk from maternal adversity.
Figures
References
-
- Gavin NI, Gaynes BN, Lohr KN, Meltzer-Brody S, Gartlehner G, Swinson T. Perinatal depression: a systematic review of prevalence and incidence. Obstet Gynecol. 2005;106:1071–83. - PubMed
-
- Marcus SM, Flynn HA, Blow FC, Barry KL. Depressive symptoms among pregnant women screened in obstetrics settings. J Womens Health (Larchmt). 2003;12:373–80. - PubMed
-
- Le Strat Y, Dubertret C, Le Foll B. Prevalence and correlates of major depressive episode in pregnant and postpartum women in the United States. J Affect Disord. 2011;135:128–38. - PubMed
-
- Grigoriadis S, VonderPorten EH, Mamisashvili L, Tomlinson G, Dennis CL, Koren G, Steiner M, Mousmanis P, Cheung A, Radford K, Martinovic J, Ross LE. The impact of maternal depression during pregnancy on perinatal outcomes: a systematic review and meta-analysis. J Clin Psychiatry. 2013;74:e321–41. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

