Clinical evaluation of thrombotic microangiopathy: identification of patients with suspected atypical hemolytic uremic syndrome
- PMID: 27766045
- PMCID: PMC5056489
- DOI: 10.1186/s12959-016-0114-0
Clinical evaluation of thrombotic microangiopathy: identification of patients with suspected atypical hemolytic uremic syndrome
Abstract
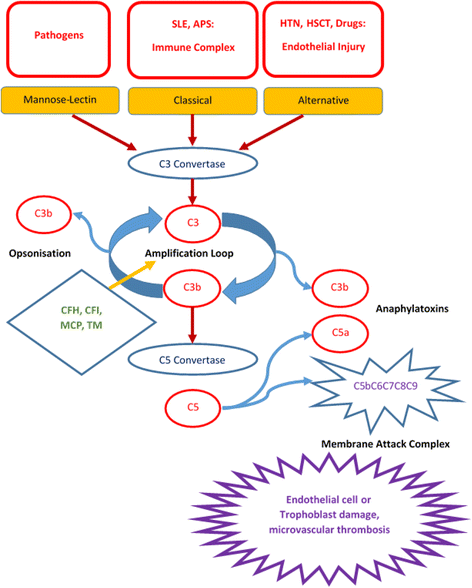
Atypical hemolytic uremic syndrome (aHUS) is a rare genetic disorder caused by defective complement regulation resulting in thrombotic microangiopathy (TMA). Patients can present as children or adults. The syndrome consists of hemolytic anemia with schistocytosis, thrombocytopenia, significant renal damage, and/or other organ system dysfunction(s). Patients with aHUS may succumb to the complications of the disease with the very first manifestation; surviving patients often suffer from progressive organ dysfunction with significant morbidity and mortality despite plasma infusion or plasma exchange. Eculizumab, a humanized monoclonal antibody to C5, was approved for treatment of aHUS in 2011. This is an expensive but highly effective therapy changing the lives and improving the outcome of patients with aHUS. Making timely and accurate diagnosis of aHUS can be life-saving if eculizumab treatment is begun promptly. Finding a genetic mutation in a complement regulatory protein is diagnostic with the appropriate clinical syndrome, but at least 30 % of patients do not have defined or reported mutations. Thus the diagnosis rests on the clinical acumen of the physician. However, the clinical manifestations of aHUS are shared by other etiologies of thrombotic microangiopathy. While laboratory finding of undetectable ADAMTS13 activity defines TTP, distinguishing aHUS from the other causes of TMA remains an art. In addition, aHUS can be unmasked by conditions with enhanced complement activation, such as systemic lupus erythematosus, pregnancy, malignant hypertension, and hematopoietic stem cell transplantation. Thus if TMA occurs in the setting of enhanced complement activation, one must consider aHUS as an underlying etiology, especially if treatment of the condition does not resolve the TMA.
Keywords: Atypical hemolytic uremic syndrome; Complement dysregulation; Thrombotic microangiopathy; Thrombotic thrombocytopenic purpura.
Figures

Similar articles
-
Hemolytic Uremic Syndrome.2023 Oct 19. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2023 Oct 19. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 32310498 Free Books & Documents.
-
Isolated thrombotic microangiopathy of the small intestine in a patient with atypical hemolytic uremic syndrome - a case report.BMC Nephrol. 2020 Mar 24;21(1):104. doi: 10.1186/s12882-020-01766-0. BMC Nephrol. 2020. PMID: 32204691 Free PMC article.
-
Consensus opinion on diagnosis and management of thrombotic microangiopathy in Australia and New Zealand.Nephrology (Carlton). 2018 Jun;23(6):507-517. doi: 10.1111/nep.13234. Nephrology (Carlton). 2018. PMID: 29419916 Review.
-
Treatment of atypical hemolytic uremic syndrome with eculizumab in a patient presenting with neuropsychiatric prodrome: a case report.Front Immunol. 2025 Apr 8;16:1542973. doi: 10.3389/fimmu.2025.1542973. eCollection 2025. Front Immunol. 2025. PMID: 40264782 Free PMC article.
-
Atypical hemolytic uremic syndrome: Review of clinical presentation, diagnosis and management.J Immunol Methods. 2018 Oct;461:15-22. doi: 10.1016/j.jim.2018.07.006. Epub 2018 Jul 19. J Immunol Methods. 2018. PMID: 30031798 Review.
Cited by
-
Pregnancy associated atypical hemolytic uremic syndrome presenting with preeclampsia with HELLP syndrome and following treatment with Eculizumab.Case Rep Perinat Med. 2022 Dec 19;12(1):20220016. doi: 10.1515/crpm-2022-0016. eCollection 2023 Jan. Case Rep Perinat Med. 2022. PMID: 40041263 Free PMC article.
-
Renal histological findings in a patient with acute renal injury associated with purpura fulminans: a case report.J Bras Nefrol. 2019 Apr-Jun;41(2):296-299. doi: 10.1590/2175-8239-jbn-2018-0074. Epub 2018 Sep 13. J Bras Nefrol. 2019. PMID: 30222177 Free PMC article.
-
Case Report: Microangiopathic Hemolytic Anemia With Normal ADAMTS13 Activity.Front Med (Lausanne). 2021 Mar 2;8:589423. doi: 10.3389/fmed.2021.589423. eCollection 2021. Front Med (Lausanne). 2021. PMID: 33738292 Free PMC article.
-
Eculizumab treatment in paediatric patients diagnosed with aHUS after haematopoietic stem cell transplantation: a HSCT-TMA case series from Japanese aHUS post-marketing surveillance.Bone Marrow Transplant. 2024 Mar;59(3):315-324. doi: 10.1038/s41409-023-02161-7. Epub 2023 Dec 15. Bone Marrow Transplant. 2024. PMID: 38102212 Free PMC article.
-
The Centenary of Immune Thrombocytopenia-Part 2: Revising Diagnostic and Therapeutic Approach.Front Pediatr. 2017 Aug 21;5:179. doi: 10.3389/fped.2017.00179. eCollection 2017. Front Pediatr. 2017. PMID: 28871277 Free PMC article. Review.
References
-
- George JN, Nester CM. Syndromes of thrombotic microangiopathy. N Engl J Med. 2014;371(19):1847–8. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

