New Possible Surgical Approaches for the Submammary Adipofascial Flap Based on Its Arterial Supply
- PMID: 27777799
- PMCID: PMC5061926
- DOI: 10.1155/2016/7696010
New Possible Surgical Approaches for the Submammary Adipofascial Flap Based on Its Arterial Supply
Abstract
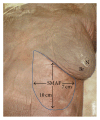
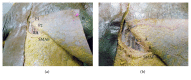
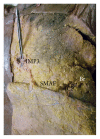
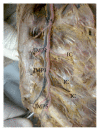
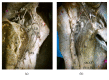
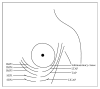
Introduction. Submammary adipofascial flap (SMAF) is a valuable option for replacement of the inferior portion of the breast. It is particularly useful for reconstruction of partial mastectomy defects. It is also used to cover breast implants. Most surgeons base this flap cranially on the submammary skin crease, reflecting it back onto the breast. The blood vessels supplying this flap are not well defined, and the harvest of the flap may be compromised due to its uncertain vascularity. The aim of the work was to identify perforator vessels supplying SMAF and define their origin, site, diameter, and length. Materials and Methods. The flap was designed and dissected on both sides in 10 female cadavers. SMAF outline was 10 cm in length and 7 cm in width. The flap was raised carefully from below upwards to identify the perforator vessels supplying it from all directions. These vessels were counted and the following measurements were taken using Vernier caliper: diameter, total length, length inside the flap, and distance below the submammary skin crease. Conclusions. The perforators at the lateral part of the flap took origin from the lateral thoracic, thoracodorsal, and intercostal vessels. They were significantly larger, longer, and of multiple origins than those on the medial part of the flap and this suggests that laterally based flaps will have better blood supply, better viability, and more promising prognosis. Both approaches, medially based and laterally based SMAF, carry a better prognosis and lesser chance for future fat necrosis than the classical cranially based flap.
Figures





Similar articles
-
The vascular basis of the thoracodorsal artery perforator flap.Plast Reconstr Surg. 2005 Sep;116(3):818-22. doi: 10.1097/01.prs.0000176253.42394.7c. Plast Reconstr Surg. 2005. PMID: 16141821
-
The lateral thoracodorsal flap in breast reconstruction.Plast Reconstr Surg. 1986 Jun;77(6):933-43. doi: 10.1097/00006534-198606000-00010. Plast Reconstr Surg. 1986. PMID: 3714889
-
Perforator Peroneal Artery Flap for Tongue Reconstruction.J Maxillofac Oral Surg. 2017 Mar;16(1):123-126. doi: 10.1007/s12663-016-0933-3. Epub 2016 Jul 11. J Maxillofac Oral Surg. 2017. PMID: 28286397 Free PMC article.
-
Extended thoracodorsal artery perforator flap for breast reconstruction.Gland Surg. 2015 Dec;4(6):519-27. doi: 10.3978/j.issn.2227-684X.2015.04.20. Gland Surg. 2015. PMID: 26645006 Free PMC article. Review.
-
Dynamic InfraRed Thermography (DIRT) in DIEP-flap breast reconstruction: A review of the literature.Eur J Obstet Gynecol Reprod Biol. 2019 Nov;242:47-55. doi: 10.1016/j.ejogrb.2019.08.008. Epub 2019 Aug 23. Eur J Obstet Gynecol Reprod Biol. 2019. PMID: 31563818 Review.
Cited by
-
Subaxillary Replacement Flap Compared with the Round Block Displacement Technique in Oncoplastic Breast Conserving Surgery: Functional Outcomes of a Feasible One Stage Reconstruction.Curr Oncol. 2022 Nov 30;29(12):9377-9390. doi: 10.3390/curroncol29120736. Curr Oncol. 2022. PMID: 36547150 Free PMC article.
-
Posterior intercostal flap: an anatomical study and best flap design.World J Surg Oncol. 2022 Jul 28;20(1):244. doi: 10.1186/s12957-022-02711-1. World J Surg Oncol. 2022. PMID: 35902870 Free PMC article.
-
Reverse Submammary Adipofascial Perforator Flap: Preliminary Results of a Dual-plane, Acellular Dermal Matrix-free, Direct-to-implant Hybrid Reconstruction.Plast Reconstr Surg Glob Open. 2025 Jun 12;13(6):e6847. doi: 10.1097/GOX.0000000000006847. eCollection 2025 Jun. Plast Reconstr Surg Glob Open. 2025. PMID: 40510435 Free PMC article.
References
-
- Jahkola T., Asko-Seljavaara S., Van Smitten K. Immediate breast reconstruction. Scandinavian Journal of Surgery. 2003;92(4):249–256. - PubMed
-
- Dutra A. K., Neto M. S., Garcia É. B., et al. The role of transverse latissimus dorsi musculocutaneous flap immediate breast reconstruction. European Journal of Plastic Surgery. 2009;32(6):293–299. doi: 10.1007/s00238-009-0366-z. - DOI
LinkOut - more resources
Full Text Sources
Other Literature Sources

