Multiple sclerosis animal models: a clinical and histopathological perspective
- PMID: 27792289
- PMCID: PMC8029141
- DOI: 10.1111/bpa.12454
Multiple sclerosis animal models: a clinical and histopathological perspective
Abstract
There is a broad consensus that multiple sclerosis (MS) represents more than an inflammatory disease: it harbors several characteristic aspects of a classical neurodegenerative disorder, that is, damage to axons, synapses and nerve cell bodies. While we are equipped with appropriate therapeutic options to prevent immune-cell driven relapses, effective therapeutic options to prevent the progressing neurodegeneration are still missing. In this review article, we will discuss to what extent pathology of the progressive disease stage can be modeled in MS animal models. While acute and relapsing-remitting forms of experimental autoimmune encephalomyelitis (EAE), which are T cell dependent, are aptly suited to model relapsing-remitting phases of MS, other EAE models, especially the secondary progressive EAE stage in Biozzi ABH mice is better representing the secondary progressive phase of MS, which is refractory to many immune therapies. Besides EAE, the cuprizone model is rapidly gaining popularity to study the formation and progression of demyelinating CNS lesions without T cell involvement. Here, we discuss these two non-popular MS models. It is our aim to point out the pathological hallmarks of MS, and discuss which pathological aspects of the disease can be best studied in the various animal models available.
Keywords: EAE; PPMS; SPMS; cuprizone; disability; disease progression; multiple sclerosis; neurodegeneration; treatment.
© 2016 International Society of Neuropathology.
Conflict of interest statement
The authors report no conflict of interest.
Figures

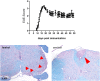
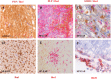


References
-
- Acs P, Kipp M, Norkute A, Johann S, Clarner T, Braun A et al (2009) 17Beta‐estradiol and progesterone prevent cuprizone provoked demyelination of corpus callosum in male mice. Glia 57:807–814. - PubMed
-
- Al‐Izki S, Pryce G, Hankey DJ, Lidster K, von Kutzleben SM, Browne L et al (2014) Lesional‐targeting of neuroprotection to the inflammatory penumbra in experimental multiple sclerosis. Brain 137:92–108. - PubMed
-
- Al‐Izki S, Pryce G, O'Neill JK, Butter C, Giovannoni G, Amor S, Baker D (2012) Practical guide to the induction of relapsing progressive experimental autoimmune encephalomyelitis in the Biozzi ABH mouse. Mult Scler Relat Disord 1:29–38. - PubMed
-
- Baker D, Amor S (2014) Experimental autoimmune encephalomyelitis is a good model of multiple sclerosis if used wisely. Mult Scler Relat Disord 3:555–564. - PubMed
-
- Bakker DA, Ludwin SK (1987) Blood–brain barrier permeability during Cuprizone‐induced demyelination. Implications for the pathogenesis of immune‐mediated demyelinating diseases . J Neurol Sci 78:125–137. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

