China PEACE risk estimation tool for in-hospital death from acute myocardial infarction: an early risk classification tree for decisions about fibrinolytic therapy
- PMID: 27798032
- PMCID: PMC5093680
- DOI: 10.1136/bmjopen-2016-013355
China PEACE risk estimation tool for in-hospital death from acute myocardial infarction: an early risk classification tree for decisions about fibrinolytic therapy
Abstract
Objectives: As the predominant approach to acute reperfusion for ST segment elevation myocardial infarction (STEMI) in many countries, fibrinolytic therapy provides a relative risk reduction for death of ∼16% across the range of baseline risk. For patients with low baseline mortality risk, fibrinolytic therapy may therefore provide little benefit, which may be offset by the risk of major bleeding. We aimed to construct a tool to determine if it is possible to identify a low-risk group among fibrinolytic therapy-eligible patients.
Design: Cross-sectional study.
Setting: The China Patient-centered Evaluative Assessment of Cardiac Events (PEACE) study includes a nationally representative retrospective sample of patients admitted with acute myocardial infarction (AMI) in 162 hospitals.
Participants: 3741 patients with STEMI who were fibrinolytic-eligible but did not receive reperfusion therapy.
Main outcome measures: In-hospital mortality, which was defined as a composite of death occurring within hospitalisation or withdrawal from treatment due to a terminal status at discharge.
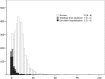
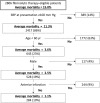
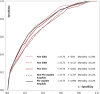
Results: In the study cohort, the in-hospital mortality was 14.7%. In the derivation cohort and the validation cohort, the combination of systolic blood pressure (≥100 mm Hg), age (<60 years old) and gender (male) identified one-fifth of the cohort with an average mortality rate of <3.0%. Half of this low risk group-those with non-anterior AMI-had an average in-hospital death risk of 1.5%.
Conclusions: Nearly, one in five patients with STEMI who are eligible for fibrinolytic therapy are at a low risk for in-hospital death. Three simple factors available at the time of presentation can identify these individuals and support decision-making about the use of fibrinolytic therapy.
Trial registration number: NCT01624883.
Keywords: Fibrinolytic therapy; risk tool.
Published by the BMJ Publishing Group Limited. For permission to use (where not already granted under a licence) please go to http://www.bmj.com/company/products-services/rights-and-licensing/.
Conflict of interest statement
HMK reports research grants from Medtronic and Johnson & Johnson, through Yale University, to develop methods of clinical trial data sharing, and the chair of a cardiac scientific advisory board for UnitedHealth.
Figures

Similar articles
-
High mortality with ST elevation myocardial infarction in a nontrial setting.Can J Cardiol. 2004 Dec;20(14):1455-9. Can J Cardiol. 2004. PMID: 15614341
-
ST-segment elevation myocardial infarction in China from 2001 to 2011 (the China PEACE-Retrospective Acute Myocardial Infarction Study): a retrospective analysis of hospital data.Lancet. 2015 Jan 31;385(9966):441-51. doi: 10.1016/S0140-6736(14)60921-1. Epub 2014 Jun 23. Lancet. 2015. PMID: 24969506 Free PMC article.
-
Development and validation of Women Acute Myocardial Infarction in-Hospital Mortality Score (WAMI Score).Int J Cardiol. 2018 May 15;259:31-39. doi: 10.1016/j.ijcard.2017.12.010. Int J Cardiol. 2018. PMID: 29579607
-
Therapy for ST-segment elevation myocardial infarction patients who present late or are ineligible for reperfusion therapy.J Am Coll Cardiol. 2010 May 4;55(18):1895-906. doi: 10.1016/j.jacc.2009.11.087. J Am Coll Cardiol. 2010. PMID: 20430260 Review.
-
Reperfusion strategies in acute ST-segment elevation myocardial infarction: a comprehensive review of contemporary management options.J Am Coll Cardiol. 2007 Sep 4;50(10):917-29. doi: 10.1016/j.jacc.2007.04.084. Epub 2007 Aug 21. J Am Coll Cardiol. 2007. PMID: 17765117 Review.
Cited by
-
The role of late reperfusion in ST-segment elevation myocardial infarction: a real-world retrospective cohort study.BMC Cardiovasc Disord. 2020 Apr 28;20(1):207. doi: 10.1186/s12872-020-01479-0. BMC Cardiovasc Disord. 2020. PMID: 32345243 Free PMC article.
-
Rationale and design of the Henan ST elevation myocardial infarction (STEMI) registry: a regional STEMI project in predominantly rural central China.BMC Cardiovasc Disord. 2019 Nov 28;19(1):271. doi: 10.1186/s12872-019-1250-9. BMC Cardiovasc Disord. 2019. PMID: 31783791 Free PMC article.
-
Risk stratification model for in-hospital death in patients undergoing percutaneous coronary intervention: a nationwide retrospective cohort study in Japan.BMJ Open. 2019 May 22;9(5):e026683. doi: 10.1136/bmjopen-2018-026683. BMJ Open. 2019. PMID: 31122979 Free PMC article.
-
Neutrophil to platelet ratio predicts in-hospital mortality in patients with acute myocardial infarction.Intern Emerg Med. 2025 Apr;20(3):723-731. doi: 10.1007/s11739-025-03859-w. Epub 2025 Jan 21. Intern Emerg Med. 2025. PMID: 39838258
References
-
- Chen Y, Jiang L, Zhang Q et al. . Doctor-reported hospital management of acute coronary syndrome in China: a nationwide survey of 1029 hospitals in 30 provinces. World J Cardiovasc Dis 2012;2:168–76.
-
- Fibrinolytic Therapy Trialists’ (FTT) Collaborative Group. Indications for fibrinolytic therapy in suspected acute myocardial infarction: collaborative overview of early mortality and major morbidity results from all randomised trials of more than 1000 patients. Lancet 1994;343:311–22. - PubMed
-
- O'Gara PT, Kushner FG, Ascheim DD et al. , American College of Emergency Physicians, Society for Cardiovascular Angiography and Interventions. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 2013;61:e78–e140. 10.1016/j.jacc.2012.11.019 - DOI - PubMed
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
