Impact of local treatment on overall survival of patients with metastatic prostate cancer: systematic review and meta-analysis
- PMID: 27802009
- PMCID: PMC5557433
- DOI: 10.1590/S1677-5538.IBJU.2016.0483
Impact of local treatment on overall survival of patients with metastatic prostate cancer: systematic review and meta-analysis
Abstract
Context: Currently, standard treatment of metastatic prostatic cancer (MPCa) is androgen-deprivation therapy (ADT). Recent studies suggested that local treatment of MPCa is related to increase of survival of those patients, as observed in other tumors.
Objective: To evaluate the impact of local treatment on overall survival and cancer specific survival in 3 and 5 years in patients with MPCa.
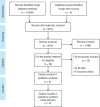
Materials and methods: Systematic review and meta-analysis of population studies published at PubMed, Scielo, Lilacs, Cochrane and EMBASE databases until June 2016. Several large cohorts and Post-Roc studies were included, that evaluated patients with MPCa submitted to local treatment (LT) using radiotherapy (RDT), surgery (RP) or brachytherapy (BCT) or not submitted to local treatment (NLT).
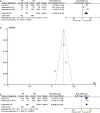
Results: 34.338 patients were analyzed in six included papers, 31.653 submitted to NLT and 2.685 to LT. Overall survival in three years was significantly higher in patients submitted to LT versus NLT (64.2% vs. 44.5%; RD 0.19, 95% CI, 0.17-0.21; p<0.00001; I²=0%), as well as in five years (51.9% vs. 23.6%; RD 0.30, 95% CI, 0.11-0.49; p<0.00001; I²=97%). Sensitive analysis according to type of local treatment showed that surgery (78.2% and 45.0%; RD 0.31, 95% CI, 0.26-0.35; p<0.00001; I²=50%) and radiotherapy (60.4% and 44.5%; RD 0.17, 95% CI, 0.12-0.22; p<0.00001; I²=67%) presented better outcomes.
Conclusion: LT using RDT, RP or BCT seems to significantly improve overall survival and cancer-specific survival of patients with metastatic prostatic cancer. Prospective and randomized studies must be performed in order to confirm our results.
Keywords: Prostate; Prostatic Neoplasms; Radiation Oncology; Survival.
Copyright® by the International Brazilian Journal of Urology.
Conflict of interest statement
CONFLICT OF INTEREST
None declared.
Figures

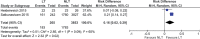



References
-
- Bolla M, van Poppel H, Tombal B, Vekemans K, Da Pozzo L, de Reijke TM, et al. Postoperative radiotherapy after radical prostatectomy for high-risk prostate cancer: long-term results of a randomised controlled trial (EORTC trial 22911) Lancet. 2012;380:2018–2027. - PubMed
-
- Wiegel T, Bartkowiak D, Bottke D, Bronner C, Steiner U, Siegmann A, et al. Adjuvant radiotherapy versus wait-and-see after radical prostatectomy: 10-year follow-up of the ARO 96-02/AUO AP 09/95 trial. Eur Urol. 2014;66:243–250. - PubMed
-
- Swanson G, Thompson I, Basler J, Crawford ED. Metastatic prostate cancer-does treatment of the primary tumor matter? J Urol. 2006;176:1292–1298. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous
