Automatic Estimation of Volumetric Breast Density Using Artificial Neural Network-Based Calibration of Full-Field Digital Mammography: Feasibility on Japanese Women With and Without Breast Cancer
- PMID: 27832519
- PMCID: PMC5359207
- DOI: 10.1007/s10278-016-9922-9
Automatic Estimation of Volumetric Breast Density Using Artificial Neural Network-Based Calibration of Full-Field Digital Mammography: Feasibility on Japanese Women With and Without Breast Cancer
Abstract
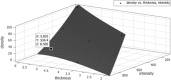
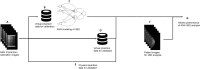
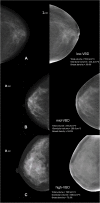
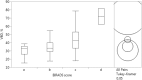
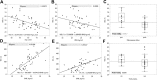
Breast cancer is the most common invasive cancer among women and its incidence is increasing. Risk assessment is valuable and recent methods are incorporating novel biomarkers such as mammographic density. Artificial neural networks (ANN) are adaptive algorithms capable of performing pattern-to-pattern learning and are well suited for medical applications. They are potentially useful for calibrating full-field digital mammography (FFDM) for quantitative analysis. This study uses ANN modeling to estimate volumetric breast density (VBD) from FFDM on Japanese women with and without breast cancer. ANN calibration of VBD was performed using phantom data for one FFDM system. Mammograms of 46 Japanese women diagnosed with invasive carcinoma and 53 with negative findings were analyzed using ANN models learned. ANN-estimated VBD was validated against phantom data, compared intra-patient, with qualitative composition scoring, with MRI VBD, and inter-patient with classical risk factors of breast cancer as well as cancer status. Phantom validations reached an R 2 of 0.993. Intra-patient validations ranged from R 2 of 0.789 with VBD to 0.908 with breast volume. ANN VBD agreed well with BI-RADS scoring and MRI VBD with R 2 ranging from 0.665 with VBD to 0.852 with breast volume. VBD was significantly higher in women with cancer. Associations with age, BMI, menopause, and cancer status previously reported were also confirmed. ANN modeling appears to produce reasonable measures of mammographic density validated with phantoms, with existing measures of breast density, and with classical biomarkers of breast cancer. FFDM VBD is significantly higher in Japanese women with cancer.
Keywords: Artificial neural networks (ANN); Breast tissue density; Computer analysis; Full-field digital mammography (FFDM); Image processing; Imaging phantoms; Machine learning; Magnetic resonance imaging.
Conflict of interest statement
The authors declare that there is no conflict of interest that has an interest in the subject matter or materials discussed in the manuscript.
Figures





Similar articles
-
Fully Automated Quantitative Estimation of Volumetric Breast Density from Digital Breast Tomosynthesis Images: Preliminary Results and Comparison with Digital Mammography and MR Imaging.Radiology. 2016 Apr;279(1):65-74. doi: 10.1148/radiol.2015150277. Epub 2015 Oct 21. Radiology. 2016. PMID: 26491909 Free PMC article.
-
Breast density quantification in dual-energy mammography using virtual anthropomorphic phantoms.J Appl Clin Med Phys. 2024 May;25(5):e14360. doi: 10.1002/acm2.14360. Epub 2024 Apr 22. J Appl Clin Med Phys. 2024. PMID: 38648734 Free PMC article.
-
Comparison of synthetic mammography, reconstructed from digital breast tomosynthesis, and digital mammography: evaluation of lesion conspicuity and BI-RADS assessment categories.Breast Cancer Res Treat. 2017 Dec;166(3):765-773. doi: 10.1007/s10549-017-4458-3. Epub 2017 Aug 17. Breast Cancer Res Treat. 2017. PMID: 28819781
-
Reproductive Factors and Mammographic Density: Associations Among 24,840 Women and Comparison of Studies Using Digitized Film-Screen Mammography and Full-Field Digital Mammography.Am J Epidemiol. 2019 Jun 1;188(6):1144-1154. doi: 10.1093/aje/kwz033. Am J Epidemiol. 2019. PMID: 30865217 Free PMC article. Review.
-
Vision 20/20: Mammographic breast density and its clinical applications.Med Phys. 2015 Dec;42(12):7059-77. doi: 10.1118/1.4935141. Med Phys. 2015. PMID: 26632060 Review.
Cited by
-
Impact of full field digital mammography diagnosis for female patients with breast cancer.Medicine (Baltimore). 2019 Apr;98(16):e15175. doi: 10.1097/MD.0000000000015175. Medicine (Baltimore). 2019. PMID: 31008938 Free PMC article.
-
Blood Test for Breast Cancer Screening through the Detection of Tumor-Associated Circulating Transcripts.Int J Mol Sci. 2022 Aug 15;23(16):9140. doi: 10.3390/ijms23169140. Int J Mol Sci. 2022. PMID: 36012405 Free PMC article.
-
Detection of Lung Contour with Closed Principal Curve and Machine Learning.J Digit Imaging. 2018 Aug;31(4):520-533. doi: 10.1007/s10278-018-0058-y. J Digit Imaging. 2018. PMID: 29450843 Free PMC article. Review.
-
An Automatic Parameter Decision System of Bilateral Filtering with GPU-Based Acceleration for Brain MR Images.J Digit Imaging. 2019 Feb;32(1):148-161. doi: 10.1007/s10278-018-0110-y. J Digit Imaging. 2019. PMID: 30088157 Free PMC article.
References
-
- Peter B, Bernard L: World cancer report. 2008
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

