Invasive mucormycosis in children: an epidemiologic study in European and non-European countries based on two registries
- PMID: 27832748
- PMCID: PMC5105268
- DOI: 10.1186/s12879-016-2005-1
Invasive mucormycosis in children: an epidemiologic study in European and non-European countries based on two registries
Abstract
Background: Mucormycosis has emerged as a rare but frequently fatal invasive fungal disease. Current knowledge on paediatric mucormycosis is based on case reports and small series reported over several decades. Contemporary data on a large cohort of patients is lacking.
Methods: Two large international registries (Zygomyco.net and FungiScope™) were searched for mucormycosis cases in ≤19 year-old patients. Cases enrolled between 2005 and 2014 were extracted, and dual entries in the two databases merged. Epidemiology, clinical characteristics, diagnostic procedures, therapeutic management and final outcome were recorded and analysed with SPSS v.12.
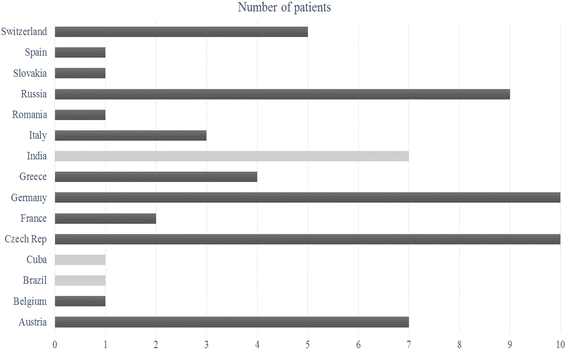
Results: Sixty-three unique cases (44 proven and 19 probable) were enrolled from 15 countries (54 in European and 9 in non-European countries). Median age was 13 years [Interquartile Range (IQR) 7.7] with a slight predominance (54.1 %) of females. Underlying conditions were haematological malignancies (46 %), other malignancies (6.3 %), haematopoietic stem cell transplantation (15.9 %), solid organ transplantation, trauma/surgery and diabetes mellitus (4.8 % each) and a variety of other diseases (7.9 %); in 9.5%, no underlying medical condition was found. Neutropenia was recorded in 46 % of the patients. The main sites of infection were lungs (19 %), skin and soft tissues (19 %), paranasal sinus/sino-orbital region (15.8 %) and rhino-cerebral region (7.9 %). Disseminated infection was present in 38.1 %. Mucormycosis diagnosis was based on several combinations of methods; culture combined with histology was performed in 31 cases (49.2 %). Fungal isolates included Rhizopus spp. (39.7 %), Lichtheimia spp. (17.5 %), Mucor spp. (12.7 %), Cunninghamella bertholletiae (6.3 %) and unspecified (23.8 %). Treatment comprised amphotericin B (AmB) monotherapy in 31.7 % or AmB in combination with other antifungals in 47.7 % of the cases, while 14.3 % received no antifungals. Surgery alone was performed in 6.3 %, and combined with antifungal therapy in 47.6 %. Crude mortality at last contact of follow-up was 33.3 %. In regression analysis, disseminated disease and prior haematopoietic stem cell transplantation were associated with increased odds of death, whereas the combination of systemic antifungal therapy with surgery was associated with improved survival.
Conclusion: Paediatric mucormycosis mainly affects children with malignancies, presents as pulmonary, soft tissue, paranasal sinus or disseminated disease and is highly lethal. Outcome is improved when active antifungal therapy and surgery are combined.
Keywords: FungiScope™; Mucormycosis; Paediatric invasive fungal diseases; Zygomyco.net; Zygomycosis.
Figures
References
-
- Neofytos D, Horn D, Anaissie E, Steinbach W, Olyaei A, Fishman J, Pfaller M, Chang C, Webster K, Marr K. Epidemiology and outcome of invasive fungal infection in adult hematopoietic stem cell transplant recipients: analysis of Multicenter Prospective Antifungal Therapy (PATH) Alliance registry. Clin Infect Dis. 2009;48(3):265–273. doi: 10.1086/595846. - DOI - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous