Brain adaptation to hypoxia and hyperoxia in mice
- PMID: 27835780
- PMCID: PMC5107733
- DOI: 10.1016/j.redox.2016.10.018
Brain adaptation to hypoxia and hyperoxia in mice
Abstract
Aims: Hyperoxic breathing might lead to redox imbalance and signaling changes that affect cerebral function. Paradoxically, hypoxic breathing is also believed to cause oxidative stress. Our aim is to dissect the cerebral tissue responses to altered O2 fractions in breathed air by assessing the redox imbalance and the recruitment of the hypoxia signaling pathways.
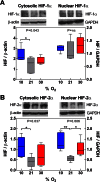
Results: Mice were exposed to mild hypoxia (10%O2), normoxia (21%O2) or mild hyperoxia (30%O2) for 28 days, sacrificed and brain tissue excised and analyzed. Although one might expect linear responses to %O2, only few of the examined variables exhibited this pattern, including neuroprotective phospho- protein kinase B and the erythropoietin receptor. The major reactive oxygen species (ROS) source in brain, NADPH oxidase subunit 4 increased in hypoxia but not in hyperoxia, whereas neither affected nuclear factor (erythroid-derived 2)-like 2, a transcription factor that regulates the expression of antioxidant proteins. As a result of the delicate equilibrium between ROS generation and antioxidant defense, neuron apoptosis and cerebral tissue hydroperoxides increased in both 10%O2 and 30%O2, as compared with 21%O2. Remarkably, the expression level of hypoxia-inducible factor (HIF)-2α (but not HIF-1α) was higher in both 10%O2 and 30%O2 with respect to 21%O2 INNOVATION: Comparing the in vivo effects driven by mild hypoxia with those driven by mild hyperoxia helps addressing whether clinically relevant situations of O2 excess and scarcity are toxic for the organism.
Conclusion: Prolonged mild hyperoxia leads to persistent cerebral damage, comparable to that inferred by prolonged mild hypoxia. The underlying mechanism appears related to a model whereby the imbalance between ROS generation and anti-ROS defense is similar, but occurs at higher levels in hypoxia than in hyperoxia.
Keywords: Hypoxia-inducible factor; In vivo hyperoxia; In vivo hypoxia; Neurons; Oxidative injury.
Copyright © 2016 The Authors. Published by Elsevier B.V. All rights reserved.
Figures





References
-
- Allen B.W., Demchenko I.T., Piantadosi C.A. Two faces of nitric oxide: implications for cellular mechanisms of oxygen toxicity. J. Appl. Physiol. 1985;106(662–7):2009. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

