Risk Factors for Incident Carotid Artery Revascularization among Older Adults: The Cardiovascular Health Study
- PMID: 27846618
- PMCID: PMC5836156
- DOI: 10.1159/000452426
Risk Factors for Incident Carotid Artery Revascularization among Older Adults: The Cardiovascular Health Study
Abstract
Background: Population-based risk factors for carotid artery revascularization are not known. We investigated the association between demographic and clinical characteristics and incident carotid artery revascularization in a cohort of older adults.
Methods: Among Cardiovascular Health Study participants, a population-based cohort of 5,888 adults aged 65 years or older enrolled in two waves (1989-1990 and 1992-1993), 5,107 participants without a prior history of carotid endarterectomy (CEA) or cerebrovascular disease had a carotid ultrasound at baseline and were included in these analyses. Cox proportional hazards multivariable analysis was used to determine independent risk factors for incident carotid artery revascularization.
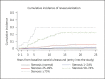
Results: Over a mean follow-up of 13.5 years, 141 participants underwent carotid artery revascularization, 97% were CEA. Baseline degree of stenosis and incident ischemic cerebral events occurring during follow-up were the strongest predictors of incident revascularization. After adjustment for these, factors independently associated with an increased risk of incident revascularization were: hypertension (HR 1.53; 95% CI: 1.05-2.23), peripheral arterial disease (HR 2.57; 95% CI: 1.34-4.93), and low-density lipoprotein cholesterol (HR 1.23 per standard deviation [SD] increment [35.4 mg/dL]; 95% CI: 1.04-1.46). Factors independently associated with a lower risk of incident revascularization were: female gender (HR 0.51; 95% CI: 0.34-0.77) and older age (HR 0.69 per SD increment [5.5 years]; 95% CI: 0.56-0.86).
Conclusions: Even after accounting for carotid stenosis and incident cerebral ischemic events, carotid revascularization is related to age, gender, and cardiovascular risk factors. Further study of these demographic disparities and the role of risk factor control is warranted.
Keywords: Cardiovascular risk factors; Carotid artery disease; Carotid duplex; Carotid endarterectomy; Gender.
© 2016 The Author(s) Published by S. Karger AG, Basel.
Figures
Similar articles
-
The natural history of asymptomatic severe carotid artery stenosis.J Vasc Surg. 2014 Nov;60(5):1218-1226. doi: 10.1016/j.jvs.2014.05.047. Epub 2014 Jul 17. J Vasc Surg. 2014. PMID: 25041986
-
Coronary revascularization of patients with silent coronary ischemia may reduce the risk of myocardial infarction and cardiovascular death after carotid endarterectomy.J Vasc Surg. 2022 Sep;76(3):750-759. doi: 10.1016/j.jvs.2022.05.004. Epub 2022 Jun 3. J Vasc Surg. 2022. PMID: 35667605
-
Transcarotid artery revascularization versus carotid endarterectomy and transfemoral stenting in octogenarians.J Vasc Surg. 2021 Nov;74(5):1602-1608. doi: 10.1016/j.jvs.2021.05.028. Epub 2021 May 31. J Vasc Surg. 2021. PMID: 34082003
-
Risk Factors for Restenosis After Carotid Revascularization: A Meta-Analysis of Hazard Ratios.World Neurosurg. 2019 May;125:414-424. doi: 10.1016/j.wneu.2019.02.065. Epub 2019 Feb 27. World Neurosurg. 2019. PMID: 30822589
-
The diagnosis and treatment of asymptomatic and symptomatic patients with carotid artery stenosis.Curr Probl Cardiol. 2025 Jun;50(6):102992. doi: 10.1016/j.cpcardiol.2025.102992. Epub 2025 Jan 18. Curr Probl Cardiol. 2025. PMID: 39832540 Review.
Cited by
-
Serum Non-Esterified Fatty Acids, Carotid Artery Intima-Media Thickness and Flow-Mediated Dilation in Older Adults: The Cardiovascular Health Study (CHS).Nutrients. 2021 Aug 31;13(9):3052. doi: 10.3390/nu13093052. Nutrients. 2021. PMID: 34578930 Free PMC article.
-
Acute strength training promotes responses in whole blood circulating levels of miR-146a among older adults with type 2 diabetes mellitus.Clin Interv Aging. 2017 Sep 15;12:1443-1450. doi: 10.2147/CIA.S141716. eCollection 2017. Clin Interv Aging. 2017. PMID: 28979106 Free PMC article.
-
Diagnosis of extracranial carotid stenosis by MRA of the brain.Sci Rep. 2021 Jun 8;11(1):12010. doi: 10.1038/s41598-021-91511-w. Sci Rep. 2021. PMID: 34103593 Free PMC article. Clinical Trial.
References
-
- Lewis RF, Abrahamowicz M, Cote R, Batista RN. Predictive power of duplex ultrasonography in asymptomatic carotid disease. Ann Intern Med. 1997;127:13–20. - PubMed
-
- Mansour MA, Mattos MA, Faught WE, Hodgson KJ, Barkmeier LD, Ramsey DE, Sumner DS. The natural history of moderate (50–79%) internal carotid artery stenosis in symptomatic, nonhemispheric, and asymptomatic patients. J Vasc Surg. 1995;21:346–356. - PubMed
-
- Barnett HJ, Taylor DW, Eliasziw M, Fox AJ, Ferguson GG, Haynes RB, Rankin RN, Glagett GP, Hachinski VC, Sackett DL, Thorpe KE, Meldrum HE, Spence JD. Benefit of carotid endarterectomy in patients with symptomatic moderate or severe stenosis. N Engl J Med. 1998;339:1415–1425. - PubMed
-
- Executive Committee for the Asymptomatic Carotid Atherosclerosis Study Endarterectomy for asymptomatic carotid artery stenosis. JAMA. 1995;273:1421–1428. - PubMed
-
- North American Symptomatic Carotid Endarterectomy Trial Collaborators Beneficial effect of carotid endarterectomy in symptomatic patients with high-grade carotid stenosis. N Engl J Med. 1991;325:445–453. - PubMed
Grants and funding
- N01 HC085080/HL/NHLBI NIH HHS/United States
- U01 HL080295/HL/NHLBI NIH HHS/United States
- N01 HC085082/HL/NHLBI NIH HHS/United States
- N01 HC085085/HC/NHLBI NIH HHS/United States
- HHSN268201200036C/HL/NHLBI NIH HHS/United States
- N01 HC055222/HL/NHLBI NIH HHS/United States
- N01 HC085079/HL/NHLBI NIH HHS/United States
- N01 HC085084/HC/NHLBI NIH HHS/United States
- R01 AG023629/AG/NIA NIH HHS/United States
- N01 HC045133/HC/NHLBI NIH HHS/United States
- N01 HC035129/HC/NHLBI NIH HHS/United States
- N01 HC085081/HL/NHLBI NIH HHS/United States
- HHSN268200800007C/HL/NHLBI NIH HHS/United States
- N01 HC085086/HL/NHLBI NIH HHS/United States
- N01 HC085083/HL/NHLBI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources