Effect of Intensive Versus Standard Clinic-Based Hypertension Management on Ambulatory Blood Pressure: Results From the SPRINT (Systolic Blood Pressure Intervention Trial) Ambulatory Blood Pressure Study
- PMID: 27849563
- PMCID: PMC5145774
- DOI: 10.1161/HYPERTENSIONAHA.116.08076
Effect of Intensive Versus Standard Clinic-Based Hypertension Management on Ambulatory Blood Pressure: Results From the SPRINT (Systolic Blood Pressure Intervention Trial) Ambulatory Blood Pressure Study
Abstract
The effect of clinic-based intensive hypertension treatment on ambulatory blood pressure (BP) is unknown. The goal of the SPRINT (Systolic Blood Pressure Intervention Trial) ambulatory BP ancillary study was to evaluate the effect of intensive versus standard clinic-based BP targets on ambulatory BP. Ambulatory BP was obtained within 3 weeks of the 27-month study visit in 897 SPRINT participants. Intensive treatment resulted in lower clinic systolic BP (mean difference between groups=16.0 mm Hg; 95% confidence interval, 14.1-17.8 mm Hg), nighttime systolic BP (mean difference=9.6 mm Hg; 95% confidence interval, 7.7-11.5 mm Hg), daytime systolic BP (mean difference=12.3 mm Hg; 95% confidence interval, 10.6-13.9 mm Hg), and 24-hour systolic BP (mean difference=11.2 mm Hg; 95% confidence interval, 9.7-12.8 mm Hg). The night/day systolic BP ratio was similar between the intensive (0.92±0.09) and standard-treatment groups (0.91±0.09). There was considerable lack of agreement within participants between clinic systolic BP and daytime ambulatory systolic BP with wide limits of agreement on Bland-Altman plots. In conclusion, targeting a systolic BP of <120 mm Hg, when compared with <140 mm Hg, resulted in lower nighttime, daytime, and 24-hour systolic BP, but did not change the night/day systolic BP ratio. Ambulatory BP monitoring may be required to assess the effect of targeted hypertension therapy on out of office BP. Further studies are needed to assess whether targeting hypertension therapy based on ambulatory BP improves clinical outcomes.
Clinical trial registration: URL: http://www.clinicaltrials.gov. Unique identifier: NCT01835249.
Keywords: blood pressure; circadian rhythm; goals; hypertension; stroke.
© 2016 American Heart Association, Inc.
Conflict of interest statement
The remaining authors report no conflicts of interest.
Figures
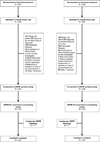


Comment in
-
SPRINT Blood Pressure: Sprinting Back to Smirk's Basal Blood Pressure?Hypertension. 2017 Jan;69(1):15-19. doi: 10.1161/HYPERTENSIONAHA.116.08216. Epub 2016 Nov 14. Hypertension. 2017. PMID: 27849568 No abstract available.
References
-
- Verdecchia P, Porcellati C, Schillaci G, Borgioni C, Ciucci A, Battistelli M, Guerrieri M, Gatteschi C, Zampi I, Santucci A, Santucci C, Reboldi G. Ambulatory blood pressure. An independent predictor of prognosis in essential hypertension. Hypertension. 1994;24:793–801. - PubMed
-
- Sega R, Facchetti R, Bombelli M, Cesana G, Corrao G, Grassi G, Mancia G. Prognostic value of ambulatory and home blood pressures compared with office blood pressure in the general population: follow-up results from the Pressioni Arteriose Monitorate e Loro Associazioni (PAMELA) study. Circulation. 2005;111:1777–1783. - PubMed
-
- Staessen JA, Thijs L, Fagard R, O'Brien ET, Clement D, de Leeuw PW, Mancia G, Nachev C, Palatini P, Parati G, Tuomilehto J, Webster J. Predicting cardiovascular risk using conventional vs ambulatory blood pressure in older patients with systolic hypertension. Systolic Hypertension in Europe Trial Investigators. JAMA. 1999;282:539–546. - PubMed
-
- Dolan E, Stanton A, Thijs L, Hinedi K, Atkins N, McClory S, Den Hond E, McCormack P, Staessen JA, O'Brien E. Superiority of ambulatory over clinic blood pressure measurement in predicting mortality: the Dublin outcome study. Hypertension. 2005;46:156–161. - PubMed
-
- Minutolo R, Gabbai FB, Agarwal R, Chiodini P, Borrelli S, Bellizzi V, Nappi F, Stanzione G, Conte G, De Nicola L. Assessment of achieved clinic and ambulatory blood pressure recordings and outcomes during treatment in hypertensive patients with CKD: A multicenter prospective cohort study. Am J Kidney Dis. 2014;64:744–752. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
- UL1 TR000433/TR/NCATS NIH HHS/United States
- UL1 TR000445/TR/NCATS NIH HHS/United States
- UL1 TR000064/TR/NCATS NIH HHS/United States
- UL1 TR000075/TR/NCATS NIH HHS/United States
- U54 GM104940/GM/NIGMS NIH HHS/United States
- UL1 TR000050/TR/NCATS NIH HHS/United States
- R01 HL130500/HL/NHLBI NIH HHS/United States
- K23 DK091521/DK/NIDDK NIH HHS/United States
- UL1 RR024134/RR/NCRR NIH HHS/United States
- HHSN268200900048C/HL/NHLBI NIH HHS/United States
- UL1 TR000005/TR/NCATS NIH HHS/United States
- HHSN268200900040C/HL/NHLBI NIH HHS/United States
- HHSN268200900046C/HL/NHLBI NIH HHS/United States
- P30 GM103337/GM/NIGMS NIH HHS/United States
- UL1 TR001064/TR/NCATS NIH HHS/United States
- UL1 RR025752/RR/NCRR NIH HHS/United States
- UL1 RR025771/RR/NCRR NIH HHS/United States
- R03 DK105314/DK/NIDDK NIH HHS/United States
- K12 HD043451/HD/NICHD NIH HHS/United States
- UL1 TR000114/TR/NCATS NIH HHS/United States
- UL1 TR000093/TR/NCATS NIH HHS/United States
- HHSN268200900049C/HL/NHLBI NIH HHS/United States
- HHSN268200900047C/HL/NHLBI NIH HHS/United States
- UL1 TR001427/TR/NCATS NIH HHS/United States
- UL1 TR000003/TR/NCATS NIH HHS/United States
- UL1 TR000439/TR/NCATS NIH HHS/United States
- UL1 TR000073/TR/NCATS NIH HHS/United States
- R03 DK100530/DK/NIDDK NIH HHS/United States
- UL1 RR025755/RR/NCRR NIH HHS/United States
- UL1 TR002003/TR/NCATS NIH HHS/United States
- UL1 TR000002/TR/NCATS NIH HHS/United States
- UL1 TR000105/TR/NCATS NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

