Trends and Outcomes of Pulmonary Arterial Hypertension-Related Hospitalizations in the United States: Analysis of the Nationwide Inpatient Sample Database From 2001 Through 2012
- PMID: 27851838
- PMCID: PMC12167389
- DOI: 10.1001/jamacardio.2016.3591
Trends and Outcomes of Pulmonary Arterial Hypertension-Related Hospitalizations in the United States: Analysis of the Nationwide Inpatient Sample Database From 2001 Through 2012
Abstract
Importance: Recent trends and outcomes of pulmonary arterial hypertension (PAH)-related hospitalization in adults in the United States are unknown.
Objective: To examine the characteristics of PAH-related hospitalizations.
Design, setting, and participants: We analyzed the National Inpatient Sample database for all adult patients (≥18 years old) with PAH as the principal discharge diagnosis from January 1, 2001, through December 31, 2012.
Main outcomes and measures: We analyzed the temporal trends in hospitalization rate, hospital charges, in-hospital mortality, length of hospitalization, and comorbidities pertaining to PAH-related hospitalizations. We also evaluated the predictors of in-hospital mortality and length of hospitalizations.
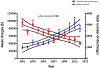
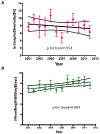
Results: The number of PAH-related hospitalizations per year in adults decreased significantly from 2001 through 2012 (3177 vs 1345, P for trend <.001). However, the mean hospital charge per admission increased 2.7-fold from 2001 through 2012 ($29 507 vs $79 607, P for trend <.001). There was a significant increase in each of these associated comorbid conditions: diabetes (4.6%-7.8%), hypertension (5.1%-17.1%), coronary artery disease (15.6%-22.3%), chronic obstructive pulmonary disease (14.4%-20.1%), anemia (12.4%-20.4%), cardiac dysrhythmias (21.7%-29.0%), congestive heart failure (40.7%-56.1%), acute (5.9%-20.1%) or chronic kidney disease (1.1%-16.4%), fluid and electrolyte imbalance (18.9%-35.3%), pneumonia (4.4%-6.3%), cardiogenic shock (0.5%-1.5%), and acute respiratory failure (4.3%-20.8%) from 2001 through 2012. The length of hospitalization increased (mean [SE], 7.0 [0.5] days in 2001 vs 7.6 [0.6] days in 2012, P for trend = .009), but in-patient mortality remained unchanged (7.8% [1.1%] in 2001 vs 6.3% [1.7%] in 2012, P for trend = .54). Admission to a teaching hospital (β coefficient for length of hospitalization, 2.0; 95% CI, 1.3-1.6; odds ratio [OR] for mortality, 1.5; 95% CI, 1.1-2.1), cardiac dysrhythmias (β coefficient, 1.8; 95% CI, 1.1-2.6; OR, 1.8; 95% CI, 1.4-2.4), acute kidney injury (β coefficient, 5.0; 95% CI, 3.9-6.1; OR, 2.3; 95% CI, 1.7-3.2), acute cerebrovascular accident (β coefficient, 6.6; 95% CI, 1.9-11.3; OR, 6.7; 95% CI, 2.1-21.1), and acute respiratory failure (β coefficient, 6.2; 95% CI, 5.1-7.4; OR, 5.6; 95% CI, 4.2-7.5) were associated with increased length of hospitalization and in-hospital mortality. Congestive heart failure (OR, 1.7; 95% CI, 1.3-2.2), cardiogenic shock (OR, 5.4; 95% CI, 2.7-10.9), and fluid and electrolyte imbalance (OR, 1.9; 95% CI, 1.5-2.4) were associated with increased in-hospital mortality but not length of hospitalization.
Conclusions and relevance: Analyses of temporal changes in PAH care reveal a significant decrease in PAH-related hospitalizations in the United States, but hospital charges have increased substantially and are increasingly being borne by Medicare. In-hospital mortality remains unchanged, but length of hospitalization has increased. This study should help identify the characteristics of patients with PAH that are associated with increased risk of in-hospital mortality and longer length of hospitalization.
Conflict of interest statement
Figures
References
-
- Galiè N, Torbicki A, Barst R et al. Guidelines on diagnosis and treatment of pulmonary arterial hypertension. The Task Force on Diagnosis and Treatment of Pulmonary Arterial Hypertension of the European Society of Cardiology. Eur Heart J. 2004;25:2243–78. - PubMed
-
- Galiè N, Humbert M, Vachiery JL et al. 2015 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension: The Joint Task Force for the Diagnosis and Treatment of Pulmonary Hypertension of the European Society of Cardiology (ESC) and the European Respiratory Society (ERS): Endorsed by: Association for European Paediatric and Congenital Cardiology (AEPC), International Society for Heart and Lung Transplantation (ISHLT). Eur Heart J. 2016;37:67–119. - PubMed
-
- Peacock AJ, Murphy NF, McMurray JJ, Caballero L, Stewart S. An epidemiological study of pulmonary arterial hypertension. Eur Respir J. 2007;30:104–9. - PubMed
-
- Frost AE, Badesch DB, Barst RJ et al. The changing picture of patients with pulmonary arterial hypertension in the United States: how REVEAL differs from historic and non-US Contemporary Registries. Chest. 2011;139:128–37. - PubMed
-
- Humbert M, Sitbon O, Chaouat A et al. Pulmonary arterial hypertension in France: results from a national registry. Am J Respir Crit Care Med. 2006;173:1023–30. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

