High Flow Nasal Cannulae versus Nasal Continuous Positive Airway Pressure in Neonates with Respiratory Distress Syndrome Managed with INSURE Method: A Randomized Clinical Trial
- PMID: 27853329
- PMCID: PMC5106564
High Flow Nasal Cannulae versus Nasal Continuous Positive Airway Pressure in Neonates with Respiratory Distress Syndrome Managed with INSURE Method: A Randomized Clinical Trial
Abstract
Background: In recent years, various noninvasive respiratory support (NRS) of ventilation has been provided more in neonates. The aim of this study was to compare the effect of HFNC with NCPAP in post-extubation of preterm infants with RDS after INSURE method (intubation, surfactant, extubation).
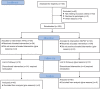
Methods: A total of 54 preterm infants with RDS (respiratory distress syndrome) were enrolled in this study. Using a randomized sequence, they were assigned into two groups after INSURE method. The first group received HFNC while the second group received NCPAP for respiratory support after extubation. A comparison was made between these two groups by the rate of reintubation, air leak syndrome, duration of oxygen therapy, hospitalization, the rate of bronchopulmonary dysplasia (BPD), intraventricular hemorrhage (IVH), retinopathy of prematurity (ROP), and mortality. Data were analyzed by using the SPSS version 18 software. The statistical analyses included Student's t-test for continuous data and compared proportions using Chi-squared test and Fisher's exact test for categorical data.
Result: The rate of reintubation was higher in the HFNC compared with the NCPAP group. The rate of either IVH or ROP had no significant differences between the two groups. In addition, duration of oxygen requirement and hospitalization were not statistically different. There was no case of BPD or mortality among these patients.
Conclusion: This study showed that preterm infants with RDS could manage post-extubation after INSURE method with either NCPAP or HFNC. However, in this single-center study, the rate of reintubation was higher in the HFNC group while further multicenter study might be assigned. Trial Registration Number: IRCT201201228800N1.
Keywords: Oxygen inhalation therapy infant-newborn; Premature birth; Pulmonary surfactants.
Figures
Similar articles
-
[Efficacy of high-flow nasal cannula versus nasal continuous positive airway pressure in the treatment of respiratory distress syndrome in neonates: a Meta analysis].Zhongguo Dang Dai Er Ke Za Zhi. 2020 Nov;22(11):1164-1171. doi: 10.7499/j.issn.1008-8830.2005102. Zhongguo Dang Dai Er Ke Za Zhi. 2020. PMID: 33172549 Free PMC article. Chinese.
-
Comparison of INSURE method with conventional mechanical ventilation after surfactant administration in preterm infants with respiratory distress syndrome: therapeutic challenge.Acta Med Iran. 2014;52(8):596-600. Acta Med Iran. 2014. PMID: 25149882 Clinical Trial.
-
Bi-level Nasal Positive Airway Pressure (BiPAP) versus Nasal Continuous Positive Airway Pressure (CPAP) for Preterm Infants with Birth Weight Less Than 1500 g and Respiratory Distress Syndrome Following INSURE Treatment: A Two-center Randomized Controlled Trial.Curr Med Sci. 2021 Jun;41(3):542-547. doi: 10.1007/s11596-021-2372-8. Epub 2021 Jun 15. Curr Med Sci. 2021. PMID: 34129204 Free PMC article. Clinical Trial.
-
Nasal respiratory support through the nares: its time has come.J Perinatol. 2010 Oct;30 Suppl:S67-72. doi: 10.1038/jp.2010.99. J Perinatol. 2010. PMID: 20877411 Review.
-
High-flow nasal cannulae for respiratory support of preterm infants: a review of the evidence.Neonatology. 2012;102(4):300-8. doi: 10.1159/000341754. Epub 2012 Sep 6. Neonatology. 2012. PMID: 22964658 Review.
Cited by
-
[Efficacy of high-flow nasal cannula versus nasal continuous positive airway pressure in the treatment of respiratory distress syndrome in neonates: a Meta analysis].Zhongguo Dang Dai Er Ke Za Zhi. 2020 Nov;22(11):1164-1171. doi: 10.7499/j.issn.1008-8830.2005102. Zhongguo Dang Dai Er Ke Za Zhi. 2020. PMID: 33172549 Free PMC article. Chinese.
-
Current insights in non-invasive ventilation for the treatment of neonatal respiratory disease.Ital J Pediatr. 2019 Aug 19;45(1):105. doi: 10.1186/s13052-019-0707-x. Ital J Pediatr. 2019. PMID: 31426828 Free PMC article. Review.
-
Nasal high flow therapy for primary respiratory support in preterm infants.Cochrane Database Syst Rev. 2023 May 5;5(5):CD006405. doi: 10.1002/14651858.CD006405.pub4. Cochrane Database Syst Rev. 2023. PMID: 37144837 Free PMC article. Review.
-
The Impact of High-Flow Nasal Cannula Therapy on Acute Respiratory Distress Syndrome Patients: A Systematic Review.Cureus. 2023 Jun 30;15(6):e41219. doi: 10.7759/cureus.41219. eCollection 2023 Jun. Cureus. 2023. PMID: 37397646 Free PMC article. Review.
-
Noninvasive Positive Airway Pressure Management for Post-extubation Support in Preterm Infants: Observational Cohort Study with Overlap Weighting Analysis.Ann Clin Epidemiol. 2023 Nov 10;6(1):17-23. doi: 10.37737/ace.24004. eCollection 2024. Ann Clin Epidemiol. 2023. PMID: 38605917 Free PMC article.
References
-
- LeVan JM, Brion LP, Wrage LA, Gantz MG, Wyckoff MH, Sanchez PJ, et al. Change in practice after the Surfactant, Positive Pressure and Oxygenation Randomised Trial. Arch Dis Child Fetal Neonatal Ed. 2014;99:F386–90. doi: 10.1136/archdischild-2014-306057. [ PMC Free Article] - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Medical