Colonic Transit and Bile Acid Synthesis or Excretion in Patients With Irritable Bowel Syndrome-Diarrhea Without Bile Acid Malabsorption
- PMID: 27856362
- PMCID: PMC5401790
- DOI: 10.1016/j.cgh.2016.11.012
Colonic Transit and Bile Acid Synthesis or Excretion in Patients With Irritable Bowel Syndrome-Diarrhea Without Bile Acid Malabsorption
Abstract
Background and aims: Bile acids (BAs) are passively absorbed to a different extent along the mammalian colon, so that levels are lower in the feces than in proximal colon. Our aim was to explore associations among total, primary, and secretory BA in stool and colonic transit in patients with irritable bowel syndrome-diarrhea (IBS-D) without overt BA malabsorption (BAM).
Methods: In a cross-sectional observational study of 116 patients with IBS-D recruited from local communities in Minnesota, we measured total and individual main fecal BA excretion, fecal fat and fecal weight over 48 hours, fasting serum levels of C4 (surrogate for BA synthesis), and overall colonic transit by scintigraphy (geometric center at 24 hours and 48 hours). Patients without overt BAM were assigned to groups based on total fecal BA level below 2337 μmol/48 hours (n = 86) or serum levels of C4 below 47.1 ng/mL (n = 91). We used Spearman correlations to test study hypotheses with correction for 14 correlations tested (P < .0036). Data from 30 healthy volunteers were used as control subjects.
Results: Patients with IBS-D who had increased or normal total BA excretion in stool or BA synthesis had higher stool proportions of primary BAs (especially chenodeoxycholate), compared with healthy control subjects. In patients with IBS-D without overt BAM (normal 48-hour total fecal BA or serum C4), there were significant positive correlations between total fecal BA, fecal primary and secretory BA, fecal weight, and increased geometric center at 24 and 48 hours (P < .0036). Normal and slightly increased levels of total fecal BA have greatest effects on colonic transit at 48 hours.
Conclusions: In the absence of overt BAM, the total, primary, and secretory BAs in stool contribute to the acceleration of colonic transit and fecal weight in the diarrhea of patients with IBS-D.
Keywords: CDCA; Clinical Study; Intestine; Lithocholate.
Copyright © 2017 AGA Institute. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Figures
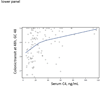

References
-
- Ridlon JM, Kang DJ, Hylemon PB. Bile salt biotransformations by human intestinal bacteria. J Lipid Res. 2006;47(2):241–259. - PubMed
-
- Slattery SA, Niaz O, Aziz Q, Ford AC, Farmer AD. Systematic review with meta-analysis: the prevalence of bile acid malabsorption in the irritable bowel syndrome with diarrhoea. Aliment Pharmacol Ther. 2015;42(1):3–11. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

