Multidrug- and Carbapenem-Resistant Pseudomonas aeruginosa in Children, United States, 1999-2012
- PMID: 27856730
- PMCID: PMC5907855
- DOI: 10.1093/jpids/piw064
Multidrug- and Carbapenem-Resistant Pseudomonas aeruginosa in Children, United States, 1999-2012
Abstract
Background: Pseudomonas aeruginosa is a common cause of healthcare-associated infection. Multidrug-resistant (MDR) (>3 classes) and carbapenem-resistant (CR) P aeruginosa are significant threats globally. We used a large reference-laboratory database to study the epidemiology of P aeruginosa in children in the United States.
Methods: Antimicrobial susceptibility data from the Surveillance Network were used to phenotypically identify MDR and CR P aeruginosa isolates in children aged 1 to 17 years between January 1999 and July 2012. Logistic regression analysis was used to calculate trends in the prevalence of MDR and CR P aeruginosa. Isolates from infants (<1 year old) and patients with cystic fibrosis were excluded.
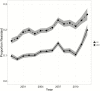
Results: Among the isolates tested, the crude proportion of MDR P aeruginosa increased from 15.4% in 1999 to 26% in 2012, and the proportion of CR P aeruginosa increased from 9.4% in 1999 to 20% in 2012. The proportion of both MDR and CR P aeruginosa increased each year by 4% (odds ratio [OR], 1.04 [95% confidence interval (CI), 1.03-1.04] and 1.04 [95% CI, 1.04-1.05], respectively). In multivariable analysis, both MDR and CR P aeruginosa were more common in the intensive care setting, among children aged 13 to 17 years, in respiratory specimens, and in the West North Central region. In addition, resistance to other antibiotic classes (aminoglycosides, fluoroquinolones, cephalosporins, and piperacillin-tazobactam) often used to treat P aeruginosa increased.
Conclusions: Rates of MDR and CR P aeruginosa infection in children are rising nationally. Aggressive prevention strategies, including instituting antimicrobial stewardship programs in pediatric settings, are essential for combating antimicrobial resistance.
Keywords: Pseudomonas aeruginosa; carbapenems; child; drug resistance; epidemiology.
© The Author 2016. Published by Oxford University Press on behalf of The Journal of the Pediatric Infectious Diseases Society. All rights reserved. For permissions, please e-mail: journals.permissions@oup.com.
Figures
References
-
- Bonomo RA, Szabo D. Mechanisms of multidrug resistance in Acinetobacter species and Pseudomonas aeruginosa. Clin Infect Dis 2006; 43(Suppl 2):S49–56. - PubMed
-
- Centers for Disease Control and Prevention. Antibiotic resistance threats in the United States. Atlanta, GA: Center for Disease Control and Prevention; 2013: pp 1–114.
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

