Unusual phenotype of pathologically confirmed progressive supranuclear palsy with autonomic dysfunction and cerebellar ataxia: Case report
- PMID: 27861346
- PMCID: PMC5120903
- DOI: 10.1097/MD.0000000000005237
Unusual phenotype of pathologically confirmed progressive supranuclear palsy with autonomic dysfunction and cerebellar ataxia: Case report
Abstract
Background: Based on the results of recent multicenter clinical-pathological studies, it seems that the clinical heterogeneity of progressive supranuclear palsy (PSP) is much broader than previously thought. We will report 2 cases of patients with unusual manifestation of pathologically confirmed PSP.
Methods: Two female patients were diagnosed with the parkinsonian phenotype of multiple system atrophy (MSAP) according to current clinical diagnostic criteria at the ages of 55 and 60 years, respectively. The patients were followed up for the next 5 and 7 years. In both cases, a detailed neuropathological examination of the brain was conducted postmortem.
Results: In the first case, the overall pathological picture corresponded with the diagnosis of 4R tauopathy. In the second case, the brain pathology corresponded with a combination of 4R tauopathy and neocortical amyloidopathy.
Conclusion: Some of the main symptoms of MSA, such as cerebellar ataxia and orthostatic hypotension, are not rare parts of the clinical picture of PSP. PSP can thus be mistakenly diagnosed as MSA. In order to determine the most accurate clinical diagnosis of PSP, a revision of its current clinical diagnostic criteria seems appropriate.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures
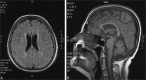



Similar articles
-
Early clinical features of patients with progressive supranuclear palsy with predominant cerebellar ataxia.Parkinsonism Relat Disord. 2013 Dec;19(12):1149-51. doi: 10.1016/j.parkreldis.2013.07.019. Epub 2013 Aug 3. Parkinsonism Relat Disord. 2013. PMID: 23916652
-
Cerebellar ataxia in progressive supranuclear palsy: An autopsy study of PSP-C.Mov Disord. 2016 May;31(5):653-62. doi: 10.1002/mds.26499. Epub 2016 Feb 3. Mov Disord. 2016. PMID: 26841329 Free PMC article.
-
Progressive supranuclear palsy phenotype mimicking synucleinopathies.J Neurol Sci. 2013 Jun 15;329(1-2):34-7. doi: 10.1016/j.jns.2013.03.008. Epub 2013 Apr 13. J Neurol Sci. 2013. PMID: 23590894
-
The phenotypic spectrum of progressive supranuclear palsy.Parkinsonism Relat Disord. 2016 Jan;22 Suppl 1:S34-6. doi: 10.1016/j.parkreldis.2015.09.041. Epub 2015 Sep 25. Parkinsonism Relat Disord. 2016. PMID: 26421392 Review.
-
Coexistence of PSP and MSA: a case report and review of the literature.Acta Neuropathol. 2006 Feb;111(2):186-92. doi: 10.1007/s00401-005-0022-z. Epub 2006 Feb 3. Acta Neuropathol. 2006. PMID: 16456665 Review.
Cited by
-
Lewy body disease or diseases with Lewy bodies?NPJ Parkinsons Dis. 2022 Jan 10;8(1):3. doi: 10.1038/s41531-021-00273-9. NPJ Parkinsons Dis. 2022. PMID: 35013341 Free PMC article. Review.
-
Progressive Supranuclear Gaze Palsy with Predominant Cerebellar Ataxia: A Case Series with Videos.J Mov Disord. 2017 May;10(2):87-91. doi: 10.14802/jmd.16059. Epub 2017 Apr 18. J Mov Disord. 2017. PMID: 28415165 Free PMC article.
References
-
- Richardson JC, Steele J, Olszewski J. Supranuclear ophthalmoplegia, pseudobulbar palsy, nuchal dystonia and dementia. A clinical report on eight cases of “heterogenous system degeneration”. Trans Am Neurol Assoc 1963; 88:25–29. - PubMed
-
- Steele JC, Richardson JC, Olszewski J. Progressive supranuclear palsy. A heterogeneous degeneration involving the brain stem, basal ganglia and cerebellum with vertical supranuclear gaze and pseudobulbar palsy, nuchal dystonia and dementia. Arch Neurol 1964; 10:333–359. - PubMed
-
- Litvan I, Hauw JJ, Bartko JJ, et al. Validity and reliability of the preliminary NINDS neuropathologic criteria for progressive supranuclear palsy and related disorders. J Neuropathol Exp Neurol 1996; 55:97–105. - PubMed
-
- Williams DR, de Silva R, Paviour DC, et al. Characteristics of two distinct clinical phenotypes in pathologically proven progressive supranuclear palsy: Richardson's syndrome and PSP-parkinsonism. Brain 2005; 128:1247–1258. - PubMed
-
- Williams DR, Holton JL, Strand K, et al. Pure akinesia with gait freezing: a third clinical phenotype of progressive supranuclear palsy. Mov Disord 2007; 22:2235–2241. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

