Resource utilisation, costs and clinical outcomes in non-institutionalised patients with Alzheimer's disease: 18-month UK results from the GERAS observational study
- PMID: 27887645
- PMCID: PMC5124297
- DOI: 10.1186/s12877-016-0371-6
Resource utilisation, costs and clinical outcomes in non-institutionalised patients with Alzheimer's disease: 18-month UK results from the GERAS observational study
Abstract
Background: Alzheimer's disease (AD), the commonest cause of dementia, represents a significant cost to UK society. This analysis describes resource utilisation, costs and clinical outcomes in non-institutionalised patients with AD in the UK.
Methods: The GERAS prospective observational study assessed societal costs associated with AD for patients and caregivers over 18 months, stratified according to baseline disease severity (mild, moderate, or moderately severe/severe [MS/S]). All patients enrolled had an informal caregiver willing to participate in the study. Healthcare resource utilisation was measured using the Resource Utilization in Dementia instrument, and 18-month costs estimated by applying unit costs of services and products (2010 values). Total societal costs were calculated using an opportunity cost approach.
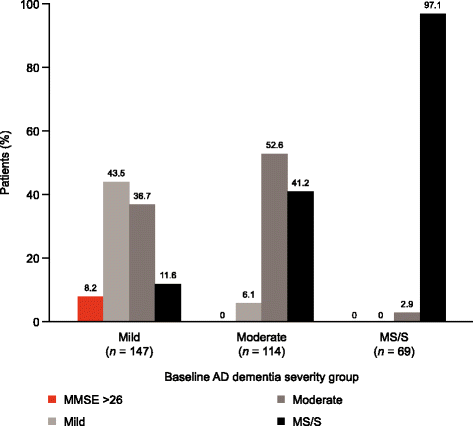
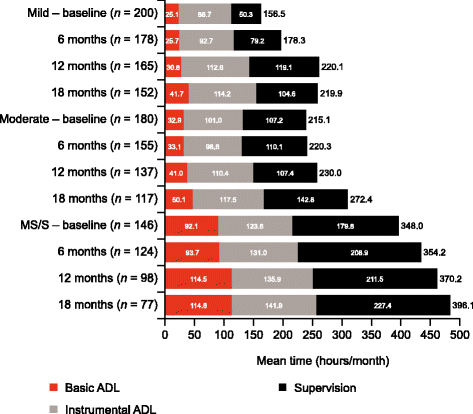
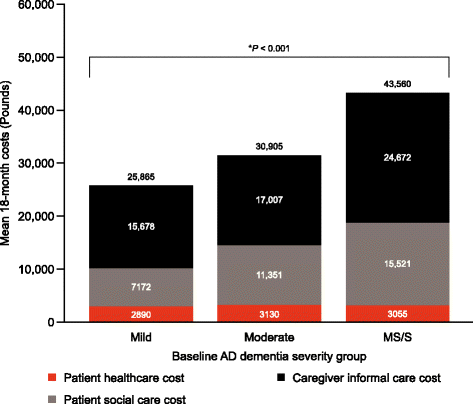
Results: Overall, 526 patients (200 mild, 180 moderate and 146 MS/S at baseline) were recruited from 24 UK centres. Mini-Mental State Examination (MMSE) scores deteriorated most markedly in the MS/S patient group, with declines of 3.6 points in the mild group, 3.5 points in the moderate group and 4.7 points in the MS/S group; between-group differences did not reach statistical significance. Patients with MS/S AD dementia at baseline were more likely to be institutionalised (Kaplan-Meier probability 28% versus 9% in patients with mild AD dementia; p < 0.001 for difference across all severities) and had a greater probability of death (Kaplan-Meier probability 15% versus 5%; p = 0.013) at 18 months. Greater disease severity at baseline was also associated with concomitant increases in caregiver time and mean total societal costs. Total societal costs of £43,560 over 18 months were estimated for the MS/S group, versus £25,865 for the mild group and £30,905 for the moderate group (p < 0.001). Of these costs, over 50% were related to informal caregiver costs at each AD dementia severity level.
Conclusions: This study demonstrated a mean deterioration in MMSE score over 18 months in patients with AD. It also showed that AD is a costly disease, with costs increasing with disease severity, even when managed in the community: informal caregiver costs represented the main contributor to societal costs.
Keywords: AD dementia severity; Alzheimer’s disease; Clinical outcomes; MMSE; Resource use; Societal costs.
Figures


Similar articles
-
Costs and Resource Use Associated with Alzheimer's Disease in Italy: Results from an Observational Study.J Prev Alzheimers Dis. 2018;5(1):55-64. doi: 10.14283/jpad.2017.31. J Prev Alzheimers Dis. 2018. PMID: 29405234 Free PMC article.
-
Resource Use and Cost of Alzheimer's Disease in France: 18-Month Results from the GERAS Observational Study.Value Health. 2018 Mar;21(3):295-303. doi: 10.1016/j.jval.2017.09.019. Epub 2017 Nov 11. Value Health. 2018. PMID: 29566836
-
Costs and resource use of community-dwelling patients with Alzheimer's disease in Japan: 18-month results from the GERAS-J study.Curr Med Res Opin. 2021 Aug;37(8):1331-1339. doi: 10.1080/03007995.2021.1922369. Epub 2021 May 20. Curr Med Res Opin. 2021. PMID: 33904362
-
Potential savings in the cost of caring for Alzheimer's disease. Treatment with rivastigmine.Pharmacoeconomics. 2000 Apr;17(4):351-60. doi: 10.2165/00019053-200017040-00005. Pharmacoeconomics. 2000. PMID: 10947490 Review.
-
Rivastigmine. A pharmacoeconomic review of its use in Alzheimer's disease.Pharmacoeconomics. 2001;19(3):303-18. doi: 10.2165/00019053-200119030-00008. Pharmacoeconomics. 2001. PMID: 11303418 Review.
Cited by
-
Potential cost savings to be made by slowing cognitive decline in mild Alzheimer's disease dementia using a model derived from the UK GERAS observational study.BMC Geriatr. 2018 Feb 23;18(1):57. doi: 10.1186/s12877-018-0748-9. BMC Geriatr. 2018. PMID: 29471784 Free PMC article.
-
Major Cost Drivers in Assessing the Economic Burden of Alzheimer's Disease: A Structured, Rapid Review.J Prev Alzheimers Dis. 2021;8(3):362-370. doi: 10.14283/jpad.2021.17. J Prev Alzheimers Dis. 2021. PMID: 34101795 Free PMC article. Review.
-
Caring for the elderly: A person-centered segmentation approach for exploring the association between health care needs, mental health care use, and costs in Germany.PLoS One. 2019 Dec 19;14(12):e0226510. doi: 10.1371/journal.pone.0226510. eCollection 2019. PLoS One. 2019. PMID: 31856192 Free PMC article.
-
Potential Impact of Slowing Disease Progression in Early Symptomatic Alzheimer's Disease on Patient Quality of Life, Caregiver Time, and Total Societal Costs: Estimates Based on Findings from GERAS-US Study.J Alzheimers Dis. 2024;100(2):563-578. doi: 10.3233/JAD-231166. J Alzheimers Dis. 2024. PMID: 38875031 Free PMC article.
-
Caregiver burden of Alzheimer's disease among informal caregivers: a cross-sectional study in Malaysia.Sci Rep. 2025 Mar 24;15(1):10067. doi: 10.1038/s41598-025-95210-8. Sci Rep. 2025. PMID: 40128538 Free PMC article.
References
-
- Organisation for Economic Co-operation and Development (OECD). Tackling dementia with big data. April 2015. http://www.oecdobserver.org/news/fullstory.php/aid/4828/Tackling_dementi.... Accessed 17 Feb 2016.
-
- Alzheimer’s Society. Dementia UK: update. 2014. http://www.alzheimers.org.uk/site/scripts/download_info.php?fileID=2323. Accessed 17 Feb 2016.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

