Effect of Previous Irradiation on Vascular Thrombosis of Microsurgical Anastomosis: A Preclinical Study in Rats
- PMID: 27975009
- PMCID: PMC5142475
- DOI: 10.1097/GOX.0000000000001073
Effect of Previous Irradiation on Vascular Thrombosis of Microsurgical Anastomosis: A Preclinical Study in Rats
Abstract
Background: The objective of the present investigation was to compare the effect of neoadjuvant irradiation on the microvascular anastomosis in cervical bundle using an experimental model in rats.
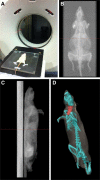
Methods: One hundred forty male Sprague-Dawley rats were allocated into 4 groups: group I, control, arterial microanastomosis; group II, control, venous microanastomosis; group III, arterial microanastomosis with previous irradiation (20 Gy); and group IV, venous microanastomosis with previous irradiation (20 Gy). Clinical parameters, technical values of anastomosis, patency, and histopathological parameters were evaluated.
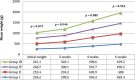
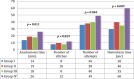
Results: Irradiated groups (III and IV) and vein anastomosis groups (II and IV) showed significantly increased technical difficulties. Group IV showed significantly reduced patency rates (7/35) when compared with the control group (0/35). Radiotherapy significantly decreased the patency rates of the vein (7/35) when compared with the artery (1/35). Groups III and IV showed significantly reduced number of endothelial cells and also showed the presence of intimal thickening and adventitial fibrosis as compared with the control group.
Conclusion: Neoadjuvant radiotherapy reduces the viability of the venous anastomosis in a preclinical rat model with a significant increase in the incidence of vein thrombosis.
Figures






Similar articles
-
Comparative study of isovolemic hemodilution with 3% albumin, dextran-40, and prophylactic enoxaparin (LMWH) on thrombus formation at venous microanastomosis in rats.Microsurgery. 2006;26(6):456-64. doi: 10.1002/micr.20270. Microsurgery. 2006. PMID: 16924631
-
Effect of isovolemic hemodilution with 3% albumin on thrombus formation at venous microanastomosis in rats.Microsurgery. 2002;22(4):152-7. doi: 10.1002/micr.21743. Microsurgery. 2002. PMID: 12111980
-
The effect of prolonged clamping and vascular stasis on the patency of arterial and venous microanastomoses.Ann Plast Surg. 1998 Apr;40(4):436-41. doi: 10.1097/00000637-199804000-00019. Ann Plast Surg. 1998. PMID: 9556001
-
The influence of intraarterial high-dose cisplatin with concomitant irradiation on arterial microanastomosis: an experimental study.Am J Clin Oncol. 2009 Apr;32(2):158-62. doi: 10.1097/COC.0b013e31817f9e00. Am J Clin Oncol. 2009. PMID: 19307956
-
Clinical results of surgery for retroperitoneal sarcoma with major blood vessel involvement.J Vasc Surg. 2006 Jul;44(1):46-55. doi: 10.1016/j.jvs.2006.03.001. J Vasc Surg. 2006. PMID: 16828425 Review.
Cited by
-
Flap Failure and Salvage in Head and Neck Reconstruction.Semin Plast Surg. 2020 Nov;34(4):314-320. doi: 10.1055/s-0040-1721766. Epub 2020 Dec 24. Semin Plast Surg. 2020. PMID: 33380919 Free PMC article. Review.
-
Hyperbaric oxygen therapy outcomes in post-irradiated patient undergoing microvascular breast reconstruction: A preliminary retrospective comparative study.JPRAS Open. 2024 Aug 7;42:1-9. doi: 10.1016/j.jpra.2024.07.017. eCollection 2024 Dec. JPRAS Open. 2024. PMID: 39279849 Free PMC article.
-
Principles of Surgical Treatment of Soft Tissue Sarcomas.Cancers (Basel). 2025 Jan 25;17(3):401. doi: 10.3390/cancers17030401. Cancers (Basel). 2025. PMID: 39941773 Free PMC article. Review.
References
-
- Bengtson BP, Schusterman MA, Baldwin BJ, et al. Influence of prior radiotherapy on the development of postoperative complications and success of free tissue transfers in head and neck cancer reconstruction. Am J Surg. 1993;166:326–330. - PubMed
-
- Choi S, Schwartz DL, Farwell DG, et al. Radiation therapy does not impact local complication rates after free flap reconstruction for head and neck cancer. Arch Otolaryngol Head Neck Surg. 2004;130:1308–1312. - PubMed
-
- Nahabedian MY, Singh N, Deune EG, et al. Recipient vessel analysis for microvascular reconstruction of the head and neck. Ann Plast Surg. 2004;52:148–155. discussion 156. - PubMed
-
- O’Sullivan B, Davis AM, Turcotte R, et al. Preoperative versus postoperative radiotherapy in soft-tissue sarcoma of the limbs: a randomised trial. Lancet. 2002;359:2235–2241. - PubMed
-
- Wang CC, editor. Clinical Radiation Oncology: Indications, Techniques, and Results. 2nd ed. New York, NY: Wiley-Liss, Inc.; 2000.
LinkOut - more resources
Full Text Sources
Other Literature Sources
