Outcomes of an inpatient refeeding protocol in youth with Anorexia Nervosa and atypical Anorexia Nervosa at Children's Hospitals and Clinics of Minnesota
- PMID: 28018595
- PMCID: PMC5165845
- DOI: 10.1186/s40337-016-0124-0
Outcomes of an inpatient refeeding protocol in youth with Anorexia Nervosa and atypical Anorexia Nervosa at Children's Hospitals and Clinics of Minnesota
Abstract
Background: Historically, inpatient protocols have adopted relatively conservative approaches to refeeding in Anorexia Nervosa (AN) in order to reduce the risk of refeeding syndrome, a potentially fatal constellation of symptoms. However, increasing evidence suggests that patients with AN can tolerate higher caloric prescriptions during treatment, which may result in prevention of initial weight loss, shorter hospital stays, and less exposure to the effects of severe malnutrition. Therefore the present study sought to examine the effectiveness of a more accelerated refeeding protocol in an inpatient AN and atypical AN sample.
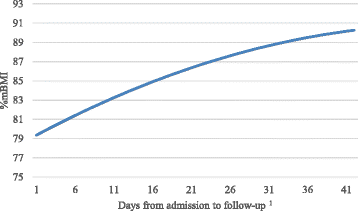
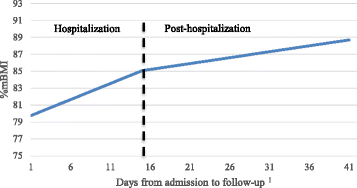
Methods: Participants were youth (ages 10-22) with AN (n = 113) and atypical AN (n = 16) who were hospitalized for medical stabilization. A retrospective chart review was conducted to assess changes in calories, weight status (percentage of median BMI, %mBMI), and indicators of refeeding syndrome, specifically hypophosphatemia, during hospitalization. Weight was assessed again approximately 4 weeks after discharge.
Results: No cases of refeeding syndrome were observed, though 47.3 % of participants evidenced hypophosphatemia during treatment. Phosphorous levels were monitored in all participants, and 77.5 % were prescribed supplemental phosphorous at the time of discharge. Higher rates of caloric changes were predictive of greater changes in %mBMI during hospitalization. Rates of caloric and weight change were not related to an increased likelihood of re-admission.
Conclusions: Results suggest that a more accelerated approach to inpatient refeeding in youth with AN and atypical AN can be safely implemented and is not associated with refeeding syndrome, provided there is close monitoring and correction of electrolytes. These findings suggest that this approach has the potential to decrease length of stay and burden associated with inpatient hospitalization, while supporting continued progress after hospitalization.
Keywords: Adolescents; Anorexia Nervosa; Children; Hypophosphatemia; Refeeding.
Figures
Similar articles
-
Higher caloric intake in hospitalized adolescents with anorexia nervosa is associated with reduced length of stay and no increased rate of refeeding syndrome.J Adolesc Health. 2013 Nov;53(5):573-8. doi: 10.1016/j.jadohealth.2013.05.014. Epub 2013 Jul 3. J Adolesc Health. 2013. PMID: 23830088
-
Short-term outcomes of the study of refeeding to optimize inpatient gains for patients with atypical anorexia nervosa.Int J Eat Disord. 2024 Apr;57(4):859-868. doi: 10.1002/eat.24115. Epub 2024 Jan 5. Int J Eat Disord. 2024. PMID: 38179719 Free PMC article. Clinical Trial.
-
A prospective examination of weight gain in hospitalized adolescents with anorexia nervosa on a recommended refeeding protocol.J Adolesc Health. 2012 Jan;50(1):24-9. doi: 10.1016/j.jadohealth.2011.06.011. Epub 2011 Aug 26. J Adolesc Health. 2012. PMID: 22188830 Free PMC article.
-
Clinical Outcomes of Refeeding Syndrome: A Systematic Review of High vs. Low-Calorie Diets for the Treatment of Anorexia Nervosa and Related Eating Disorders in Children and Adolescents.Cureus. 2023 May 21;15(5):e39313. doi: 10.7759/cureus.39313. eCollection 2023 May. Cureus. 2023. PMID: 37351245 Free PMC article. Review.
-
High-calorie refeeding in adolescents with anorexia nervosa: a narrative review.Acta Gastroenterol Belg. 2024 Apr-Jun;87(2):287-293. doi: 10.51821/87.2.12851. Acta Gastroenterol Belg. 2024. PMID: 39210761 Review.
Cited by
-
An audit of the changes in thiamine levels during higher caloric nutritional rehabilitation of adolescent patients hospitalised with a restrictive eating disorder.J Eat Disord. 2020 Sep 1;8:41. doi: 10.1186/s40337-020-00318-z. eCollection 2020. J Eat Disord. 2020. PMID: 32884809 Free PMC article.
-
Outcomes of a Standardized, High-Caloric, Inpatient Re-Alimentation Treatment Protocol in 120 Severely Malnourished Adolescents with Anorexia Nervosa.J Clin Med. 2022 May 5;11(9):2585. doi: 10.3390/jcm11092585. J Clin Med. 2022. PMID: 35566710 Free PMC article.
-
Study protocol for a randomised controlled trial investigating two different refeeding formulations to improve safety and efficacy of hospital management of adolescent and young adults admitted with anorexia nervosa.BMJ Open. 2020 Oct 7;10(10):e038242. doi: 10.1136/bmjopen-2020-038242. BMJ Open. 2020. PMID: 33033021 Free PMC article.
-
Comparison of metabolic parameters between oral and total parenteral nutrition in children with severe eating disorders.Fukushima J Med Sci. 2024 Apr 26;70(2):75-85. doi: 10.5387/fms.2023-02. Epub 2024 Apr 9. Fukushima J Med Sci. 2024. PMID: 38599829 Free PMC article.
-
The gut microbiome in anorexia nervosa: relevance for nutritional rehabilitation.Psychopharmacology (Berl). 2019 May;236(5):1545-1558. doi: 10.1007/s00213-018-5159-2. Epub 2019 Jan 5. Psychopharmacology (Berl). 2019. PMID: 30612189 Free PMC article. Review.
References
-
- Golden NH, Katzman DK, Kreipe RE, Stevens SL, Sawyer SM, Rees J, et al. Eating disorders in adolescents: position paper of the Society for Adolescent Medicine. J Adolesc Health. 2003;33(6):496–503. - PubMed
-
- Zhao Y, Encinosa W. An Update on Hospitalizations for Eating Disorders, 1999 to 2009: Statistical Brief #120. Rockville: Healthcare Cost and Utilization Project (HCUP) Statistical Briefs; 2011.
LinkOut - more resources
Full Text Sources
Other Literature Sources

