Validation and Modification of a Prediction Model for Acute Cardiac Events in Patients With Breast Cancer Treated With Radiotherapy Based on Three-Dimensional Dose Distributions to Cardiac Substructures
- PMID: 28095159
- PMCID: PMC5455600
- DOI: 10.1200/JCO.2016.69.8480
Validation and Modification of a Prediction Model for Acute Cardiac Events in Patients With Breast Cancer Treated With Radiotherapy Based on Three-Dimensional Dose Distributions to Cardiac Substructures
Erratum in
-
Errata.J Clin Oncol. 2017 Nov 10;35(32):3736. doi: 10.1200/JCO.2017.76.2732. J Clin Oncol. 2017. PMID: 29112825 Free PMC article. No abstract available.
Abstract
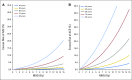
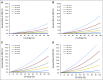
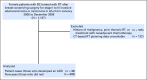
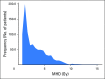
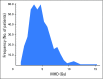
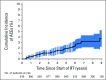
Purpose A relationship between mean heart dose (MHD) and acute coronary event (ACE) rate was reported in a study of patients with breast cancer (BC). The main objective of our cohort study was to validate this relationship and investigate if other dose-distribution parameters are better predictors for ACEs than MHD. Patients and Methods The cohort consisted of 910 consecutive female patients with BC treated with radiotherapy (RT) after breast-conserving surgery. The primary end point was cumulative incidence of ACEs within 9 years of follow-up. Both MHD and various dose-distribution parameters of the cardiac substructures were collected from three-dimensional computed tomography planning data. Results The median MHD was 2.37 Gy (range, 0.51 to 15.25 Gy). The median follow-up time was 7.6 years (range, 0.1 to 10.1 years), during which 30 patients experienced an ACE. The cumulative incidence of ACE increased by 16.5% per Gy (95% CI, 0.6 to 35.0; P = .042). Analysis showed that the volume of the left ventricle receiving 5 Gy (LV-V5) was the most important prognostic dose-volume parameter. The most optimal multivariable normal tissue complication probability model for ACEs consisted of LV-V5, age, and weighted ACE risk score per patient (c-statistic, 0.83; 95% CI, 0.75 to 0.91). Conclusion A significant dose-effect relationship was found for ACEs within 9 years after RT. Using MHD, the relative increase per Gy was similar to that reported in the previous study. In addition, LV-V5 seemed to be a better predictor for ACEs than MHD. This study confirms the importance of reducing exposure of the heart to radiation to avoid excess risk of ACEs after radiotherapy for BC.
Figures



Comment in
-
Radiation-Induced Heart Disease After Breast Cancer Treatment: How Big a Problem, and How Much Can-and Should-We Try to Reduce It?J Clin Oncol. 2017 Apr 10;35(11):1146-1148. doi: 10.1200/JCO.2016.71.4113. Epub 2017 Jan 17. J Clin Oncol. 2017. PMID: 28095154 No abstract available.
-
Cardiac Morbidity and Radiation Therapy for Breast Cancer.Int J Radiat Oncol Biol Phys. 2018 Feb 1;100(2):283-286. doi: 10.1016/j.ijrobp.2017.06.2443. Int J Radiat Oncol Biol Phys. 2018. PMID: 29353643 No abstract available.
References
-
- Clarke M, Collins R, Darby S, et al. Effects of radiotherapy and of differences in the extent of surgery for early breast cancer on local recurrence and 15-year survival: An overview of the randomised trials. Lancet. 2005;366:2087–2106. - PubMed
-
- Zagar TM, Marks LB. Breast cancer: Risk of heart disease after radiotherapy-cause for concern. Nat Rev Clin Oncol. 2013;10:310–312. - PubMed
-
- Boero IJ, Paravati AJ, Triplett DP, et al. Modern radiation therapy and cardiac outcomes in breast cancer. Int J Radiat Oncol Biol Phys. 2016;94:700–708. - PubMed
-
- Boekel NB, Schaapveld M, Gietema JA, et al. Cardiovascular disease risk in a large, population-based cohort of breast cancer survivors. Int J Radiat Oncol Biol Phys. 2016;94:1061–1072. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

