(Re)Building a Kidney
- PMID: 28096308
- PMCID: PMC5407737
- DOI: 10.1681/ASN.2016101077
(Re)Building a Kidney
Abstract
(Re)Building a Kidney is a National Institute of Diabetes and Digestive and Kidney Diseases-led consortium to optimize approaches for the isolation, expansion, and differentiation of appropriate kidney cell types and the integration of these cells into complex structures that replicate human kidney function. The ultimate goals of the consortium are two-fold: to develop and implement strategies for in vitro engineering of replacement kidney tissue, and to devise strategies to stimulate regeneration of nephrons in situ to restore failing kidney function. Projects within the consortium will answer fundamental questions regarding human gene expression in the developing kidney, essential signaling crosstalk between distinct cell types of the developing kidney, how to derive the many cell types of the kidney through directed differentiation of human pluripotent stem cells, which bioengineering or scaffolding strategies have the most potential for kidney tissue formation, and basic parameters of the regenerative response to injury. As these projects progress, the consortium will incorporate systematic investigations in physiologic function of in vitro and in vivo differentiated kidney tissue, strategies for engraftment in experimental animals, and development of therapeutic approaches to activate innate reparative responses.
Keywords: Directed differentiation; Organogenesis; Organoid; Regeneration.
Copyright © 2017 by the American Society of Nephrology.
Figures



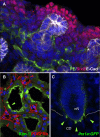
References
-
- Stevens PE, Levin A; Kidney Disease: Improving Global Outcomes Chronic Kidney Disease Guideline Development Work Group Members : Evaluation and management of chronic kidney disease: Synopsis of the kidney disease: Improving global outcomes 2012 clinical practice guideline. Ann Intern Med 158: 825–830, 2013 - PubMed
-
- Freedman BS, Brooks CR, Lam AQ, Fu H, Morizane R, Agrawal V, Saad AF, Li MK, Hughes MR, Werff RV, Peters DT, Lu J, Baccei A, Siedlecki AM, Valerius MT, Musunuru K, McNagny KM, Steinman TI, Zhou J, Lerou PH, Bonventre JV: Modelling kidney disease with CRISPR-mutant kidney organoids derived from human pluripotent epiblast spheroids. Nat Commun 6: 8715, 2015 - PMC - PubMed
MeSH terms
Grants and funding
- DP3 DK108215/DK/NIDDK NIH HHS/United States
- I01 BX002660/BX/BLRD VA/United States
- UH2 DK107343/DK/NIDDK NIH HHS/United States
- UH2 DK107344/DK/NIDDK NIH HHS/United States
- UH3 DK107357/DK/NIDDK NIH HHS/United States
- U01 DK107350/DK/NIDDK NIH HHS/United States
- UH2 DK107374/DK/NIDDK NIH HHS/United States
- R24 DK106743/DK/NIDDK NIH HHS/United States
- R37 DK054364/DK/NIDDK NIH HHS/United States
- U01 DK094526/DK/NIDDK NIH HHS/United States
- UH2 DK107357/DK/NIDDK NIH HHS/United States
- UH3 DK107372/DK/NIDDK NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

