Impaired Glucose Homeostasis in First-Episode Schizophrenia: A Systematic Review and Meta-analysis
- PMID: 28097367
- PMCID: PMC6352957
- DOI: 10.1001/jamapsychiatry.2016.3803
Impaired Glucose Homeostasis in First-Episode Schizophrenia: A Systematic Review and Meta-analysis
Abstract
Importance: Schizophrenia is associated with an increased risk of type 2 diabetes. However, it is not clear whether schizophrenia confers an inherent risk for glucose dysregulation in the absence of the effects of chronic illness and long-term treatment.
Objective: To conduct a meta-analysis examining whether individuals with first-episode schizophrenia already exhibit alterations in glucose homeostasis compared with controls.
Data sources: The EMBASE, MEDLINE, and PsycINFO databases were systematically searched for studies examining measures of glucose homeostasis in antipsychotic-naive individuals with first-episode schizophrenia compared with individuals serving as controls.
Study selection: Case-control studies reporting on fasting plasma glucose levels, plasma glucose levels after an oral glucose tolerance test, fasting plasma insulin levels, insulin resistance, and hemoglobin A1c (HbA1c) levels in first-episode antipsychotic-naive individuals with first-episode schizophrenia compared with healthy individuals serving as controls. Two independent investigators selected the studies.
Data extraction: Two independent investigators extracted study-level data for a random-effects meta-analysis. Standardized mean differences in fasting plasma glucose levels, plasma glucose levels after an oral glucose tolerance test, fasting plasma insulin levels, insulin resistance, and HbA1c levels were calculated. Sensitivity analyses examining the effect of body mass index, diet and exercise, race/ethnicity, and minimal (≤2 weeks) antipsychotic exposure were performed.
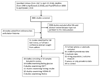
Data synthesis: Of 3660 citations retrieved, 16 case-control studies comprising 15 samples met inclusion criteria. The overall sample included 731 patients and 614 controls. Fasting plasma glucose levels (Hedges g = 0.20; 95% CI, 0.02 to 0.38; P = .03), plasma glucose levels after an oral glucose tolerance test (Hedges g = 0.61; 95% CI, 0.16 to 1.05; P = .007), fasting plasma insulin levels (Hedges g = 0.41; 95% CI, 0.09 to 0.72; P = .01), and insulin resistance (homeostatic model assessment of insulin resistance) (Hedges g = 0.35; 95% CI, 0.14 to 0.55; P = .001) were all significantly elevated in patients compared with controls. However, HbA1c levels (Hedges g = -0.08; CI, -0.34 to 0.18; P = .55) were not altered in patients compared with controls.
Conclusions and relevance: These findings show that glucose homeostasis is altered from illness onset in schizophrenia, indicating that patients are at increased risk of diabetes as a result. This finding has implications for the monitoring and treatment choice for patients with schizophrenia.
Conflict of interest statement
Professor Howes has received investigator-initiated research funding from and/or participated in advisory/speaker meetings organised by Astra-Zeneca, Autifony, BMS, Eli Lilly, Heptares, Jansenn, Lundbeck, Lyden-Delta, Otsuka, Servier, Sunovion, Rand and Roche. Neither Professor Howes nor his family have been employed by or have holdings/a financial stake in any biomedical company.
Figures


Comment in
-
Diabetes: Linking diabetes and schizophrenia.Nat Rev Endocrinol. 2017 Mar;13(3):126. doi: 10.1038/nrendo.2017.13. Epub 2017 Feb 3. Nat Rev Endocrinol. 2017. PMID: 28155901 No abstract available.
-
First-Episode Schizophrenia and Diabetes Risk.JAMA Psychiatry. 2017 Jul 1;74(7):761-762. doi: 10.1001/jamapsychiatry.2017.0762. JAMA Psychiatry. 2017. PMID: 28538958 No abstract available.
-
First-Episode Schizophrenia and Diabetes Risk.JAMA Psychiatry. 2017 Jul 1;74(7):761. doi: 10.1001/jamapsychiatry.2017.0760. JAMA Psychiatry. 2017. PMID: 28538965 No abstract available.
-
First-Episode Schizophrenia and Diabetes Risk-Reply.JAMA Psychiatry. 2017 Jul 1;74(7):763. doi: 10.1001/jamapsychiatry.2017.0765. JAMA Psychiatry. 2017. PMID: 28538995 No abstract available.
-
First-Episode Schizophrenia and Diabetes Risk.JAMA Psychiatry. 2017 Jul 1;74(7):762-763. doi: 10.1001/jamapsychiatry.2017.0905. JAMA Psychiatry. 2017. PMID: 28539001 No abstract available.
References
-
- Beary M, Hodgson R, Wildgust HJ. A critical review of major mortality risk factors for all-cause mortality in first-episode schizophrenia: clinical and research implications. Journal of Psychopharmacology. 2012;26(S5):52–61. - PubMed
-
- Crump C, Winkleby MA, Sundquist K, Sundquist J. Comorbidities and mortality in persons with schizophrenia: a Swedish national cohort study. Am J Psychiatry. 2013;170(3):324–333. - PubMed
-
- Hoang U, Goldacre MJ, Stewart R. Avoidable mortality in people with schizophrenia or bipolar disorder in England. Acta Psychiatr Scand. 2013;127(3):195–201. - PubMed
-
- Laursen TM, Nordentoft M, Mortensen PB. Excess early mortality in schizophrenia. Annu Rev Clin Psychol. 2014;10:425–448. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

