The Laboratory Diagnosis of Autoimmune Encephalitis
- PMID: 28101474
- PMCID: PMC5206099
- DOI: 10.14581/jer.16010
The Laboratory Diagnosis of Autoimmune Encephalitis
Abstract
Autoimmune encephalitis is a group of encephalitis syndromes that cause altered mentality, memory decline, or seizures in association with the presence of serum and cerebrospinal fluid (CSF) autoantibodies (auto-Abs). An early diagnosis enables early treatments. The detection of auto-Abs is a confirmatory diagnosis. Tissue-based assay, cell-based immunoassay, and immunoblotting are used to detect various autoantibodies. The CSF test for the presence of antibodies is important because it is more sensitive and reflects disease activity in many autoimmune encephalitis, although antibody tests can be negative even in the presence of autoimmune encephalitis. EEG is often abnormal, but nonspecific. A unilateral or bilateral medial temporal T2 high signal is a common finding in MRI. Fludeoxyglucose-positron emission tomography is sometimes useful for diagnosis in patients with normal MRI.
Keywords: Autoantibody; Autoimmune encephalitis; EEG; Imaging; Laboratory diagnosis.
Figures


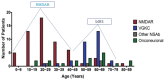

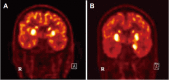
References
-
- Bernal F, Graus F, Pifarré A, Saiz A, Benyahia B, Ribalta T. Immunohistochemical analysis of anti-Hu-associated paraneoplastic encephalomyelitis. Acta Neuropathol. 2002;103:509–15. - PubMed
-
- Bien CG, Vincent A, Barnett MH, et al. Immunopathology of autoanti-body-associated encephalitides: clues for pathogenesis. Brain. 2012;135(Pt 5):1622–38. - PubMed
-
- Darnell RB, Posner JB. Paraneoplastic Syndromes. New York: Oxford; 2011.
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

