A giant and insidious subphrenic biloma formation due to gallbladder perforation mimicking biliary cystic tumor: A case report
- PMID: 28123732
- PMCID: PMC5244985
- DOI: 10.3892/mco.2016.1075
A giant and insidious subphrenic biloma formation due to gallbladder perforation mimicking biliary cystic tumor: A case report
Abstract
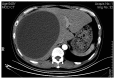
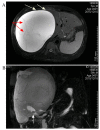
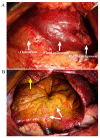
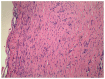
Gallbladder perforation (GBP) represents a rare, but potentially life-threatening, complication of acute cholecystitis. GBP is subdivided into three categories whereas the development of biloma is extremely rare. The present case study reports on a 40-year-old man with a 10-year history of calculus cholecystitis, who was referred to The First Affiliated Hospital of Nanjing Medical University (Nanjing, China) for the surgical treatment of an emerging massive hepatic entity with insidious symptoms and normal laboratory tests. A preoperative imaging study demonstrated the collection with internal septations and mural nodules, but no visible communication with the biliary system. Given the suspected biliary cystic tumor, a laparotomy was performed and the lumen was scattered with papillae. An intraoperative frozen section examination illustrated a simple hepatic cyst. Biochemical analysis of the collection and histopathology of the gallbladder and capsule substantiated the diagnosis of biloma formation due to GBP. The purpose of the present case report was to demonstrate how a pinhole-sized perforation with extravasation of unconcentrated bile from the gallbladder may result in insidious clinical presentation and an undetected leak site. According to the clinicopathological characteristics and composition, formation of biloma should be classified as type IV GBP. To differentiate bilomas with intracystic septations and mural nodules from BCTs is difficult via a preoperative examination, and the definitive diagnosis should be based on a histological examination. Laparotomy with frozen section examination may be the optimal approach in such a case.
Keywords: biliary cystic tumor; biloma; calculus cholecystitis; gallbladder perforation; insidious symptoms.
Figures
References
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
