Laboratory confirmed miltefosine resistant cases of visceral leishmaniasis from India
- PMID: 28137296
- PMCID: PMC5282768
- DOI: 10.1186/s13071-017-1969-z
Laboratory confirmed miltefosine resistant cases of visceral leishmaniasis from India
Abstract
Background: Miltefosine unresponsive and relapse cases of visceral leishmaniasis (VL) are increasingly being reported. However, there has been no laboratory confirmed reports of miltefosine resistance in VL. Here, we report two laboratory confirmed cases of VL from India.
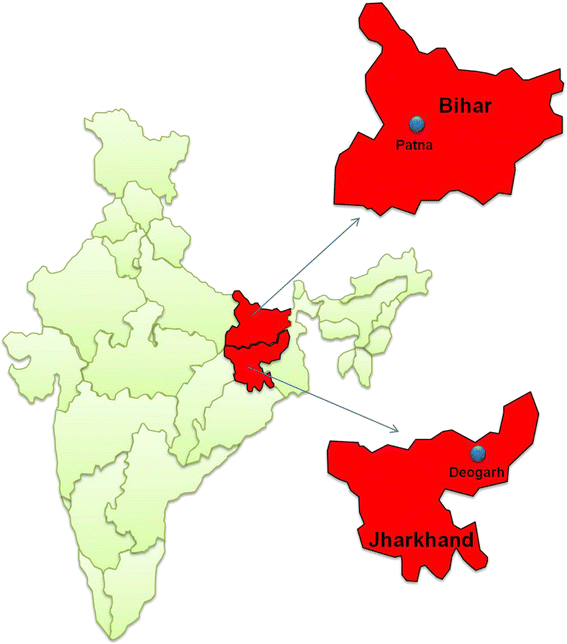
Methods: Two patients with VL were referred to us with suspected VL. The first patient was a native of the VL endemic state of Bihar, but residing in Delhi, a VL non-endemic area. He was treated with broad-spectrum antibiotics and antipyretics but was unresponsive to treatment. The second patient was from Jharkhand state in eastern India (adjoining Bihar), another endemic state for VL. He was refractory to anti-leishmanial treatment, which included administration of miltefosine. Following investigation, both patients were serologically positive for VL, and blood buffy coat from both patients grew Leishmania donovani. The isolates derived from both cases were characterized for their drug susceptibility, genetically characterised, and SNPs typed for LdMT and LdROS gene expression. Both patients were successfully treated with amphotericin B.
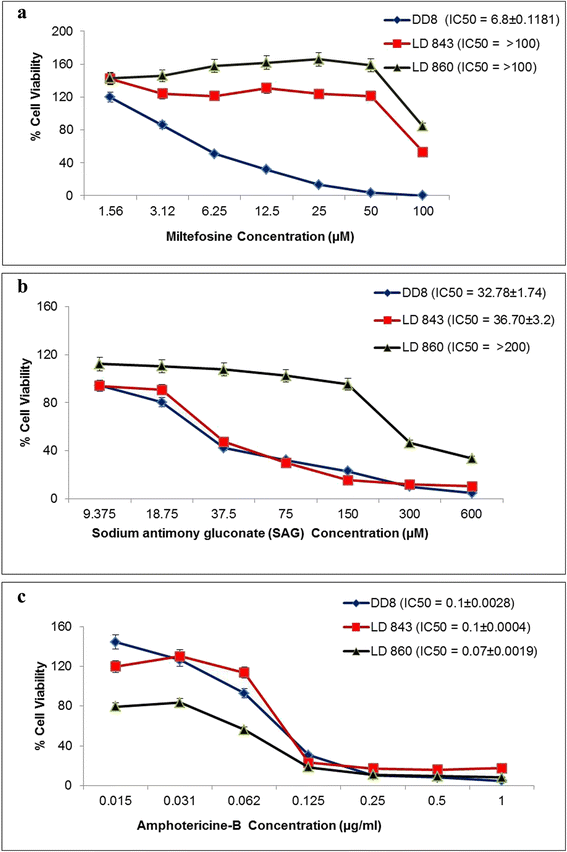
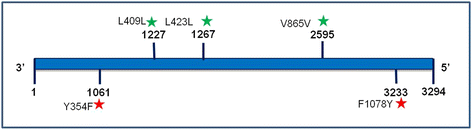
Results: The in vitro drug susceptibility assays carried out on both isolates showed good IC50 values to amphotericin B (0.1 ± 0.0004 μg/ml and 0.07 ± 0.0019 μg/ml). One isolate was refractory to SbIII with an IC50 of > 200 μM while the second isolate was sensitive to SbIII with an IC50 of 36.70 ± 3.2 μM. However, in both the isolates, IC50 against miltefosine was more than 10-fold higher (> 100 μM) than the standard strain DD8 (6.8 ± 0.1181 μM). Furthermore, genetic analyses demonstrated single nucleotide polymorphisms (SNPs) (354Tyr↔Phe and 1078Phe↔Tyr) in the LdMT gene of the parasites.
Conclusions: Here, we document two laboratory confirmed cases of miltefosine resistant VL from India. Our finding highlights the urgent need to establish control measures to prevent the spread of these strains. We also propose that LdMT gene mutation analysis could be used as a molecular marker of miltefosine resistance in L. donovani.
Keywords: Bihar; Drug resistance; Jharkhand; Miltefosine; Visceral leishmaniasis.
Figures


Similar articles
-
Drug susceptibility in Leishmania isolates following miltefosine treatment in cases of visceral leishmaniasis and post kala-azar dermal leishmaniasis.PLoS Negl Trop Dis. 2012;6(5):e1657. doi: 10.1371/journal.pntd.0001657. Epub 2012 May 22. PLoS Negl Trop Dis. 2012. PMID: 22629478 Free PMC article.
-
Antimony susceptible Leishmania donovani: evidence from in vitro drug susceptibility of parasites isolated from patients of post-kala-azar dermal leishmaniasis in pre- and post-miltefosine era.Microbiol Spectr. 2024 Jun 4;12(6):e0402623. doi: 10.1128/spectrum.04026-23. Epub 2024 May 7. Microbiol Spectr. 2024. PMID: 38712926 Free PMC article.
-
The overexpression of genes of thiol metabolism contribute to drug resistance in clinical isolates of visceral leishmaniasis (kala azar) in India.Parasit Vectors. 2014 Dec 17;7:596. doi: 10.1186/s13071-014-0596-1. Parasit Vectors. 2014. PMID: 25515494 Free PMC article.
-
Evaluating drug resistance in visceral leishmaniasis: the challenges.Parasitology. 2018 Apr;145(4):453-463. doi: 10.1017/S0031182016002031. Epub 2016 Nov 21. Parasitology. 2018. PMID: 27866478 Free PMC article. Review.
-
Chemotherapeutics of visceral leishmaniasis: present and future developments.Parasitology. 2018 Apr;145(4):481-489. doi: 10.1017/S0031182017002116. Epub 2017 Dec 7. Parasitology. 2018. PMID: 29215329 Free PMC article. Review.
Cited by
-
Metabolite Biomarkers of Leishmania Antimony Resistance.Cells. 2021 Apr 30;10(5):1063. doi: 10.3390/cells10051063. Cells. 2021. PMID: 33946139 Free PMC article.
-
Discovery of pyrazolopyrrolidinones as potent, broad-spectrum inhibitors of Leishmania infection.Front Trop Dis. 2023;3:1011124. doi: 10.3389/fitd.2022.1011124. Epub 2023 Jan 23. Front Trop Dis. 2023. PMID: 36818551 Free PMC article.
-
Genomic and Transcriptomic Analysis for Identification of Genes and Interlinked Pathways Mediating Artemisinin Resistance in Leishmania donovani.Genes (Basel). 2020 Nov 17;11(11):1362. doi: 10.3390/genes11111362. Genes (Basel). 2020. PMID: 33213096 Free PMC article.
-
Therapeutic Modalities in Post Kala-azar Dermal Leishmaniasis: A Systematic Review of the Effectiveness and Safety of the Treatment Options.Indian J Dermatol. 2021 Jan-Feb;66(1):34-43. doi: 10.4103/ijd.IJD_264_20. Indian J Dermatol. 2021. PMID: 33911291 Free PMC article.
-
Therapeutic Activity of a Topical Formulation Containing 8-Hydroxyquinoline for Cutaneous Leishmaniasis.Pharmaceutics. 2023 Nov 8;15(11):2602. doi: 10.3390/pharmaceutics15112602. Pharmaceutics. 2023. PMID: 38004580 Free PMC article.
References
-
- Berman J. Visceral leishmaniasis in the New World and Africa. Indian J Med Res. 2006;123:289–94. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

