Evaluation, Diagnosis, and Medical Management of Rectal Prolapse
- PMID: 28144208
- PMCID: PMC5179269
- DOI: 10.1055/s-0036-1593431
Evaluation, Diagnosis, and Medical Management of Rectal Prolapse
Abstract
Full-thickness rectal prolapse, or procidentia, is the passage of the full-thickness wall of the rectum beyond the anal sphincters. This condition results in pain and fecal incontinence which greatly impairs the quality of life of those afflicted. It is associated with several anatomic abnormalities, including decreased anal sphincter tone, levator muscle diastasis, and a deep anterior cul-de-sac. The diagnosis of rectal prolapse is made based on physical examination, although several other modalities are used to provide additional information about the patients' condition. While medical management of rectal prolapse can be effective in some cases, the mainstay of management of rectal prolapse is surgical correction.
Keywords: procidentia; rectal prolapse.
Figures


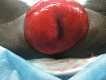




References
-
- Kairaluoma M V, Kellokumpu I H. Epidemiologic aspects of complete rectal prolapse. Scand J Surg. 2005;94(3):207–210. - PubMed
-
- Corman M L. Philadelphia, PA: Lippincott Williams & Wilkins; 2004. Rectal prolapse, solitary rectal ulcer, syndrome of the descending perineum, and rectocele; p. 1408.
-
- Marceau C, Parc Y, Debroux E, Tiret E, Parc R. Complete rectal prolapse in young patients: psychiatric disease a risk factor of poor outcome. Colorectal Dis. 2005;7(4):360–365. - PubMed
-
- Wassef R, Rothenberger D A, Goldberg S M. Rectal prolapse. Curr Probl Surg. 1986;23(6):397–451. - PubMed
-
- Madoff R D, Mellgren A. One hundred years of rectal prolapse surgery. Dis Colon Rectum. 1999;42(4):441–450. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

