Morbidity and mortality among very preterm singletons following fertility treatment in Australia and New Zealand, a population cohort study
- PMID: 28148237
- PMCID: PMC5288897
- DOI: 10.1186/s12884-017-1235-6
Morbidity and mortality among very preterm singletons following fertility treatment in Australia and New Zealand, a population cohort study
Abstract
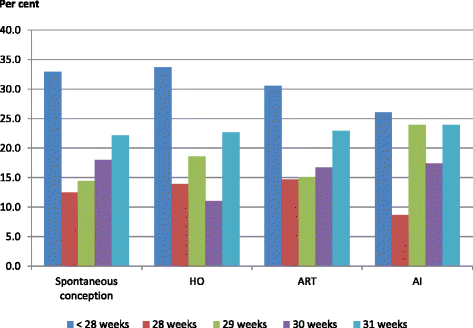
Background: Due to high rates of multiple birth and preterm birth following fertility treatment, the rates of mortality and morbidity among births following fertility treatment were higher than those conceived spontaneously. However, it is unclear whether the rates of adverse neonatal outcomes remain higher for very preterm (<32 weeks gestational age) singletons born after fertility treatment. This study aims to compare adverse neonatal outcomes among very preterm singletons born after fertility treatment including assisted reproductive technology (ART) hyper-ovulution (HO) and artificial insemination (AI) to those following spontaneous conception.
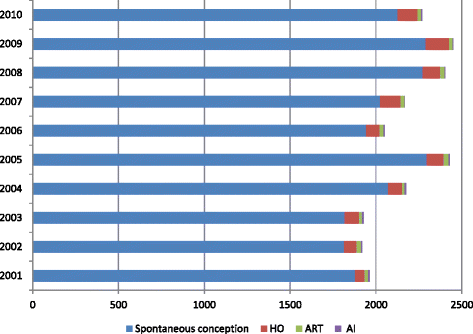
Methods: The population cohort study included 24069 liveborn very preterm singletons who were admitted to Neonatal Intensive Care Unit (NICU) in Australia and New Zealand from 2000 to 2010. The in-hospital neonatal mortality and morbidity among 21753 liveborn very preterm singletons were compared by maternal mode of conceptions: spontaneous conception, HO, ART and AI. Univariate and multivariate binary logistic regression analysis was used to examine the association between mode of conception and various outcome factors. Odds ratio (OR) and adjusted odds ratio (AOR) and 95% confidence interval (CI) were calculated.
Results: The rate of small for gestational age was significantly higher in HO group (AOR 1.52, 95% CI 1.02-2.67) and AI group (AOR 2.98, 95% CI 1.53-5.81) than spontaneous group. The rate of birth defect was significantly higher in ART group (AOR 1.71, 95% CI 1.36-2.16) and AI group (AOR 3.01, 95% CI 1.47-6.19) compared to spontaneous group. Singletons following ART had 43% increased odds of necrotizing enterocolitis (AOR 1.43, 95% CI 1.04-1.97) and 71% increased odds of major surgery (AOR 1.71, 95% CI 1.37-2.13) compared to singletons conceived spontaneously. Other birth and NICU outcomes were not different among the comparison groups.
Conclusions: Compared to the spontaneous conception group, risk of congenital abnormality significantly increases after ART and AI; the risk of morbidities increases after ART, HO and AI. Preconception planning should include comprehensive information about the benefits and risks of fertility treatment on the neonatal outcomes.
Keywords: Artificial insemination; Assisted reproductive technology; Hyper-ovulation; Preterm birth; Very preterm birth.
Figures
Similar articles
-
Gestational age-specific perinatal mortality rates for assisted reproductive technology (ART) and other births.Hum Reprod. 2018 Feb 1;33(2):320-327. doi: 10.1093/humrep/dex340. Hum Reprod. 2018. PMID: 29140454
-
Assisted reproductive technology and perinatal outcomes: conventional versus discordant-sibling design.Fertil Steril. 2016 Sep 1;106(3):710-716.e2. doi: 10.1016/j.fertnstert.2016.04.038. Epub 2016 May 14. Fertil Steril. 2016. PMID: 27187051
-
Assisted reproductive technology surveillance--United States, 2011.MMWR Surveill Summ. 2014 Nov 21;63(10):1-28. MMWR Surveill Summ. 2014. PMID: 25412164
-
The associations of birth intervals with small-for-gestational-age, preterm, and neonatal and infant mortality: a meta-analysis.BMC Public Health. 2013;13 Suppl 3(Suppl 3):S3. doi: 10.1186/1471-2458-13-S3-S3. Epub 2013 Sep 17. BMC Public Health. 2013. PMID: 24564484 Free PMC article. Review.
-
Assisted reproductive technologies: a hierarchy of risks for conception, pregnancy outcomes and treatment decisions.J Dev Orig Health Dis. 2017 Aug;8(4):443-447. doi: 10.1017/S2040174417000526. J Dev Orig Health Dis. 2017. PMID: 28721836 Review.
Cited by
-
Assisted reproductive techniques do not impact late neurodevelopmental outcomes of preterm children.Front Pediatr. 2023 Jun 19;11:1123183. doi: 10.3389/fped.2023.1123183. eCollection 2023. Front Pediatr. 2023. PMID: 37404562 Free PMC article.
-
Generation and Breeding of EGFP-Transgenic Marmoset Monkeys: Cell Chimerism and Implications for Disease Modeling.Cells. 2021 Feb 27;10(3):505. doi: 10.3390/cells10030505. Cells. 2021. PMID: 33673402 Free PMC article.
-
The Role of Extracellular Vesicles in the Developing Brain: Current Perspective and Promising Source of Biomarkers and Therapy for Perinatal Brain Injury.Front Neurosci. 2021 Sep 24;15:744840. doi: 10.3389/fnins.2021.744840. eCollection 2021. Front Neurosci. 2021. PMID: 34630028 Free PMC article. Review.
-
Acute Kidney Injury in Pregnancy: The Need for Higher Awareness. A Pragmatic Review Focused on What Could Be Improved in the Prevention and Care of Pregnancy-Related AKI, in the Year Dedicated to Women and Kidney Diseases.J Clin Med. 2018 Oct 1;7(10):318. doi: 10.3390/jcm7100318. J Clin Med. 2018. PMID: 30275392 Free PMC article. Review.
-
Neonatal outcomes in singleton pregnancies conceived by fresh or frozen embryo transfer compared to spontaneous conceptions: a systematic review and meta-analysis.Arch Gynecol Obstet. 2020 Jul;302(1):31-45. doi: 10.1007/s00404-020-05593-4. Epub 2020 May 22. Arch Gynecol Obstet. 2020. PMID: 32445067 Free PMC article.
References
-
- Hilder LZZ, Parker M, Jahan S, Chambers GM. 014. Australia’s mothers and babies 2012. Perinatal statistics series no. 30. Cat. no. PER 69. Canberra: AIHW; 2014.
-
- Blencowe H, Cousens S, Oestergaard MZ, Chou D, Moller AB, Narwal R, et al. National, regional, and worldwide estimates of preterm birth rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. Lancet. 2012;379(9832):2162–2172. doi: 10.1016/S0140-6736(12)60820-4. - DOI - PubMed
-
- Chow SSW. Report of the Australian and New Zealand Neonatal Network 2012. Sydney: ANZNN; 2014.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical