Photodynamic therapy monitoring with optical coherence angiography
- PMID: 28148963
- PMCID: PMC5288644
- DOI: 10.1038/srep41506
Photodynamic therapy monitoring with optical coherence angiography
Abstract
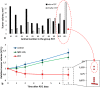
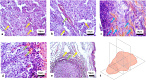
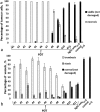
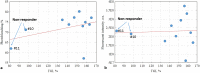
Photodynamic therapy (PDT) is a promising modern approach for cancer therapy with low normal tissue toxicity. This study was focused on a vascular-targeting Chlorine E6 mediated PDT. A new angiographic imaging approach known as M-mode-like optical coherence angiography (MML-OCA) was able to sensitively detect PDT-induced microvascular alterations in the mouse ear tumour model CT26. Histological analysis showed that the main mechanisms of vascular PDT was thrombosis of blood vessels and hemorrhage, which agrees with angiographic imaging by MML-OCA. Relationship between MML-OCA-detected early microvascular damage post PDT (within 24 hours) and tumour regression/regrowth was confirmed by histology. The advantages of MML-OCA such as direct image acquisition, fast processing, robust and affordable system opto-electronics, and label-free high contrast 3D visualization of the microvasculature suggest attractive possibilities of this method in practical clinical monitoring of cancer therapies with microvascular involvement.
Conflict of interest statement
The authors declare no competing financial interests.
Figures


References
-
- Wilson B. C. & Patterson M. S. The physics, biophysics and technology of photodynamic therapy. Phys Med Biol 53, R61–R109 (2008). - PubMed
-
- Henderson B. W. & Dougherty T. J. How does photodynamic therapy work? Photochemistry and Photobiology 55(1), 145–157 (1992). - PubMed
-
- Fisher A. M., Murphree A. L. & Gomer C. J. Clinical and preclinical photodynamic therapy. Lasers Surg Med 17(1), 2–31 (1995). - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

