Complications with peripherally inserted central catheters (PICCs) used in hospitalized patients and outpatients: a prospective cohort study
- PMID: 28149507
- PMCID: PMC5273851
- DOI: 10.1186/s13756-016-0161-0
Complications with peripherally inserted central catheters (PICCs) used in hospitalized patients and outpatients: a prospective cohort study
Abstract
Background: Peripherally Inserted Central Catheters (PICCs) are widely used for hospitalized patients and among outpatients. Despite many advantages, PICC-related complications can occur such as infection, thrombosis or mechanical complications. We aimed to evaluate rates and nature of PICC-related complications from insertion to removal and analyze risk factors of complications at baseline and during healthcare.
Methods: We performed a prospective cohort study looking at PICC-related complication rates in the inpatient and outpatient settings of 163 patients over a 7-month period. Pertinent patient demographics as well as catheter-related factors were collected. The data were analyzed to identify catheter-related complications using univariate and multivariate analysis.
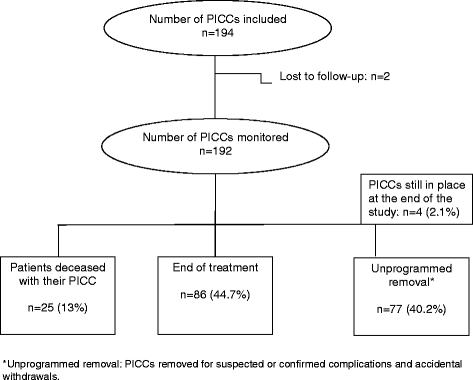
Results: One hundred ninety-two PICCs were monitored for a total of 5218 PICC-days (3337 PICC-days for inpatients, 1881 PICC-days for outpatients). The overall complication rate was 30.2% (11.1 per 1000 PICC-days) with a mean time to onset of 16.1 days. Complications included occlusion (8.9%), accidental withdrawal (8.9%), infections (6.3%) including 9 local infections (4.7%) and 3 bloodstream infections (1.6%), venous thrombosis (1.6%) and hematoma (1%). Complication rate was higher in the hospitalization setting (36.1%; 14.38 per 1000 PICC-days) than in the outpatient setting (19.4%; 3.19 per 1000 PICC-days). Multivariate logistic regression analysis showed that the occurrence of occlusion was significantly associated with an age > 65 years (OR = 4.19; 95% CI [1.1-15.81]) and the presence of a pre-occlusive event the week before PICC removal (OR = 76.35; 95% CI [9.36-622.97]).
Conclusions: PICCs appear safe in the inpatient and outpatient settings with low rates of infectious or thrombotic complications. Occlusion and accidental withdrawal were the most common complications, with age > 65 and catheter pre-occlusive event associated with an increased likelihood of catheter occlusion.
Keywords: Inpatient and outpatient settings; PICC-related complications; Prospective follow-up.
Figures
Similar articles
-
Risk of catheter-related bloodstream infection with peripherally inserted central venous catheters used in hospitalized patients.Chest. 2005 Aug;128(2):489-95. doi: 10.1378/chest.128.2.489. Chest. 2005. PMID: 16100130 Review.
-
Infectious complications of peripherally inserted central venous catheters in children.Pediatr Infect Dis J. 2010 May;29(5):426-9. doi: 10.1097/INF.0b013e3181c94d9e. Pediatr Infect Dis J. 2010. PMID: 20016395
-
Evaluation of PICC complications in orthopedic inpatients with bone infection for long-term intravenous antibiotics therapy.J Vasc Access. 2015 Jul-Aug;16(4):299-308. doi: 10.5301/jva.5000389. Epub 2015 Apr 27. J Vasc Access. 2015. PMID: 25953205
-
Peripherally inserted central catheter complications in neonates with upper versus lower extremity insertion sites.Adv Neonatal Care. 2013 Jun;13(3):198-204. doi: 10.1097/ANC.0b013e31827e1d01. Adv Neonatal Care. 2013. PMID: 23722492
-
Unveiling Peripherally Inserted Central Catheter Fractures and Related Complications in the Neonatal Intensive Care Unit: A Concise Review.Cureus. 2023 Oct 24;15(10):e47572. doi: 10.7759/cureus.47572. eCollection 2023 Oct. Cureus. 2023. PMID: 38021894 Free PMC article. Review.
Cited by
-
Ready-to-Use Multichamber Bags in Home Parenteral Nutrition for Patients with Advanced Cancer: A Single-Center Prospective Study.Nutrients. 2024 Feb 5;16(3):457. doi: 10.3390/nu16030457. Nutrients. 2024. PMID: 38337741 Free PMC article.
-
Clinical factors associated with peripherally inserted central catheters (PICC) related bloodstream infections: a single centre retrospective cohort.Antimicrob Resist Infect Control. 2023 Jan 30;12(1):5. doi: 10.1186/s13756-023-01209-z. Antimicrob Resist Infect Control. 2023. PMID: 36717942 Free PMC article.
-
Clinical study of complications of a peripherally inserted central catheter in cancer patients.Nurs Open. 2023 Jul;10(7):4480-4489. doi: 10.1002/nop2.1690. Epub 2023 Feb 28. Nurs Open. 2023. PMID: 36853924 Free PMC article.
-
Ultrasound-guided insertion of peripherally inserted central catheter after anesthetic induction in children undergoing surgery for moyamoya disease - Thirty cases report.Anesth Pain Med (Seoul). 2021 Jul;16(3):273-278. doi: 10.17085/apm.20099. Epub 2021 Jul 8. Anesth Pain Med (Seoul). 2021. PMID: 34233410 Free PMC article.
-
Performance and safety of PowerPICC catheters and accessories: a prospective observational study.BMJ Open. 2024 Sep 30;14(9):e081288. doi: 10.1136/bmjopen-2023-081288. BMJ Open. 2024. PMID: 39349374 Free PMC article.
References
-
- Mermel LA, Allon M, Bouza E, Craven DE, Flynn P, O’Grady NP, et al. Clinical practice guidelines for the diagnosis and management of intravascular catheter-related infection: 2009 Update by the Infectious Diseases Society of America. Clin Infect Dis. 2009;49(1):1–45. doi: 10.1086/599376. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources