Patient Characteristics, Management, and Predictors of Outcome from Severe Community-Onset Staphylococcal Sepsis in Northeast Thailand: A Prospective Multicenter Study
- PMID: 28167592
- PMCID: PMC5417193
- DOI: 10.4269/ajtmh.16-0606
Patient Characteristics, Management, and Predictors of Outcome from Severe Community-Onset Staphylococcal Sepsis in Northeast Thailand: A Prospective Multicenter Study
Abstract
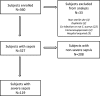
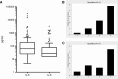
AbstractStaphylococcus aureus infection is a persistent threat in resource-restricted settings in southeast Asia but informative data about this disease remain limited. We analyzed characteristics, management, and predictors of outcome in severely septic patients with community-onset S. aureus infection in northeast Thailand. We performed a prospective, multicenter observational cohort study of community-onset S. aureus sepsis in four referral hospitals recruiting patients at least 14 years of age admitted between March 2010 and December 2013. One hundred and nineteen patients with severe staphylococcal sepsis were enrolled. Diabetes was the most common underlying condition. Methicillin-resistant infection was rare. Twenty-eight-day mortality was 20%. Ninety-two percent of patients received appropriate antibiotic therapy and 82% were administered intravenous fluids on the first hospital day, although only 14% were managed in an intensive care unit (ICU). On univariable analysis, clinical variables at enrollment significantly associated with death at 28 days were coagulopathy or respiratory failure. Plasma interleukin (IL)-8 concentration alone accurately predicted mortality (area under the receiver operating curve = 0.82, 95% confidence interval = 0.73-0.90). In multivariable analysis, addition of IL-8 concentration to a mortality prediction model containing clinical variables further improved the predictive ability of the model. We conclude that severe staphylococcal sepsis in northeast Thailand causes significant mortality. Diabetes is a common preexisting condition and most patients are managed outside the ICU even if they receive vasoactive/inotropic agents or mechanical ventilation. While clinical factors apparent on presentation including coagulopathy and respiratory failure predict death, plasma IL-8 improves this prediction.
Figures

References
-
- Nickerson EK, West TE, Day NP, Peacock SJ. Staphylococcus aureus disease and drug resistance in resource-limited countries in south and east Asia. Lancet Infect Dis. 2009;9:130–135. - PubMed
-
- Stoesser N, Moore CE, Pocock JM, An KP, Emary K, Carter M, Sona S, Poda S, Day N, Kumar V, Parry CM. Pediatric bloodstream infections in Cambodia, 2007 to 2011. Pediatr Infect Dis J. 2013;32:e272–e276. - PubMed
-
- Martin GS, Mannino DM, Eaton S, Moss M. The epidemiology of sepsis in the United States from 1979 through 2000. N Engl J Med. 2003;348:1546–1554. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

