Phenotypic and Genotypic Analysis of Multidrug-Resistant Mycobacterium tuberculosis Isolates from Sudanese Patients
- PMID: 28197340
- PMCID: PMC5286464
- DOI: 10.1155/2017/8340746
Phenotypic and Genotypic Analysis of Multidrug-Resistant Mycobacterium tuberculosis Isolates from Sudanese Patients
Abstract
Background. Currently, mutations in rpoB, KatG, and rrs genes and inhA promoter were considered to be involved in conferring resistance to rifampicin, isoniazid, and streptomycin in Mycobacterium tuberculosis (MTB). Objective. The aims of this study were to detect the prevalence of first-line tuberculosis (TB) drug resistance among a group of previously treated and newly detected TB patients, to determine the association between prevalence of multidrug resistance (MDR) and demographic information (age and sex), to explain genes correlated with MDR Mycobacterium tuberculosis, and to characterize MTB via 16S ribosomal RNA (16S rRNA) analysis. Methods. A hundred MTB isolates from Sudanese pulmonary TB patients were included in the study. The proportional method of drug susceptibility test was carried out on Löwenstein-Jensen media. Multiplex PCR of rpoB and KatG genes and inhA promoter was conducted; then rrs genes were amplified by conventional PCR and were sequenced. The sequences of the PCR product were compared with known rrs gene sequences in the GenBank database by multiple sequence alignment tools. Result. The prevalence of MDR was 14.7% among old cases and 5.3% among newly diagnosed cases. Conclusion. Mutations in rrs could be considered as a diagnostic marker.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
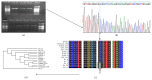
Similar articles
-
Prevalence of isoniazid resistance-conferring mutations associated with multidrug-resistant tuberculosis in Free State Province, South Africa.S Afr Med J. 2019 Aug 28;109(9):659-664. doi: 10.7196/SAMJ.2019.v109i9.13730. S Afr Med J. 2019. PMID: 31635590
-
Detection of mutations associated with isoniazid resistance in multidrug-resistant Mycobacterium tuberculosis clinical isolates.J Antimicrob Chemother. 2014 Sep;69(9):2369-75. doi: 10.1093/jac/dku161. Epub 2014 May 22. J Antimicrob Chemother. 2014. PMID: 24855126
-
Occurrence of disputed rpoB mutations among Mycobacterium tuberculosis isolates phenotypically susceptible to rifampicin in a country with a low incidence of multidrug-resistant tuberculosis.BMC Infect Dis. 2019 Jan 3;19(1):3. doi: 10.1186/s12879-018-3638-z. BMC Infect Dis. 2019. PMID: 30606116 Free PMC article.
-
Detection of novel and reported mutations in the rpoB, katG and inhA genes in multidrug-resistant tuberculosis isolates: A hospital-based study.J Glob Antimicrob Resist. 2015 Mar;3(1):1-4. doi: 10.1016/j.jgar.2014.10.002. Epub 2014 Nov 8. J Glob Antimicrob Resist. 2015. PMID: 27873643
-
Molecular characterization of multidrug-resistant Mycobacterium tuberculosis isolates from high prevalence tuberculosis states in Mexico.Infect Genet Evol. 2017 Nov;55:384-391. doi: 10.1016/j.meegid.2016.09.012. Epub 2016 Sep 13. Infect Genet Evol. 2017. PMID: 27637930
Cited by
-
Detection of several carbapenems resistant and virulence genes in classical and hyper-virulent strains of Klebsiella pneumoniae isolated from hospitalized neonates and adults in Khartoum.BMC Res Notes. 2020 Jul 1;13(1):312. doi: 10.1186/s13104-020-05157-4. BMC Res Notes. 2020. PMID: 32611369 Free PMC article.
-
First and Second-Line Anti-Tuberculosis Drug-Resistance Patterns in Pulmonary Tuberculosis Patients in Zambia.Antibiotics (Basel). 2023 Jan 12;12(1):166. doi: 10.3390/antibiotics12010166. Antibiotics (Basel). 2023. PMID: 36671366 Free PMC article.
-
Phenotypic and genotypic drug susceptibility patterns of Mycobacterium tuberculosis isolates from pulmonary tuberculosis patients in Central and Southern Ethiopia.PLoS One. 2023 Sep 8;18(9):e0285063. doi: 10.1371/journal.pone.0285063. eCollection 2023. PLoS One. 2023. PMID: 37682820 Free PMC article.
-
Drug Resistance Pattern of M. tuberculosis Complex in Oromia Region of Ethiopia.Infect Drug Resist. 2021 May 4;14:1679-1689. doi: 10.2147/IDR.S294559. eCollection 2021. Infect Drug Resist. 2021. PMID: 33976556 Free PMC article.
-
Whole-Genome Sequence of Multidrug-Resistant Methicillin-Resistant Staphylococcusepidermidis Carrying Biofilm-Associated Genes and a Unique Composite of SCCmec.Antibiotics (Basel). 2022 Jun 24;11(7):861. doi: 10.3390/antibiotics11070861. Antibiotics (Basel). 2022. PMID: 35884115 Free PMC article.
References
-
- World Health Organization. Global Tuberculosis Report 2015. 20th. chapter 4. Geneva, Switzerland: WHO/HTM/TB/2015.22; 2015.
-
- Mitchison D. A., Nunn A. J. Influence of initial drug resistance on the response to short-course chemotherapy of pulmonary tuberculosis. American Review of Respiratory Disease. 1986;133(3):423–430. - PubMed
-
- WHO. Global Tuberculosis Control 2014. Geneva, Switzerland: WHO; 2014. http://www.who.int/tb/publications/global_report/
-
- World Health Organization/IUATLD. Report. 3. Geneva, Switzerland: World Health Organization/IUATLD; 2003. Global project on anti-tuberculosis drug resistance surveillance.
LinkOut - more resources
Full Text Sources
Other Literature Sources

