Copeptin for risk stratification in non-traumatic headache in the emergency setting: a prospective multicenter observational cohort study
- PMID: 28197843
- PMCID: PMC5307398
- DOI: 10.1186/s10194-017-0733-2
Copeptin for risk stratification in non-traumatic headache in the emergency setting: a prospective multicenter observational cohort study
Abstract
Background: In the emergency setting, non-traumatic headache is a benign symptom in 80% of cases, but serious underlying conditions need to be ruled out. Copeptin improves risk stratification in several acute diseases. Herein, we investigated the value of copeptin to discriminate between serious secondary headache and benign headache forms in the emergency setting.
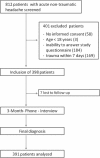
Methods: Patients presenting with acute non-traumatic headache were prospectively enrolled into an observational cohort study. Copeptin was measured upon presentation to the emergency department. Primary endpoint was serious secondary headache defined by a neurologic cause requiring immediate treatment of the underlying disease. Secondary endpoint was the combination of mortality and hospitalization within 3 months. Two board-certified neurologist blinded to copeptin levels verified the endpoints after a structured 3-month-telephone interview.
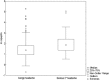
Results: Of the 391 patients included, 75 (19%) had a serious secondary headache. Copeptin was associated with serious secondary headache (OR 2.03, 95%CI 1.52-2.70, p < 0.0001). Area under the curve (AUC) for copeptin to identify the primary endpoint was 0.70 (0.63-0.76). After adjusting for age > 50, focal-neurological abnormalities, and thunderclap onset of symptoms, copeptin remained an independent predictive factor for serious secondary headache (OR 1.74, 95%CI 1.26-2.39, p = 0.001). Moreover, copeptin improved the AUC of the multivariate logistic clinical model (p-LR-test < 0.001). Even though copeptin values were higher in patients reaching the secondary endpoint, this association was not significant in multivariate logistic regression.
Conclusions: Copeptin was independently associated with serious secondary headache as compared to benign headaches forms. Copeptin may be a promising novel blood biomarker that should be further validated to rule out serious secondary headache in the emergency department.
Trial registration: Study Registration on 08/02/2010 as NCT01174901 at clinicaltrials.gov.
Keywords: Biomarker; Copeptin; Emergency; Head pain; Headache; Vasopressin.
Figures
References
-
- Schuetz P, Christ-Crain M, Wolbers M, Schild U, Thomann R, Falconnier C, Widmer I, Neidert S, Blum CA, Schonenberger R, Henzen C, Bregenzer T, Hoess C, Krause M, Bucher HC, Zimmerli W, Muller B, Pro Hsg Procalcitonin guided antibiotic therapy and hospitalization in patients with lower respiratory tract infections: a prospective, multicenter, randomized controlled trial. BMC Health Serv Res. 2007;7:102. doi: 10.1186/1472-6963-7-102. - DOI - PMC - PubMed
-
- Ang SH, Chan YC, Mahadevan M. Emergency department headache admissions in an acute care hospital:why do they occur and what can we do about it? Ann Acad Med Singapore. 2009;38:1007–1010. - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical