Menopausal Hormone Therapy Is Associated With Increased Risk of Fecal Incontinence in Women After Menopause
- PMID: 28209529
- PMCID: PMC5447480
- DOI: 10.1053/j.gastro.2017.02.005
Menopausal Hormone Therapy Is Associated With Increased Risk of Fecal Incontinence in Women After Menopause
Abstract
Background & aims: Low estrogen levels can contribute to development of fecal incontinence (FI) in women after menopause by altering neuromuscular continence mechanisms. However, studies have produced conflicting results on the association between menopausal hormone therapy (MHT) and risk of FI.
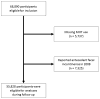
Methods: We studied the association between MHT and risk of FI among 55,828 postmenopausal women (mean age, 73 years) who participated in the Nurses' Health Study, were enrolled since 2008, and with no report of FI. We defined incident FI as a report of at least 1 liquid or solid FI episode per month during 4 years of follow-up from self-administered, biennial questionnaires administered in 2010 and 2012. We used Cox proportional hazard models to calculate multivariate-adjusted hazard ratios and 95% confidence intervals (CIs) for FI risk in women receiving MHT, adjusting for potential confounding factors.
Results: During more than 185,000 person-years of follow-up, there were 6834 cases of incident FI. Compared with women who never used MHT, the multivariate hazard ratio for FI was 1.26 (95% CI, 1.18-1.34) for past users of MHT and 1.32 (95% CI, 1.20-1.45) for current users. The risk of FI increased with longer duration of MHT use (P trend ≤ .0001) and decreased with time since discontinuation. There was an increased risk of FI among women receiving MHT that contained a combination of estrogen and progestin (hazard ratio, 1.37; 95% CI, 1.10-1.70) compared with estrogen monotherapy.
Conclusions: Current or past use of MHT was associated with a modestly increased risk of FI among postmenopausal women in the Nurses' Health Study. These results support a potential role for exogenous estrogens in the impairment of the fecal continence mechanism.
Keywords: Estrogen; Menopause; Motility; Progestin.
Copyright © 2017 AGA Institute. Published by Elsevier Inc. All rights reserved.
Figures
References
-
- Koloski NA, Jones M, Kalantar J, et al. Psychological impact and risk factors associated with new onset fecal incontinence. J Psychosom Res. 2012;73:464–8. - PubMed
-
- Ng KS, Sivakumaran Y, Nassar N, et al. Fecal Incontinence: Community Prevalence and Associated Factors--A Systematic Review. Dis Colon Rectum. 2015;58:1194–209. - PubMed
-
- Haadem K, Ling L, Ferno M, et al. Estrogen receptors in the external anal sphincter. Am J Obstet Gynecol. 1991;164:609–10. - PubMed
-
- Franz HB, Wendler D, Oettling G. Immunohistochemical assessment of steroid hormone receptors in tissues of the anal canal. Implications for anal incontinence? Acta Obstet Gynecol Scand. 1996;75:892–5. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous