A Frailty Index Based On Deficit Accumulation Quantifies Mortality Risk in Humans and in Mice
- PMID: 28220898
- PMCID: PMC5318852
- DOI: 10.1038/srep43068
A Frailty Index Based On Deficit Accumulation Quantifies Mortality Risk in Humans and in Mice
Abstract
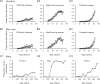
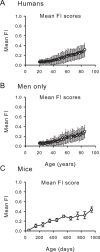
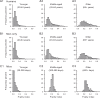
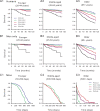
Although many common diseases occur mostly in old age, the impact of ageing itself on disease risk and expression often goes unevaluated. To consider the impact of ageing requires some useful means of measuring variability in health in animals of the same age. In humans, this variability has been quantified by counting age-related health deficits in a frailty index. Here we show the results of extending that approach to mice. Across the life course, many important features of deficit accumulation are present in both species. These include gradual rates of deficit accumulation (slope = 0.029 in humans; 0.036 in mice), a submaximal limit (0.54 in humans; 0.44 in mice), and a strong relationship to mortality (1.05 [1.04-1.05] in humans; 1.15 [1.12-1.18] in mice). Quantifying deficit accumulation in individual mice provides a powerful new tool that can facilitate translation of research on ageing, including in relation to disease.
Conflict of interest statement
The authors declare no competing financial interests.
Figures
References
-
- Vaupel J. W. et al.. Biodemographic trajectories of longevity. Science 280, 855–860 (1998). - PubMed
-
- Vaupel J. W., Mantron K. G. & Stallard E. The impact of heterogeneity in individual frailty on the dynamics of mortality. Demography 16, 439–454 (1979). - PubMed
-
- Saunderson et al.. Acute coronary syndrome management in older adults: guidelines, temporal changes and challenges. Age Ageing 43, 450–455 (2014). - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

