Neuro, trauma, or med/surg intensive care unit: Does it matter where multiple injuries patients with traumatic brain injury are admitted? Secondary analysis of the American Association for the Surgery of Trauma Multi-Institutional Trials Committee decompressive craniectomy study
- PMID: 28225527
- PMCID: PMC5481498
- DOI: 10.1097/TA.0000000000001361
Neuro, trauma, or med/surg intensive care unit: Does it matter where multiple injuries patients with traumatic brain injury are admitted? Secondary analysis of the American Association for the Surgery of Trauma Multi-Institutional Trials Committee decompressive craniectomy study
Abstract
Introduction: Patients with nontraumatic acute intracranial pathology benefit from neurointensivist care. Similarly, trauma patients with and without traumatic brain injury (TBI) fare better when treated by a dedicated trauma team. No study has yet evaluated the role of specialized neurocritical (NICU) and trauma intensive care units (TICU) in the management of TBI patients, and it remains unclear which TBI patients are best served in NICU, TICU, or general (Med/Surg) ICU.
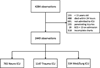
Methods: This study is a secondary analysis of The American Association for the Surgery of Trauma Multi-Institutional Trials Committee (AAST-MITC) decompressive craniectomy study. Twelve Level 1 trauma centers provided clinical data and head computed tomography (CT) scans of patients with Glasgow Coma Scale score of 13 or less and CT evidence of TBI. Non-ICU admissions were excluded. Multivariate logistic regression was performed to measure the association between ICU type and survival and calculate the probability of death for increasing Injury Severity Score (ISS). Multiple injuries patients (ISS > 15) with TBI and isolated TBI patients (other Abbreviated Injury Scale score < 3) were analyzed separately.
Results: There were 3641 patients with CT evidence of TBI with 2951 admitted to an ICU. Before adjustment, patient demographics, injury severity, and survival differed significantly by unit type. After adjustment, unit type, age, and ISS remained independent predictors of death. Unit type modified the effect of ISS on mortality. TBI multiple injuries patients admitted to a TICU had improved survival across increasing ISS. Survival for isolated TBI patients was similar between TICU and NICU. Med/surg ICU carried the greatest probability of death.
Conclusion: Multiple injuries patients with TBI have lower mortality risk when admitted to a trauma ICU. This survival benefit increases with increasing injury severity. Isolated TBI patients have similar mortality risk when admitted to a neuro ICU compared with a trauma ICU. Med/surg ICU admission carries the highest mortality risk.
Level of evidence: Therapeutic study, level IV.
Conflict of interest statement
Conflict of Interest: The authors have no financial conflicts of interest related to the content of this manuscript
Figures



References
-
- Centers for Disease Control and Prevention. Report to Congress on Traumatic Brain Injury in the United States: Epidemiology and Rehabilitation. Atlanta, GA: National Center for Injury Prevention and Control; Division of Unintentional Injury Prevention; 2015.
-
- English SW, Turgeon AF, Owen E, Doucette S, Pagliarello G, McIntyre L. Protocol management of severe traumatic brain injury in intensive care units: a systematic review. Neurocrit Care. 2013;18(1):131–142. - PubMed
-
- Fakhry SM, Trask AL, Waller MA, Watts DD. IRTC Neurotrauma Task Force. Management of brain-injured patients by an evidenced-based medicine protocol improves outcomes and decreases. J Trauma. 2004;56(3):492–499. - PubMed
-
- Arabi YM, Haddad S, Tamim HM, Al-Dawood A, Al-Qahtani S, Ferayan A, Al-Abdulmughni I, Al-Oweis J, Rugaan A. Mortality reduction after implementing a clinical practice guidelines-based management protocol for severe traumatic brain injury. J Crit Care. 2010;25:190–195. - PubMed
-
- Shafi S, Barnes SA, Millar D, Sobrino J, Kudyakov R, Berryman C, Rayan N, Dubiel R, Coimbra R, Magnotti LJ, et al. Suboptimal compliance with evidence-based guidelines inpatients with traumatic brain injuries. J Neurosurg. 2014;120(3):773–777. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

