Isoniazid-resistant tuberculosis: a cause for concern?
- PMID: 28234075
- PMCID: PMC5479083
- DOI: 10.5588/ijtld.16.0716
Isoniazid-resistant tuberculosis: a cause for concern?
Abstract
The drug isoniazid (INH) is a key component of global tuberculosis (TB) control programmes. It is estimated, however, that 16.1% of TB disease cases in the former Soviet Union countries and 7.5% of cases outside of these settings have non-multidrug-resistant (MDR) INH resistance. Resistance has been linked to poorer treatment outcomes, post-treatment relapse and death, at least for specific sites of disease. Multiple genetic loci are associated with phenotypic resistance; however, the relationship between genotype and phenotype is complex, and restricts the use of rapid sequencing techniques as part of the diagnostic process to determine the most appropriate treatment regimens for patients. The burden of resistance also influences the usefulness of INH preventive therapy. Despite seven decades of INH use, our knowledge in key areas such as the epidemiology of resistant strains, their clinical consequences, whether tailored treatment regimens are required and the role of INH resistance in fuelling the MDR-TB epidemic is limited. The importance of non-MDR INH resistance needs to be re-evaluated both globally and by national TB control programmes.
Conflict of interest statement
HRS declares funding from the National Institute for Health Research (NIHR), UK during the conduct of the study; and, outside of the submitted work, grants and personal fees from Otsuka Pharmaceutical, non-financial support from Sanofi, and other support from the WHO.
Figures
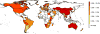
References
-
- Abubakar I, Zignol M, Falzon D, Raviglione M, Ditiu L, Masham S, Adetifa I, Ford N, Cox H, Lawn SD, Marais BJ, McHugh TD, Mwaba P, Bates M, Lipman M, Zijenah L, Logan S, McNerney R, Zumla A, Sarda K, Nahid P, Hoelscher M, Pletschette M, Memish ZA, Kim P, Hafner R, Cole S, Migliori GB, Maeurer M, Schito M, Zumla A. Drug-resistant tuberculosis: time for visionary political leadership. Lancet Infect Dis. 2013;13(6):529–39. - PubMed
-
- Meyer H, Mally J. Über Hydrazinderivate der Pyridincarbonsäuren. Monatshefte Chemie verwandte Teile anderer Wissenschaften. 1912;33(4):393–414.
-
- Crofton’s Clinical Tuberculosis. International Union Against Tuberculosis and Lung Disease. (Third) 2009
-
- Mitchison DA. Role of individual drugs in the chemotherapy of tuberculosis. Int J Tuberc Lung Dis. 2000;4(9):796–806. - PubMed
-
- World Health Organization. Treatment of tuberculosis: guidelines. (4th) 2009 http://www.who.int/tb/publications/2010/9789241547833/en/ Date last updated: 2009. Date last accessed: January 7 2013. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

