Can we predict fall asthma exacerbations? Validation of the seasonal asthma exacerbation index
- PMID: 28238748
- PMCID: PMC5568982
- DOI: 10.1016/j.jaci.2017.01.026
Can we predict fall asthma exacerbations? Validation of the seasonal asthma exacerbation index
Abstract
Background: A Seasonal Asthma Exacerbation Predictive Index (saEPI) was previously reported based on 2 prior National Institute of Allergy and Infectious Diseases Inner City Asthma Consortium trials.
Objective: This study sought to validate the saEPI in a separate trial designed to prevent fall exacerbations with omalizumab therapy.
Methods: The saEPI and its components were analyzed to characterize those who had an asthma exacerbation during the Preventative Omalizumab or Step-Up Therapy for Fall Exacerbations (PROSE) study. We characterized those inner-city children with and without asthma exacerbations in the fall period treated with guidelines-based therapy (GBT) in the absence and presence of omalizumab.
Results: A higher saEPI was associated with an exacerbation in both the GBT alone (P < .001; area under the curve, 0.76) and the GBT + omalizumab group (P < .01; area under the curve, 0.65). In the GBT group, younger age at recruitment, higher total IgE, higher blood eosinophil percentage and number, and higher treatment step were associated with those who had an exacerbation compared with those who did not. In the GBT + omalizumab group, younger age at recruitment, increased eosinophil number, recent exacerbation, and higher treatment step were also associated with those who had an exacerbation. The saEPI was associated with a high negative predictive value in both groups.
Conclusions: An exacerbation in children treated with GBT with or without omalizumab was associated with a higher saEPI along with higher markers of allergic inflammation, treatment step, and a recent exacerbation. Those that exacerbated on omalizumab had similar features with the exception of some markers of allergic sensitization, indicating a need to develop better markers to predict poor response to omalizumab therapy and alternative treatment strategies for children with these risk factors. The saEPI was able to reliably predict those children unlikely to have an asthma exacerbation in both groups.
Keywords: Fall asthma exacerbation; Seasonal Asthma Exacerbation Predictive Index (saEPI); asthma exacerbation predictors; guidelines-based therapy; omalizumab.
Copyright © 2017 American Academy of Allergy, Asthma & Immunology. All rights reserved.
Figures
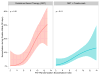

References
-
- Bloom B, Cohen RA, Freeman G. Summary health statistics for u.s. Children: national health interview survey, 2011. Vital and health statistics Series 10, Data from the National Health Survey. 2012:1–88. - PubMed
-
- Ivanova JI, Bergman R, Birnbaum HG, Colice GL, Silverman RA, McLaurin K. Effect of asthma exacerbations on health care costs among asthmatic patients with moderate and severe persistent asthma. The Journal of allergy and clinical immunology. 2012;129:1229–35. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- UM1 AI109565/AI/NIAID NIH HHS/United States
- UL1 TR000150/TR/NCATS NIH HHS/United States
- UL1 TR001105/TR/NCATS NIH HHS/United States
- UL1 TR000075/TR/NCATS NIH HHS/United States
- UL1 RR025780/RR/NCRR NIH HHS/United States
- UM2 AI117870/AI/NIAID NIH HHS/United States
- UL1 TR001422/TR/NCATS NIH HHS/United States
- UL1 TR001082/TR/NCATS NIH HHS/United States
- HHSN272200900052C/AI/NIAID NIH HHS/United States
- HHSN272201000052I/AI/NIAID NIH HHS/United States
- UL1 TR000154/TR/NCATS NIH HHS/United States
- R01 AI098077/AI/NIAID NIH HHS/United States
- UL1 TR000451/TR/NCATS NIH HHS/United States
- UM1 AI114271/AI/NIAID NIH HHS/United States
- UL1 TR000040/TR/NCATS NIH HHS/United States
- UL1 TR000077/TR/NCATS NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

